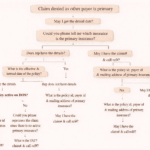
In medical billing, denial codes are a common challenge that healthcare providers and billing teams must handle efficiently. One such frequently encountered denial is Denial Code 97, which states:
“The benefit for this service is included in the payment/allowance for another service/procedure that has already been adjudicated.”
Simply put, this means that the insurance payer considers the billed service as part of another procedure already paid for. This situation is often referred to as a bundling issue.
Understanding why this denial occurs and how to resolve it is crucial for maximizing reimbursements and reducing revenue loss. This guide breaks down Denial Code 97 in a clear, beginner-friendly way.
What Does Denial Code 97 Mean?
Denial Code 97 indicates that:
A procedure or service submitted in a claim is not separately payable
It is already included (bundled) in another service billed on the same date
The insurance company has processed and paid the primary procedure, but not the additional one
Example
If a provider bills for:
A surgical procedure
And a minor service that is typically included in that surgery
The insurer may deny the minor service under Code 97 because it is considered part of the main procedure.
Why Does This Denial Occur?
- NCCI Edits (Bundling Rules)
The National Correct Coding Initiative (NCCI) defines which procedures can and cannot be billed together.
Some codes are always bundled
Others can be billed together only with appropriate modifiers - Missing or Incorrect Modifiers
Modifiers indicate that a service is distinct or separate.
Without the correct modifier, the payer assumes bundling applies
Example modifiers: -59, -25, -XS - Duplicate or Overlapping Services
If two procedures overlap in scope, the payer may deny one as inclusive. - Incorrect Coding
Sometimes the issue arises from:
Wrong CPT code selection
Improper documentation
Step-by-Step Process to Handle Denial Code 97
- Verify the Denial Details
Ask or check:
Denial date
Claim number
Reference number - Identify the Bundled CPT Code
Find out:
Which CPT code was paid
Which CPT code was denied
Whether both were billed on the same date of service (DOS) - Check Timely Filing Limits
Always confirm:
Deadline to submit corrected claims or appeals - Review NCCI Edits
Use coding tools to check:
Whether bundling is valid
If it can be overridden with a modifier - Consult the Coding Team
Send the case to coders to determine:
If modifier correction is needed
If the denial is valid
Tools to Identify Bundled CPT Codes
Encoder tools
Find-A-Code
NCCI edit tables
Payer-specific guidelines
These tools help determine:
Whether two CPT codes are bundled
If a modifier can override the edit
Which modifier is appropriate
How to Resolve Denial Code 97
Scenario 1: Modifier Can Be Applied
If the coding team confirms a modifier is appropriate:
Update the CPT code with the correct modifier
Submit a corrected claim
For Medicare: Submit a new (fresh) claim instead of corrected
Scenario 2: Coding Is Correct (No Bundling)
If no NCCI edit exists:
Contact the insurance payer
Request reprocessing of the claim
If denied again, proceed with an appeal
Scenario 3: Service Is Truly Bundled
If the service is legitimately included:
The charge must be written off
No further action required
Important Tips to Prevent Code 97 Denials
Always verify NCCI edits before claim submission
Use modifiers only when clinically justified
Ensure proper documentation supports separate services
Avoid billing duplicate or overlapping procedures
Train staff regularly on coding updates
Key Takeaways
Denial Code 97 indicates a bundled or inclusive service
It often results from NCCI edits or missing modifiers
Not all denials are errors—some are valid and non-payable
Proper use of tools and coding knowledge is essential
Always involve the coding team for accuracy
Frequently Asked Questions (FAQs)
- What is bundling in medical billing?
Bundling means combining multiple services into one payment. The insurer pays for the primary procedure and considers related services included. - Can Denial Code 97 be appealed?
Yes, but only if:
The coding is correct
No NCCI edit exists
Documentation supports separate billing - Which modifiers help override bundling?
Common modifiers include:
-59 (Distinct procedural service)
-25 (Significant, separate E/M service)
-XS (Separate structure) - Does Medicare accept corrected claims for Code 97?
No. Medicare typically requires a new claim submission instead of a corrected one. - When should a claim be written off?
If the service is truly bundled and cannot be unbundled with a modifier, it should be written off.
Conclusion:
Denial Code 97 is one of the most common yet manageable issues in medical billing. It revolves around the concept of bundled services, which can initially seem confusing but becomes clearer with proper tools and processes.
By understanding NCCI edits, using the right modifiers, and collaborating with coding teams, billing professionals can significantly reduce denials and improve reimbursement rates. Consistency, accuracy, and proactive verification are the keys to staying ahead of Code 97 challenges.