One of the most challenging denial scenarios in medical billing is when a claim is rejected because the procedure, treatment, or drug is considered experimental or investigational by the insurance payer. This type of denial can significantly impact reimbursement and requires a strategic approach to resolve.
If you’re new to denial management or want to refine your workflow, this guide will walk you through the process step by step in simple, practical terms.
What Does “Experimental/Investigational” Mean?
Insurance companies label a service as experimental or investigational when:
It is not widely accepted in the medical community
It lacks sufficient clinical evidence
It is not included in the payer’s approved coverage policies
It is considered under research or trial phase
Example:
A newly developed surgical technique or a recently approved drug may not yet be covered by all insurance plans.
Why Do These Denials Happen?
Understanding the root cause helps you decide the next step.

Common Reasons:
CPT code not recognized as standard treatment
Lack of supporting documentation
Missing prior authorization
Payer-specific policy exclusions
Incorrect coding or outdated code usage
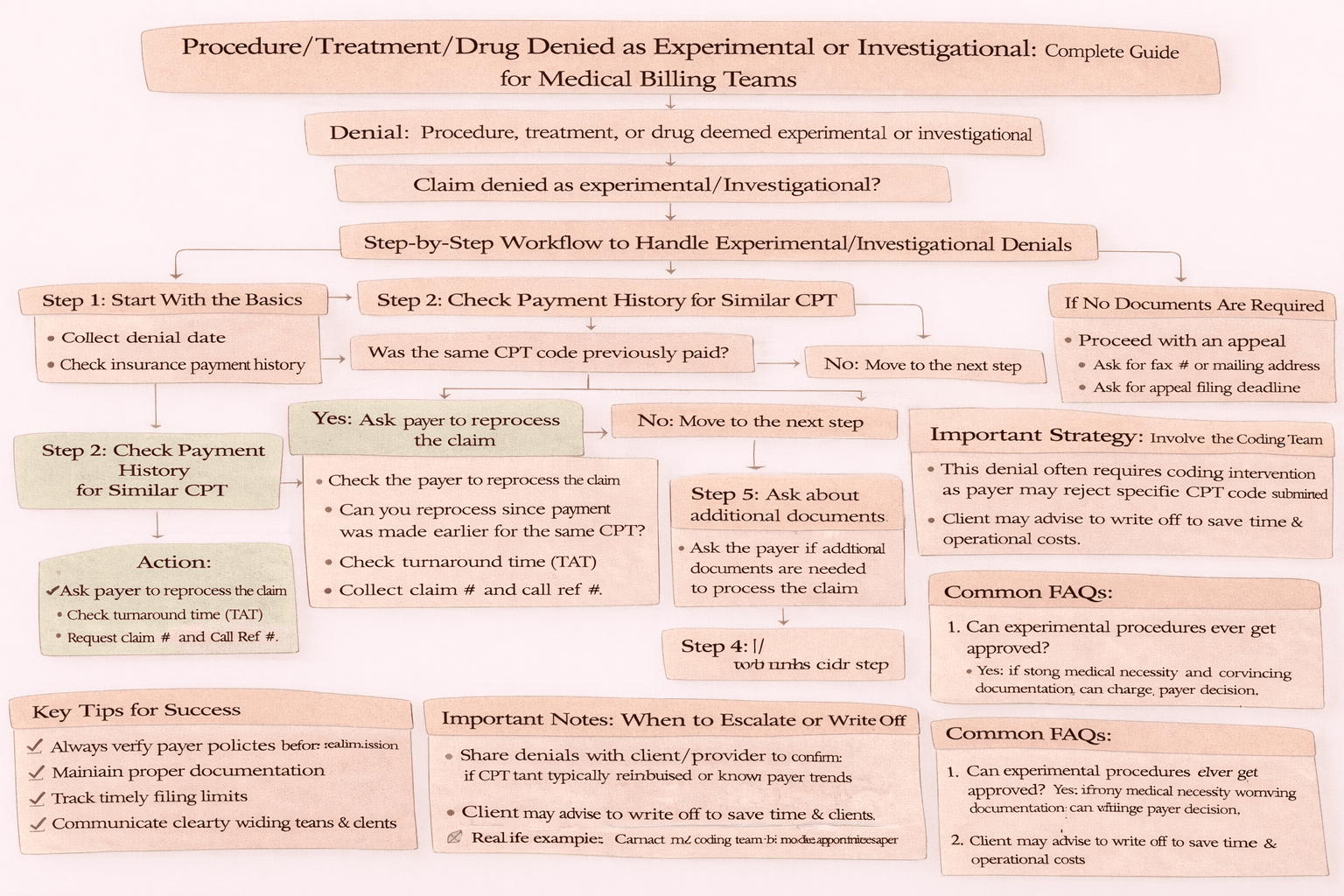
Step-by-Step Workflow to Handle This Denial
1. Start With the Basics
Ask for the denial date and verify details in the insurance payment history.
2. Check Payment History for Similar CPT
If the same CPT was previously paid:
Request the payer to reprocess the claim
Ask if they can reprocess since payment was made earlier for the same CPT
Check the turnaround time
Collect claim number and call reference number

If the CPT was not previously paid:
Move to the next step
3. Ask About Additional Requirements
Ask the payer if any additional documentation is required to process the claim.
4. If Additional Documents Are Required
Clarify what documents are needed such as clinical notes, medical necessity documentation, or lab reports.
Confirm the submission time limit.
Submit the documents within the timeframe and record claim number and call reference number.
5. If No Documents Are Required
Proceed with an appeal.
Ask for fax number or mailing address and the appeal filing deadline.
Prepare and submit the appeal and document claim number and call reference number.
Important Strategy: Involve the Coding Team
This denial often requires coding intervention because the payer may not accept the submitted CPT code.
Send the case to the coding team and request an alternate CPT code if applicable.
If an alternate CPT is provided:
Update and resubmit the claim
If no alternate CPT is available:
Follow payer guidance to submit documents or file an appeal
When to Escalate or Write Off
Not all claims should be pursued indefinitely.
Share such denials with the client or provider and confirm whether the CPT is typically reimbursed or if there are known payer trends.
In some cases, the client may advise a direct write off to save time and operational costs.
Key Tips for Success
Always verify payer policies before resubmission
Maintain proper documentation
Track timely filing limits
Communicate clearly with coding teams and clients
Avoid repeated submissions without correction
Real-Life Example
A claim for a new therapy procedure is denied as investigational.
Actions taken:
Checked history and found no prior payments
Contacted payer and confirmed no documents were required
Sent case to coding and no alternate CPT was available
Filed an appeal with medical necessity documentation
Client later confirmed the payer does not cover this CPT
Final outcome:
Claim written off
FAQs
1. Can experimental procedures ever get approved?
Yes, if strong medical necessity and proper documentation are provided, the payer may reconsider.
2. What documents help in appeals?
Physician notes, clinical studies, treatment justification, and prior treatment history.
3. How long do appeals usually take?
Typically around 30 to 60 days depending on the payer.
4. Should I always send the claim to coding?
Yes, this denial type requires coding review to check for alternate billable CPTs.
5. What if the payer repeatedly denies the same CPT?
Escalate internally, inform the client, and consider write off if it is confirmed non payable.
Conclusion
Denials related to experimental or investigational procedures can be complex and time consuming. However, by following a structured workflow, verifying payment history, coordinating with coding teams, understanding payer requirements, and involving clients, you can handle these effectively.
The key is to avoid unnecessary rework and focus on informed decisions and timely action to improve reimbursement outcomes and overall efficiency.