In medical billing, claim denials are a common challenge, and one frequent issue is when a procedure (CPT) code is inconsistent with the patient’s age. This denial occurs when the insurance payer determines that the billed procedure does not align with the age criteria defined for that specific code. For billing professionals and beginners in revenue cycle management (RCM), understanding how to identify, investigate, and resolve this denial is crucial. This guide explains the entire process in simple terms, along with practical steps, tips, and examples to help you handle such cases efficiently.
What Does “Procedure Code Inconsistent with Patient’s Age” Mean?
Certain CPT (Current Procedural Terminology) codes are designed for specific age groups. For example: Pediatric services for children, Geriatric services for elderly patients, Age-specific preventive exams. If a claim includes a CPT code that does not match the patient’s age, the insurance company rejects or denies the claim.
Example:
A pediatric wellness exam billed for a 45-year-old patient → Denial
A geriatric assessment billed for a child → Denial
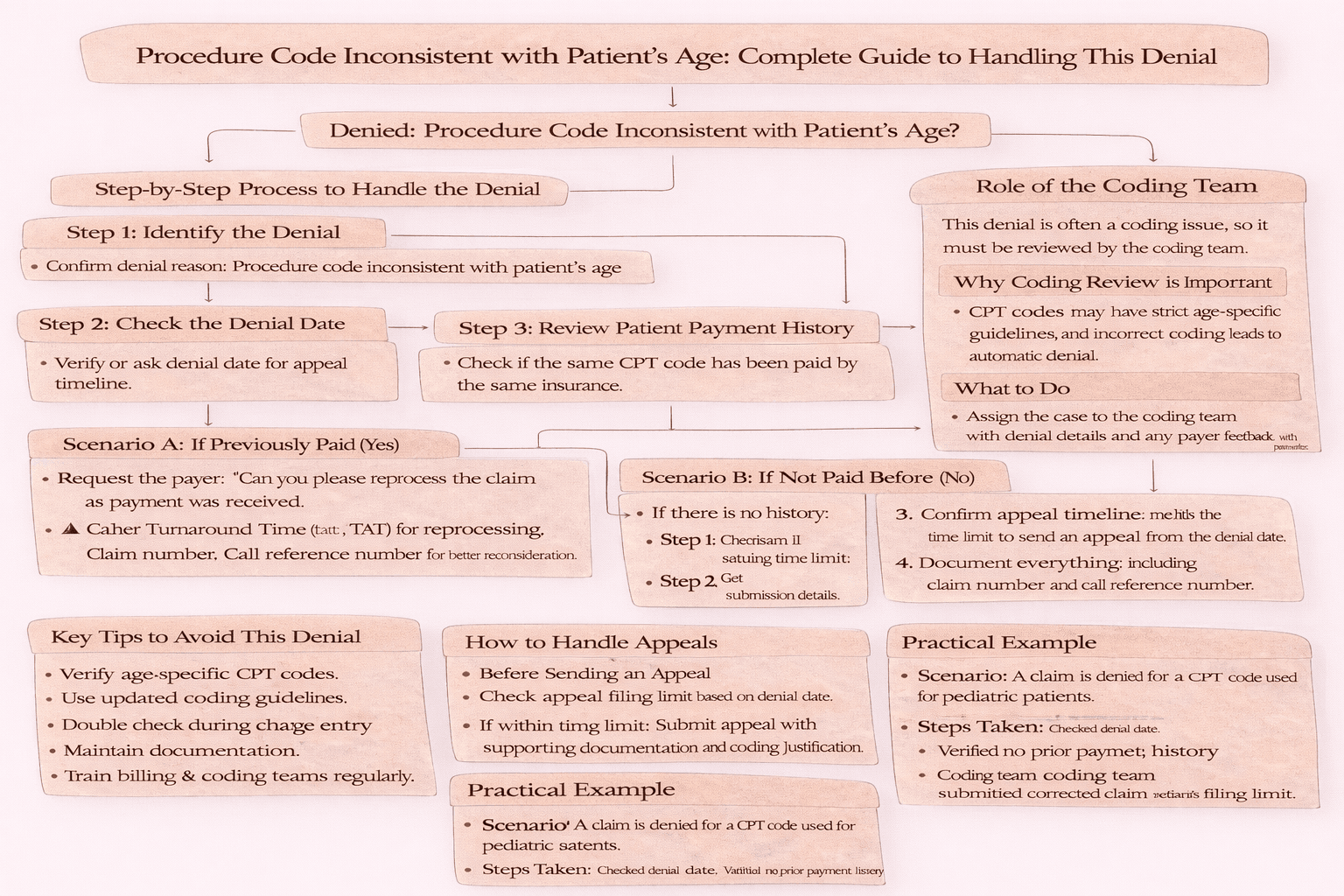
Step-by-Step Process to Handle the Denial
1. Identify the Denial
Start by confirming the denial reason: “Procedure code inconsistent with patient’s age.”
2. Check the Denial Date
Always ask or verify: Denial date which is important for appeal timelines.
3. Review Patient Payment History
Check whether the same CPT code was previously paid by the same insurance.
Scenario A: If Previously Paid (Yes)
If the same CPT was paid earlier: Request the payer: “Can you please reprocess the claim as payment was received for the same CPT earlier?” Ask: Turnaround Time (TAT) for reprocessing, Claim number, Call reference number. This strengthens your case for reconsideration.

Scenario B: If Not Paid Before (No)
If there is no history of payment:
Step 1: Check filing limits by asking the time limit to submit a corrected claim.
Step 2: Get submission details such as fax number or mailing address for appeal or corrections.
Step 3: Confirm appeal timeline which is the time limit to send an appeal from the denial date.
Step 4: Document everything including claim number and call reference number.
Role of the Coding Team
This denial is often a coding issue, so it must be reviewed by the coding team.
Why Coding Review is Important
CPT codes may have strict age-specific guidelines and incorrect coding leads to automatic denial.
What to Do
Assign the case to the coding team with denial details and any payer feedback such as valid age range for CPT.
After Coding Review: What Next?
Case 1: Coding Error Found
If the coding team identifies an incorrect CPT: Update the correct CPT code and submit a corrected claim. Ensure filing limit is not exceeded.
If the time limit is crossed: Check client instructions since some still want submission.
Case 2: Coding is Correct
If the coding team confirms the CPT is accurate: Proceed with an appeal.
How to Handle Appeals
Before Sending an Appeal
Check appeal filing limit based on denial date.
If within time limit: Submit appeal with supporting documentation and coding justification.
If time limit is crossed: Follow client instructions since some clients still require appeals, otherwise write off the claim.
Key Tips to Avoid This Denial
Verify age-specific CPT codes and always confirm whether the CPT matches patient age criteria.
Use updated coding guidelines by referring to latest CPT manuals and payer policies.
Double-check during charge entry by implementing validation checks before claim submission.
Maintain documentation by keeping records of payer communication and saving coding justifications.
Train billing and coding teams regularly to reduce recurring errors.
Practical Example
Scenario: A claim is denied for a CPT code used for pediatric patients.
Steps Taken: Checked denial date, Verified no prior payment history, Sent case to coding team, Coding team corrected CPT, Submitted corrected claim within filing limit.
Result: Claim successfully reimbursed.
Frequently Asked Questions (FAQs)
1. Why do insurance companies deny claims based on age?
Because certain CPT codes are defined for specific age groups and mismatches indicate incorrect billing.
2. Can I appeal if the CPT code is correct?
Yes, if the coding is accurate, you can submit an appeal with proper documentation and justification.
3. What if the corrected claim deadline has passed?
Follow client instructions: some allow submission anyway, otherwise the claim may need to be written off.
4. How do I know the valid age range for a CPT code?
You can check CPT coding manuals, insurance payer guidelines, or consult the coding team.
5. Who is responsible for fixing this denial?
Primarily the coding team, but billing teams must coordinate and take action based on their response.
Conclusion
The “procedure code inconsistent with patient’s age” denial is a common but manageable issue in medical billing. The key lies in accurate coding, timely follow-up, and clear communication with payers and coding teams. By following a structured approach verifying payment history, involving the coding team, and respecting filing limits, you can resolve these denials efficiently and reduce revenue loss. Staying proactive with coding accuracy and documentation will not only minimize errors but also improve overall claim success rates.