In medical billing, hospice-related denials—commonly referred to as B9 denials (Patient Enrolled in Hospice)—are a frequent challenge. These denials occur when claims are incorrectly billed while a patient is under hospice care. Understanding hospice rules, billing responsibilities, and the correct use of modifiers is essential to avoid revenue loss and rework.
This guide explains hospice eligibility, billing workflows, denial reasons, and step-by-step resolution strategies in a simple and practical way—ideal for beginners and experienced billers alike.
What Is Hospice Care?
Hospice care is a type of medical support provided to patients who are nearing the end of life. Instead of focusing on curing the illness, hospice prioritizes comfort, pain relief, and quality of life.
When Is a Patient Eligible for Hospice?
A patient qualifies for hospice if:
They are diagnosed with a terminal illness with a life expectancy of 6 months or less, OR
They choose to decline curative treatment due to its risks or severity and still have a limited life expectancy
Key Feature of Hospice Care
Treatment shifts from curative care → palliative care (comfort-based)
Services are typically coordinated and managed by a hospice provider
How Hospice Affects Medical Billing
Once a patient elects hospice care:
All hospice-related services must be billed to the hospice provider, not Medicare Part B
The patient waives rights to Medicare Part B payments for services related to the terminal condition
Only non-hospice-related services can be billed separately
This is where billing errors commonly occur.
Understanding B9 Denial (Patient Enrolled in Hospice)
A B9 denial indicates that the claim was rejected because the patient was enrolled in hospice during the Date of Service (DOS).
Common Reasons for B9 Denial
Claim billed to Medicare Part B instead of hospice
Missing GV or GW modifier
Services related to hospice condition billed incorrectly
Incorrect payer submission (e.g., billed to commercial insurance)
Key Modifiers in Hospice Billing

- GV Modifier
Use when:
The service is related to the hospice condition
Provided by an attending physician NOT employed by hospice
Bill to Medicare Part B with GV modifier - GW Modifier
Use when:
The service is NOT related to the hospice diagnosis
Bill to Medicare Part B with GW modifier
Quick Tip
ScenarioWhere to BillModifierHospice-related service (hospice-employed provider)HospiceNoneHospice-related service (non-hospice physician)MedicareGVNon-hospice-related serviceMedicareGW
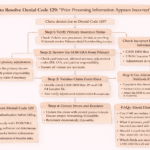
Step-by-Step Denial Handling Process
Here’s a simplified workflow to resolve hospice denials effectively:
Step 1: Identify the Denial
Confirm: “Patient enrolled in hospice”
Step 2: Verify Key Dates
Ask for:
Denial date
Hospice enrollment start & end dates
Step 3: Check Date of Service (DOS)
Case 1: DOS Outside Hospice Period
Request claim reprocessing
Set follow-up based on TAT (Turnaround Time)
Case 2: DOS Within Hospice Period
Request:
Hospice name
NPI
Mailing address
Policy ID
What If Information Is Missing?
Sometimes, insurance representatives provide limited data.
Here’s What You Can Do:
Use NPI lookup tools (like NPPES) to find hospice details
Check Medicare portals for hospice enrollment information
Use SSN as policy ID if applicable
Special Scenarios to Handle Carefully
- No Hospice Information Available
Follow client-specific guidelines
Option: Release claim to patient - Commercial Insurance Denial
Do NOT rebill commercial insurance
Redirect claim to:
Hospice provider, OR
Medicare (if appropriate with modifiers)
Example Scenario
Situation:
A patient receives a physician visit during hospice enrollment.
Incorrect Billing:
Claim sent to Medicare without modifier → Denied
Correct Billing:
If related and physician not hospice-employed → Use GV modifier
If unrelated → Use GW modifier
Key Tips to Avoid Hospice Denials
Always verify hospice enrollment before billing
Cross-check DOS against hospice period
Use correct modifiers (GV/GW)
Maintain updated payer and hospice information
Document communication with insurance reps (Claim #, Call Ref #)
FAQs
- What does B9 denial mean in medical billing?
It indicates that the patient was enrolled in hospice during the service date, and the claim was billed incorrectly. - Can Medicare be billed during hospice care?
Yes, but only:
With GV modifier (related services by non-hospice physician)
With GW modifier (unrelated services) - What happens if I bill hospice-related services to Medicare?
The claim will be denied because hospice should be billed instead. - How do I find hospice provider details?
You can use:
NPI lookup tools (NPPES)
Medicare portal
Information from insurance representatives - Should I rebill commercial insurance for hospice patients?
No. Claims must be redirected to hospice or Medicare, not commercial insurance.
Conclusion:
Handling Patient Enrolled in Hospice (B9) denials requires a clear understanding of hospice rules, billing pathways, and modifier usage. The key is verifying hospice enrollment and aligning billing accordingly.
By following structured workflows, using correct modifiers, and gathering accurate hospice information, you can significantly reduce denials and improve claim success rates.
Mastering hospice billing isn’t just about compliance—it’s about ensuring patients receive appropriate care while providers get reimbursed correctly.