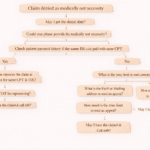
Medical billing denials are a common challenge in revenue cycle management, and Denial Code 150 is one of the more frequently encountered issues. This denial indicates that the payer believes the documentation submitted does not justify the level of service billed.
For beginners, this can be confusing, but once you understand the cause, it becomes easier to resolve and prevent.
What Is Denial Code 150?
Denial Code 150 means the payer believes the submitted information does not support the level of service billed.
In simple terms:
The documentation does not justify the CPT code, or
The service level billed is higher than what the records support
This denial is commonly seen in evaluation and management services, procedures, and time-based billing.
Common Reasons for Denial Code 150
1. CPT Code Has Reached Maximum Allowance
Some services have limits within a specific timeframe.
Examples include therapy sessions exceeding allowed visits or repeated tests within a short period.
The payer denies additional claims once the limit is reached.
2. Medical Necessity or Coding Issue
This is the most common reason.
Issues may include diagnosis not supporting the procedure, incorrect CPT or modifier usage, or upcoding.
Example
A higher-level visit is billed, but documentation only supports a lower-level visit.
3. Medical Records Requested
The payer may require more information before processing the claim.
This usually happens for complex or high-cost services or when documentation is insufficient.
The claim may be denied or held until records are reviewed.
Importance of Remark Codes
Always check the remark codes in the EOB or ERA.
They provide specific reasons for the denial and guide the next steps such as submitting records or correcting coding.
Never assume the reason without reviewing these codes.
Step-by-Step Process to Handle Denial Code 150
Step 1: Review Denial Details
Check EOB or ERA and identify remark codes.
Step 2: Identify the Root Cause
Determine whether the issue is related to frequency limits, documentation, or coding.
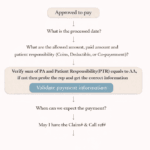
Step 3: Take Action Based on Scenario
Scenario A: CPT Maximum Reached
Verify patient history and service limits.
If justified, submit medical documentation and appeal.
Scenario B: Medical Necessity or Coding Issue
Compare CPT code with documentation and diagnosis.
Correct coding errors, adjust service level if needed, and add missing documentation.
Scenario C: Medical Records Requested
Gather physician notes, test results, and treatment plans.
Submit within the payer’s deadline.
Step 4: File an Appeal if Needed
Include a cover letter, corrected claim if applicable, and supporting documentation.
Example Scenario
A physician bills a high-level consultation, but documentation supports only moderate complexity.
Solution:
Review notes and either submit additional documentation or correct the CPT level and resubmit.
Key Tips to Prevent Denial Code 150
Ensure accurate and complete documentation
Match CPT codes with clinical notes
Verify medical necessity before billing
Track frequency limits for services
Respond quickly to documentation requests
Perform regular internal audits
Frequently Asked Questions (FAQs)
1. What does Denial Code 150 mean in simple terms?
It means the documentation does not support the level of service billed.
2. Can this denial be appealed?
Yes, with proper supporting documentation.
3. How do I find the exact reason for denial?
Check remark codes in the EOB or ERA.
4. Is this always a coding error?
No, it can also be due to frequency limits or missing documentation.
5. How can I avoid this denial?
Focus on accurate coding, complete documentation, and regular audits.
Conclusion
Denial Code 150 is primarily a documentation-related denial that highlights a mismatch between what was billed and what was supported. By understanding the causes such as frequency limits, medical necessity issues, and documentation gaps, you can resolve these denials efficiently.
A proactive approach with proper documentation, accurate coding, and regular audits will help reduce these denials and improve overall revenue cycle performance.