In medical billing, claim denials are a common challenge—but many of them are preventable. One such frequent denial is Denial Code 197, which occurs when precertification, authorization, or notification is missing for a service that requires it.
If you’re new to healthcare billing or revenue cycle management, this topic may sound technical. Don’t worry—this guide breaks it down into simple terms. You’ll learn what Denial 197 means, why it happens, and exactly how to handle it step by step.
What is Denial Code 197?
Denial Code 197 is issued when an insurance payer rejects a claim because prior authorization was not obtained before the service was performed.
In simple terms:
The insurance company is saying:
“You should have asked for approval before doing this procedure.”
Types of Authorization
Understanding the different types of authorization helps prevent this denial.
- Prior Authorization (Pre-Authorization)
Approval obtained before performing a procedure
Required for expensive or specialized treatments
Ensures medical necessity - Retro Authorization
Requested after the service is already performed
Typically allowed only in specific situations (like emergencies)
Where to Find Authorization Details
Authorization numbers are usually documented in:
CMS-1500 Form → Box 23
UB-04 Form → Locator 63
Always verify these fields before claim submission.
Common Reasons for Denial 197
Here are the most frequent causes:
Authorization was never requested
Authorization was obtained but not added to the claim
Invalid or incorrect authorization number
Service performed by an out-of-network provider
Procedure performed outside the authorized timeframe
Emergency services not properly documented
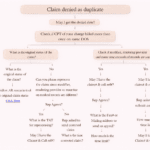
Step-by-Step Process to Handle Denial 197
Handling this denial requires a structured approach. Below is a simplified workflow.
Step 1: Verify Denial Details
Call the insurance representative
Ask for:
Denial date
Reason for denial
Step 2: Check If Authorization Exists
If Authorization is Available:
Provide the authorization number to the payer
Request claim reprocessing
If approved:
Ask for turnaround time (TAT)
Note claim reference number
If denied:
Submit a corrected claim
Ensure:
Correct authorization number is included
Use correct billing frequency code (e.g., “7” for replacement claims)
If Authorization is NOT Available:
Now evaluate further.
Step 3: Check Place of Service
If Emergency Service (POS 23):
Emergency services often do not require prior authorization
Request payer to reprocess claim
If approved:
Note TAT and follow up
If NOT Emergency:
Check the following:
Step 4: Look for Authorization Elsewhere
Ask:
Does the payer system show authorization?
Is there a hospital claim with authorization for the same date of service?
If YES:
Request reprocessing using that authorization
Step 5: Request Retro Authorization
If no authorization exists:
Ask if retro authorization is possible
If YES:
Follow payer instructions:
Fill required forms
Attach medical records
Submit within deadline
If NO:
Two options:
Write off the claim
File an appeal (based on client instructions)
Special Tip: Use Evicore Portal
Some insurance providers use Evicore for authorization tracking.
You can:
Check if authorization exists for a CPT code
Verify approval period
Contact Evicore if needed
This can save time and avoid unnecessary appeals.
Key Tips to Prevent Denial 197
Prevention is always better than rework. Follow these best practices:
Before Billing:
Verify if authorization is required
Obtain authorization before scheduling procedure
Double-check CPT codes match authorization
During Claim Submission:
Enter correct authorization number
Ensure it matches payer records
Check date validity
After Submission:
Monitor claims regularly
Act quickly on rejections
Example Scenario
Case:
A patient undergoes an MRI scan.
What went wrong:
Authorization was required but not obtained.
Outcome:
Claim denied with Code 197.
Resolution:
Billing team contacts payer
Requests retro authorization
Submits medical records
Claim is reprocessed and paid
Frequently Asked Questions (FAQs)
- What is the main cause of Denial 197?
The primary reason is missing prior authorization for services that require approval. - Can emergency services be denied under Code 197?
Yes, but often incorrectly. Emergency services usually do not require authorization, and claims can be reprocessed upon clarification. - What if the authorization number is incorrect?
You must submit a corrected claim with the valid authorization number. - Is retro authorization always possible?
No. It depends on the payer’s policy. Some allow it under specific conditions, while others do not. - When should a claim be written off?
If:
Authorization is not available
Retro authorization is denied
Appeal is unsuccessful
Then the claim may need to be written off (based on client policy).
Conclusion:
Denial Code 197 is one of the most common yet preventable claim denials in medical billing. It mainly occurs due to missing or incorrect authorization. By understanding the authorization process, verifying details before submission, and following a structured denial management workflow, you can significantly reduce revenue loss.
The key takeaway is simple:
Always verify authorization before providing services—and document it correctly.
With consistent checks, proper communication, and timely follow-ups, handling Denial 197 becomes much more manageable—even for beginners.








