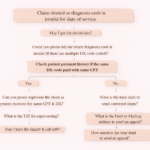
In medical billing and revenue cycle management, denial codes can be confusing, especially for beginners. One of the most common adjustment-related denials is Code 45, which indicates that a charge exceeds the allowable or contracted amount.
If not handled properly, this denial can lead to revenue loss or compliance issues. This guide explains what Denial Code 45 means and how to handle it in different scenarios.
What is Denial Code 45?
Denial Code 45 means the charge exceeds the fee schedule, maximum allowable, or contracted amount.
In simple terms, the provider billed more than what the insurance payer allows for a specific service, and the extra amount is not payable.
Understanding CO-45 vs PR-45
CO-45 (Contractual Obligation)
The denied amount is written off as a provider adjustment.
It cannot be billed to the patient.
Common for in-network providers.
PR-45 (Patient Responsibility)
The denied amount is assigned to the patient.
Do not bill the patient immediately without verification.
Often occurs in out-of-network or benefit-related scenarios.
Why Does Denial Code 45 Occur?
Charges exceed payer fee schedule
Incorrect contracted rate setup
Outdated or incorrect CPT pricing
Out-of-network billing
System configuration issues
How to Work on Denial Code 45 (Step-by-Step)
Scenario 1: Claim is Processed and Paid
What happens
Insurance processes the claim and pays a portion while the remaining amount shows as CO-45.
What it means
The denied amount is a contractual adjustment.
What to do
Verify allowed amount versus billed amount
Confirm payer contract terms
Post adjustment in billing system if authorized
Example
Billed amount ₹5000
Allowed amount ₹3500
CO-45 adjustment ₹1500
Action: Adjust ₹1500 as contractual write-off
Scenario 2: Claim is Denied with Multiple Codes
What happens
CO-45 appears along with other denial codes.
What it means
CO-45 is not the main issue.
What to do
Focus on primary denial codes such as missing information or eligibility issues
Correct them and resubmit the claim
Example
CO-45 with CO-16
Action: Fix CO-16 first and resubmit
Scenario 3: Claim is Denied with Only CO-45
What happens
No payment is made and only CO-45 appears.
What it means
There may be incorrect claim processing.
What to do
Do not assume it is just an adjustment
Contact the payer and verify fee schedule, contract rates, and processing details
Request reprocessing or file an appeal if needed
Scenario 4: PR-45 Denial
What happens
The amount is assigned to patient responsibility.
Important
Do not bill the patient immediately.
What to do
Verify with payer and client or provider policy
Check network status
Confirm if patient truly owes the amount
Example
PR-45 shows ₹2000
Action: Verify before billing patient
Key Tips for Handling Denial Code 45
Always verify payer contracts and fee schedules
Understand the difference between adjustment and denial
Do not bill patients without confirmation in PR-45 cases
Ensure correct system configuration
Communicate with payers and document all details
Common Mistakes to Avoid
Writing off PR-45 without verification
Billing patients incorrectly
Ignoring primary denial codes
Assuming all CO-45 are simple adjustments
Not checking payer contracts
FAQs
1. Is Denial Code 45 always a write-off?
No, CO-45 is usually a write-off, but if it appears alone, verify before adjusting.
2. Can I bill the patient for PR-45?
Not immediately. Always confirm with payer and client before billing.
3. Why does CO-45 appear after payment?
Because the billed amount exceeded the allowed amount, and the excess is adjusted.
4. How can I prevent Denial Code 45?
Use updated fee schedules, verify contracts, and ensure correct charge entry.
5. What if the allowed amount seems incorrect?
Contact the payer and request review or file an appeal.
Conclusion
Denial Code 45 is one of the most common adjustments in medical billing, but it must be handled carefully to avoid revenue loss or compliance issues. The key is understanding the difference between CO-45 and PR-45, identifying the correct scenario, and taking appropriate action.
The most important rule is to verify first and adjust later. By following a structured process and maintaining accurate data, you can handle this denial effectively and confidently.