In medical billing, claim denials are a common challenge that can delay reimbursements and impact revenue cycles. One such denial is Code 146: “Diagnosis was invalid for the date(s) of service reported.”
This denial occurs when the diagnosis (DX) code submitted on a claim is not valid or acceptable for the specific date of service (DOS). Understanding how to identify, investigate, and resolve this issue is crucial for billing professionals, coders, and healthcare providers.
In this guide, we’ll break down everything you need to know about denial code 146 in a simple, practical way—along with actionable steps to resolve it efficiently.
What Does Denial Code 146 Mean?
Denial Code 146 indicates that the diagnosis code used in the claim is not valid for the date of service submitted.
Common Reasons:
The DX code was inactive or deleted before the service date
The code became effective after the service date
Incorrect or outdated ICD version was used
Typographical or coding errors
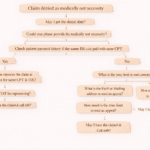
Step-by-Step Process to Handle Denial Code 146
Handling this denial requires a structured approach. Here’s a simplified workflow based on real-world billing practices:

- Verify the Denial Details
Start by gathering essential information:
Denial date
Claim number
Invalid diagnosis code(s)
Ask:
Which diagnosis code is invalid?
Are multiple diagnosis codes affected?
- Check Patient Payment History
Review whether the same diagnosis code has been previously accepted.
Scenario A: Same DX + CPT Paid Before
If the same combination of diagnosis (DX) and procedure (CPT) was previously paid:
Request the payer to reprocess the claim
Provide proof of prior payment if needed
Ask:
Can you reprocess the claim?
What is the turnaround time (TAT)?
Can I get the claim reference number?
Scenario B: No Prior Payment Found
If there is no history of payment:
Determine the time limit to submit a corrected claim
Collect submission details
Ask:
What is the corrected claim filing deadline?
What is the fax number or mailing address?
- Send Claim to Coding Team
This is a critical step.
Assign the denial to the coding team for validation:
Confirm whether the diagnosis code is correct
Identify a valid replacement if needed
What to Do Based on Coding Team Response
If Coding Team Provides a New DX Code:
Update the claim with the correct diagnosis
Submit a corrected claim
Ensure submission is within the time limit
Note: Some clients may request submission even after the deadline—follow client-specific guidelines.
If Coding Team Confirms DX Code Is Correct:
Prepare and send an appeal to the insurance payer
Before appealing:
Check appeal filing limits (from denial date)
Ensure documentation supports medical necessity
Appeal Process Explained
When sending an appeal:
Include:
Original claim details
Explanation of why the diagnosis is valid
Supporting medical records
Coding references (if applicable)
Important Questions:
What is the appeal time limit?
Is the appeal still within the allowed period?
If Appeal Deadline Is Crossed:
Typically, the claim may need to be written off
However, follow client instructions—some may still request submission
Key Tips to Avoid Denial Code 146
Preventing this denial is always better than fixing it later.
Best Practices:
Always verify ICD code validity dates
Use updated coding software or encoder tools
Cross-check diagnosis codes with date of service
Ensure correct ICD version (ICD-9 vs ICD-10 if applicable historically)
Train staff regularly on coding updates
Perform pre-submission claim audits
Example Scenario
Let’s simplify with an example:
Situation:
A claim submitted for December 1, 2019 includes a diagnosis code that became effective in 2020.
Outcome:
The payer rejects it with denial code 146 because the code wasn’t valid on that date.
Resolution:
Coding team reviews and replaces with a valid 2019 code
Corrected claim is submitted within filing limits
Frequently Asked Questions (FAQs)
- What is the main cause of denial code 146?
The most common cause is using a diagnosis code that is not valid for the specific date of service—either expired or not yet active. - Can I resubmit the same claim without changes?
Only if you have proof that the same DX and CPT combination was previously paid. Otherwise, correction or appeal is required. - How do I know if a diagnosis code is valid?
Use updated ICD coding tools or check official coding guidelines that list effective and termination dates. - What happens if the corrected claim deadline has passed?
Typically, the claim is written off. However, some clients may still request submission or appeal—always follow client instructions. - When should I send an appeal instead of a corrected claim?
Send an appeal when the coding team confirms the diagnosis code is correct and does not require changes.
Conclusion:
Denial Code 146 can seem complex at first, but with a structured approach, it becomes manageable. The key is to verify diagnosis validity, involve the coding team, and act within timelines.
Whether it’s reprocessing, correcting, or appealing a claim, understanding the root cause and following the correct workflow ensures faster resolution and improved revenue cycle performance.
By implementing preventive measures and maintaining strong coordination between billing and coding teams, you can significantly reduce the occurrence of this denial in the future.