Medical billing can feel complex, especially when claims get denied. One of the common denial reasons healthcare providers encounter is Denial Code 151, which relates to service frequency or maximum allowable limits. In this article, you’ll learn what Denial Code 151 means, why it happens, and how to handle it effectively in simple, practical terms.
What is Denial Code 151?
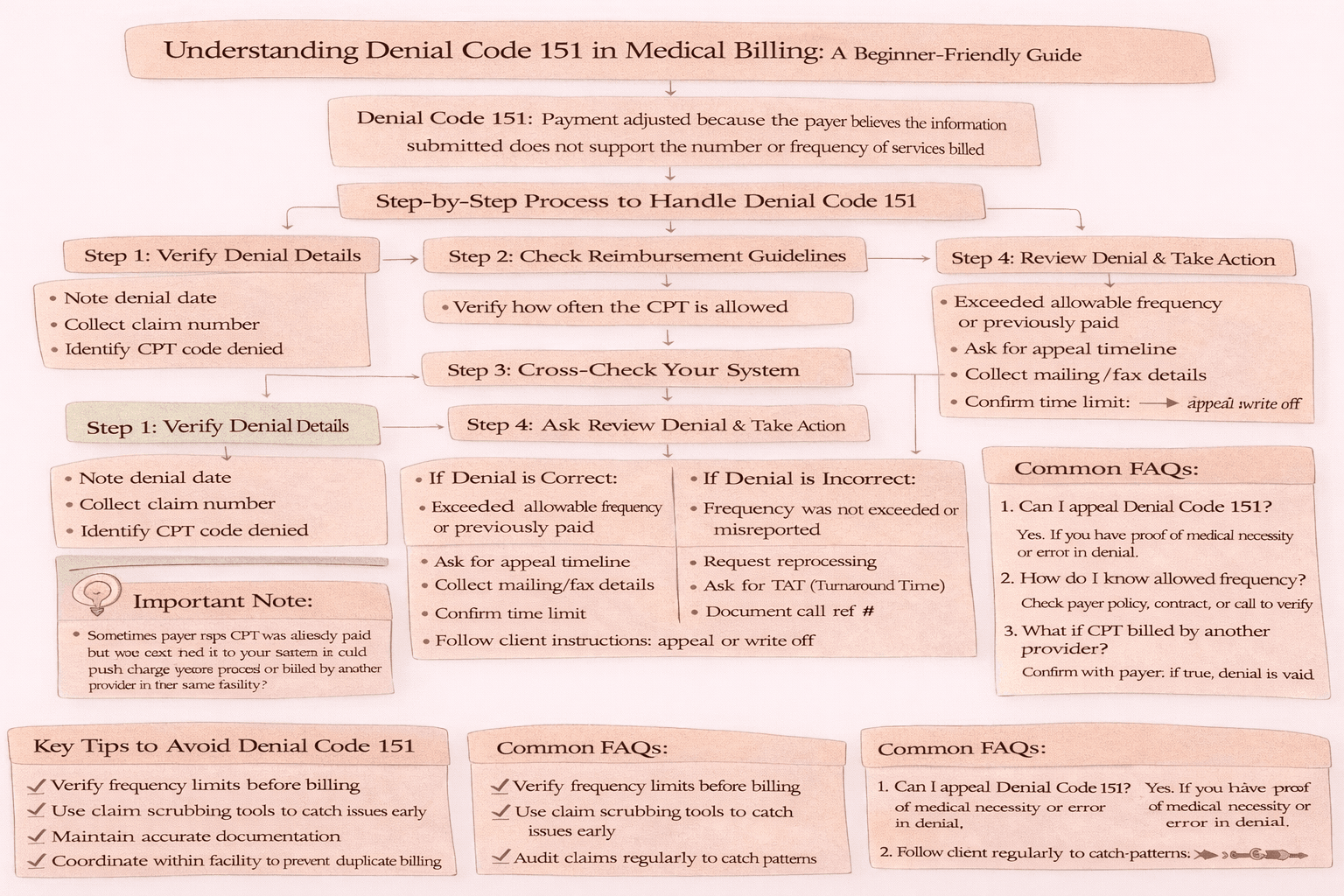
Denial Code 151 means payment adjusted because the payer believes the information submitted does not support the number or frequency of services billed. In simple terms, the insurance company thinks the service was performed too many times or exceeded the allowed frequency within a specific time frame.
Why Does Denial Code 151 Occur?
This denial usually happens when a CPT code exceeds the payer’s allowed usage limits.
Common reasons include:
The same procedure billed multiple times in one day
Service exceeds daily, weekly, or monthly limits
Incorrect billing frequency
Duplicate claims
Missing documentation to justify repeated services
Example:
If a CPT code is allowed once per day but billed twice on the same day, the second charge may be denied with Code 151.
Step-by-Step Process to Handle Denial Code 151
Handling this denial requires a structured approach.
1. Verify the Denial Details
Gather denial date, claim number, and CPT code involved.
2. Check the Payer’s Reimbursement Guidelines
Verify how often the CPT code is allowed such as once per day, per visit, or per month.
3. Cross-Check Your System
Compare payer rules with your records. Check if the same CPT was billed on the same day, billed under another provider in the same facility, or if there is a missing charge posting.
4. Determine if the Denial is Correct or Incorrect
If denied correctly:
The CPT exceeded allowed frequency or was already paid.
Action steps include asking for appeal timeline, collecting mailing or fax details, confirming time limits, and following client instructions such as appeal or write off.
If denied incorrectly:
The CPT was not billed previously or frequency limits were not exceeded.
Action steps include requesting reprocessing, asking for turnaround time, and documenting call reference details.
Important Scenario to Watch For
Sometimes you may not find the CPT in your system but the payer says it has already been paid. This could mean the charge was not posted or another provider in the same facility billed it. In such cases, ask for CPT details and billing provider name, document everything, and treat the denial as correct if confirmed.
Key Tips to Avoid Denial Code 151
Always verify frequency limits before billing.
Use claim scrubbing tools to catch issues early.
Maintain accurate documentation to support repeated services.
Coordinate within the facility to avoid duplicate billing.
Audit claims regularly to identify patterns.
Real-Life Example
CPT 99213 is allowed once per day. A patient visits twice on the same day and both visits are billed. The first claim is paid and the second is denied with Code 151. If medically necessary, you can appeal with proper documentation. If it is a duplicate, accept the denial or write it off.
FAQs About Denial Code 151
1. Can I appeal Denial Code 151?
Yes, if you have documentation proving medical necessity or if the denial is incorrect.
2. How do I know the allowed frequency of a CPT code?
Check payer policy manuals, call the insurance representative, or refer to contract guidelines.
3. What if the CPT was billed by another provider?
Verify with the payer and internally. If confirmed, the denial is usually valid.
4. What is the typical time limit for appeals?
It varies by payer but usually ranges from 30 to 180 days.
5. What should I document during calls?
Call reference number, representative name, date and time, and discussion details.
Conclusion
Denial Code 151 is mainly related to service frequency limits. While it may seem complicated at first, it becomes manageable when you follow a structured process verify payer guidelines, compare with your records, identify whether the denial is correct, and take appropriate action. By improving documentation, checking frequency rules in advance, and coordinating internally, you can reduce denials and improve overall revenue cycle efficiency.