In medical billing and revenue cycle management, denial codes can slow down payments and disrupt cash flow if not handled properly. One such common denial is Denial Code 129, which indicates that prior processing information appears incorrect. This denial typically arises when a claim is submitted to a secondary or tertiary insurance payer and there is an issue with how the primary insurance details were reported. If you’re new to denial management, this guide explains the causes and how to fix them in a simple and structured way.
What Is Denial Code 129?
Denial Code 129 means that the secondary insurance company cannot process the claim because the information about the primary insurance processing is missing, incorrect, or inconsistent. In simple terms, the secondary payer does not accept or cannot validate the primary insurance details submitted.
Why Does Denial Code 129 Occur?
There are two primary reasons for this denial.
1. Primary Insurance Did Not Process the Claim
Secondary insurance requires that the primary insurance processes the claim first. Only the remaining balance is sent to secondary.
Example:
Total charge ₹8,000
Primary allowed ₹8,000
Primary paid ₹6,400
Patient responsibility ₹1,600
In this case, the secondary insurance can process ₹1,600. However, if the primary denies the claim completely, the secondary will also deny it with Code 129 because it depends on primary adjudication.
2. Incorrect Primary Payment Information Submitted
Even if primary processed the claim, denial 129 can occur if payment details are missing, incorrect, or not properly reported.
Where to check:
CMS 1500 Form Box 29 for amount paid
UB 04 Form Locator 54 for prior payments
If these fields are blank, incorrect, or do not match the EOB or ERA, the secondary payer will reject the claim.
Step-by-Step Guide to Resolve Denial Code 129
Here is a simple workflow to resolve this denial.
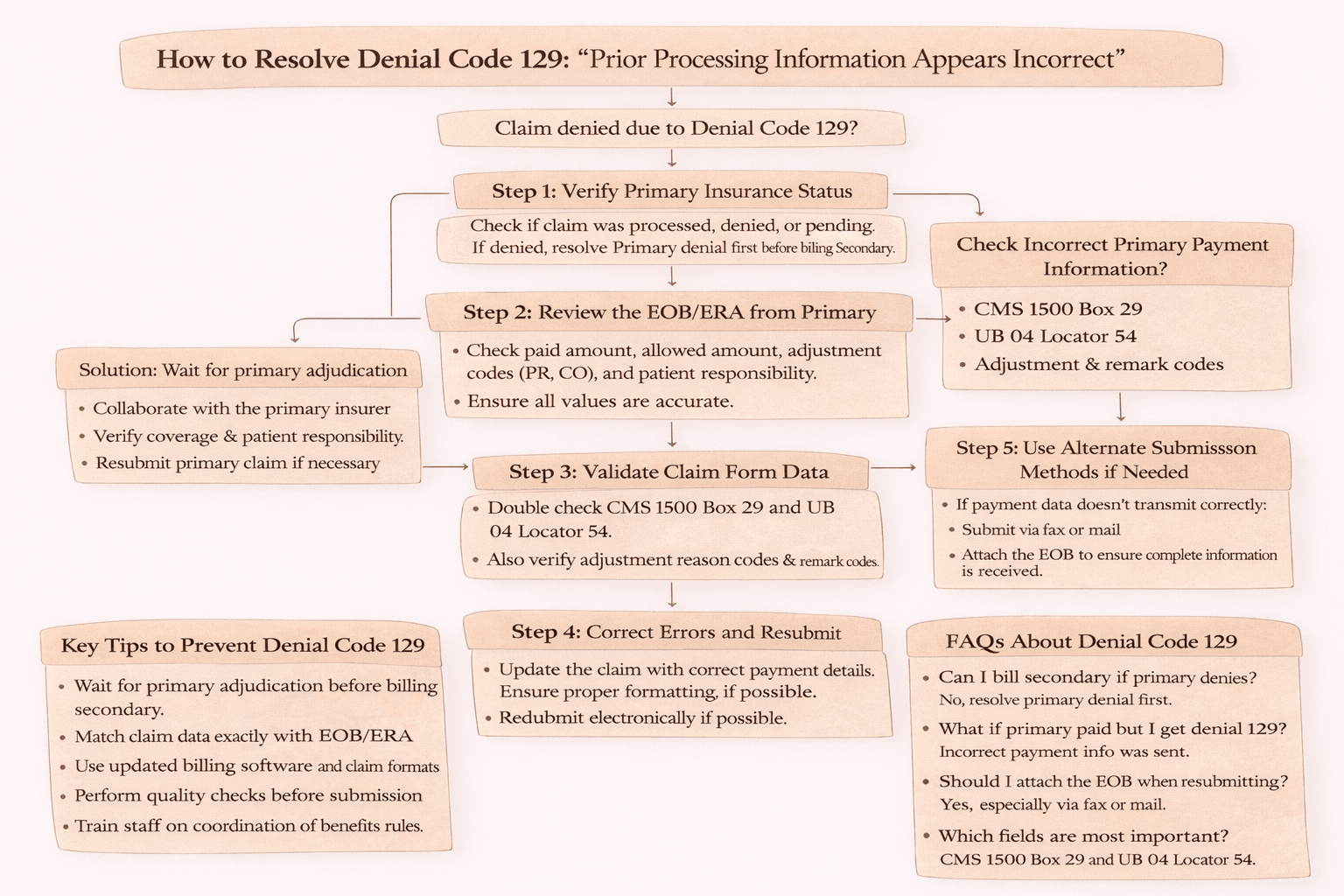
Step 1: Verify Primary Insurance Status
Check whether the claim was processed, denied, or pending. If denied, fix the primary denial first before billing secondary.
Step 2: Review the EOB or ERA from Primary
Check paid amount, allowed amount, adjustment codes such as PR or CO, and patient responsibility. Ensure all values are accurate.
Step 3: Validate Claim Form Data
Double check CMS 1500 Box 29 and UB 04 Locator 54. Also verify claim adjustment reason codes and remittance remark codes.
Step 4: Correct Errors and Resubmit
Update the claim with correct payment details, ensure proper formatting, and resubmit electronically if possible.
Step 5: Use Alternate Submission Methods if Needed
If payment data is not transmitting correctly, submit via fax or mail with EOB attached to ensure the payer receives complete information.
Special Scenarios to Watch For
In some cases, even if primary denies, secondary may still pay for non covered services or patient responsibility denials. This depends on the patient’s policy and coordination of benefits rules.
Common Mistakes That Trigger Denial 129
Missing primary payment amount
Incorrect adjustment codes
Mismatch between EOB and claim data
Billing secondary before primary processing
Not attaching EOB when required
Key Tips to Prevent Denial Code 129
Always wait for primary adjudication before billing secondary
Match claim data exactly with EOB or ERA
Use updated billing software and claim formats
Perform quality checks before submission
Train staff on coordination of benefits rules
FAQs About Denial Code 129
1. Can I bill secondary insurance if primary denies the claim?
No, in most cases you must resolve the primary denial first.
2. What if the primary paid but I still get denial 129?
This usually means incorrect or missing payment information was submitted.
3. Do I need to attach the EOB when resubmitting?
Yes, especially for fax or mail submissions or when required by the payer.
4. Which fields are most important?
CMS 1500 Box 29 and UB 04 Locator 54 must accurately reflect primary payment details.
5. Can software errors cause this denial?
Yes, billing systems may fail to populate payment fields correctly, so always validate before submission.
Conclusion
Denial Code 129 is mainly a coordination of benefits issue rather than a complex coding problem. It usually occurs due to lack of primary insurance processing or incorrect reporting of primary payment details. By verifying primary adjudication, ensuring accurate data entry, and resubmitting claims correctly, you can resolve this denial efficiently. A structured approach and attention to detail will help reduce rejections and improve reimbursement timelines while strengthening your overall denial management process.