In medical billing, claim denials are common—but some are easier to resolve than others. One such denial is MA120, which indicates a missing, incomplete, or invalid CLIA certification number. This issue typically arises when laboratory services are billed without proper compliance details.
If you’re new to healthcare billing or struggling to resolve MA120 denials efficiently, this guide breaks everything down into simple, actionable steps. By the end, you’ll understand what CLIA is, why it matters, and exactly how to fix and prevent this denial.
What is a CLIA Number?
CLIA stands for Clinical Laboratory Improvement Amendments. It is a federal regulatory standard in the United States that ensures quality and accuracy in laboratory testing.
A CLIA number is:
A unique identifier assigned to certified laboratories
Required for billing lab-related services
Mandatory for claims involving diagnostic tests
Without a valid CLIA number, insurance payers cannot verify whether the lab meets regulatory standards—leading to claim rejection or denial.
What Does MA120 Denial Mean?
The MA120 denial code indicates:
“Missing/incomplete/invalid CLIA certification number.”
Common Causes:
CLIA number missing from the claim (Box 23 in CMS-1500 form)
Incorrect or expired CLIA number
CLIA number not matching the billing provider
System or clearinghouse omission
Lab not CLIA-certified
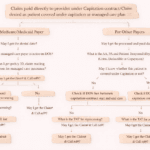
Step-by-Step Process to Resolve MA120 Denial
Here’s a simplified workflow you can follow:
- Verify the Denial Details
Start by collecting basic information:
Denial date
Claim number
Payer details
This helps track and reference your case during follow-ups. - Check if CLIA Number Was Submitted
Review:
Box 23 of the claim form
Billing software or clearinghouse records
If CLIA Number is Present:
Confirm with the payer if the number is correct and valid
If CLIA Number is Missing:
Proceed to identify and obtain the correct CLIA number
- Validate the CLIA Number
If the number exists:
Ask the payer representative:
“Can you confirm if the CLIA number submitted is correct?”
Outcomes:
Correct → Request claim reprocessing
Incorrect → Ask for the correct CLIA number
- If Payer Provides Correct CLIA Number
Take the following steps:
Update the CLIA number in your billing system
Resubmit the corrected claim
Also ask:
What is the timely filing limit (TFL) for corrected claims?
- If Payer Refuses to Provide CLIA Number
You will need to find it manually using official databases:
Search Using:
Laboratory name
Facility address
Existing CLIA number (if partial info available)
Tips:
Some facilities have multiple CLIA numbers
Always match the correct address and lab location
- Unable to Find CLIA Number?
If the lab is not listed:
It may not be CLIA-certified
Escalate the issue to your client or supervisor - Request Claim Reprocessing or Resubmission
Depending on the situation:
Reprocessing: If error was on payer’s side
Corrected claim: If data needs updating
Always document:
Call reference number
Representative name
Instructions given
Important Notes to Remember
CLIA + QW Modifier
For CLIA-waived tests, you must:
Include the QW modifier
Add the CLIA number
Failure to include both can trigger MA120 denial.
When to Escalate
Assign the case to your client if:
You don’t have system access to update CLIA
CLIA number cannot be located
Facility is not certified
Key Tips to Prevent MA120 Denials
Preventing this denial is far easier than fixing it. Here’s how:
Always Verify Before Submission
Ensure CLIA number is populated in Box 23
Validate accuracy with internal records
Maintain Updated Records
Keep a database of CLIA numbers by facility
Regularly audit for expired or inactive certifications
Use Automation Tools
Configure billing software to flag missing CLIA entries
Train Billing Staff
Educate teams on:
When CLIA is required
How to verify it
Double-Check Modifiers
Always attach QW modifier for waived tests
Example Scenario
Situation:
A lab test claim gets denied with MA120.
Action Taken:
Checked claim → CLIA missing
Searched lab in database → Found correct CLIA
Updated claim → Resubmitted
Claim paid successfully
Lesson:
Simple verification upfront could have avoided delay.
Frequently Asked Questions (FAQs)
- What is the purpose of a CLIA number?
It ensures that laboratories meet federal quality standards for testing accuracy and reliability. - Where is the CLIA number entered in a claim?
In Box 23 of the CMS-1500 claim form. - Can a facility have more than one CLIA number?
Yes. Larger organizations or multi-location labs often have multiple CLIA certifications. - What happens if a lab is not CLIA-certified?
Claims for lab services will be denied, and the issue must be escalated for compliance review. - Is the QW modifier always required?
No. It is only required for CLIA-waived tests.
Conclusion:
The MA120 denial is a straightforward but critical issue tied to compliance. Missing or incorrect CLIA numbers can delay payments and disrupt revenue cycles—but with a structured approach, they are easy to resolve.
By verifying claims before submission, maintaining accurate records, and understanding the role of CLIA certification, you can significantly reduce these denials. When issues do arise, following a clear workflow ensures faster resolution and minimal disruption.
Staying proactive is the key—because in medical billing, accuracy isn’t optional, it’s essential.