In medical billing and revenue cycle management, claim denials are a common challenge. One specific denial that often confuses beginners is: “Procedure/Revenue Code is inconsistent with the patient’s age.” This denial occurs when a submitted CPT (Current Procedural Terminology) code does not align with the patient’s age criteria defined by the payer or coding guidelines. Understanding how to identify, investigate, and resolve this denial is essential for minimizing revenue loss and ensuring compliance. This guide breaks down the process step-by-step in simple terms, making it easy for beginners to follow.
What Does “Procedure Code Inconsistent with Patient’s Age” Mean?
Certain medical procedures are age-specific. Insurance companies enforce rules that define which procedures are valid for children, which apply to adults, and which are limited to specific age ranges.
Example:
A pediatric procedure billed for a 45-year-old patient
A geriatric screening billed for a teenager
In such cases, the insurance system flags the mismatch and denies the claim.
Common Reasons for This Denial
Understanding the root cause helps resolve the issue faster.
1. Incorrect CPT Code Selection
The most common reason is assigning a CPT code that doesn’t match the patient’s age group.
2. Coding Errors
Mistakes during coding, especially when similar procedures exist for different age groups, can lead to denial.
3. Lack of Documentation
If documentation doesn’t justify the procedure for that age, the payer may reject it.
4. Payer-Specific Guidelines
Different insurance companies may have unique age restrictions for certain procedures.
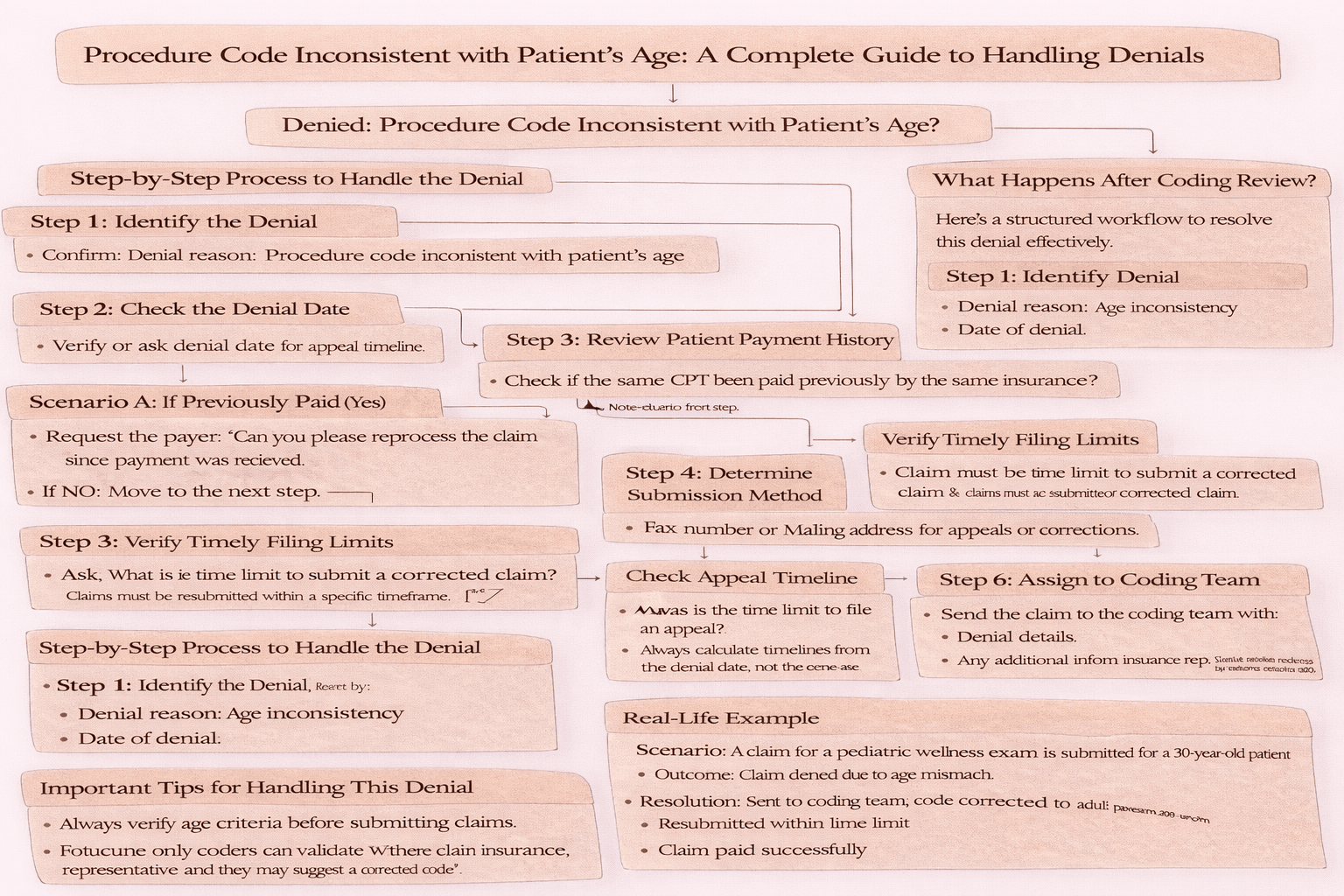
Step-by-Step Process to Handle the Denial
Here’s a structured workflow to resolve this denial effectively.
Step 1: Identify the Denial
Start by confirming: Denial reason: Age inconsistency, Date of denial.
Step 2: Check Patient Payment History
Ask: Has the same CPT been paid previously by the same insurance?
If YES: Request the insurance representative: “Can you please reprocess the claim since payment was previously received for the same CPT?” Ask for: Turnaround Time (TAT), Claim number, Call reference number.
If NO: Move to the next step.
Step 3: Verify Timely Filing Limits
Ask: What is the time limit to submit a corrected claim? This is crucial because claims must be resubmitted within a specific timeframe.
Step 4: Determine Submission Method
Find out: Fax number or Mailing address for appeals or corrections.
Step 5: Check Appeal Timeline
Ask: What is the time limit to file an appeal? Always calculate timelines from the denial date, not the service date.
Step 6: Assign to Coding Team
Send the claim to the coding team with: Denial details, Any additional information from the insurance representative. Because only coders can validate whether the CPT code is correct and they may suggest a corrected code.
What Happens After Coding Review?
Scenario 1: CPT Code is Incorrect
Update the claim with the correct CPT code and submit a corrected claim if within time limit.
If time limit is exceeded: Follow client instructions, some clients still want submission.
Scenario 2: CPT Code is Correct
Prepare and submit an appeal. Include: Medical records, Justification for procedure, Supporting documentation.
If appeal time limit is exceeded: Write off the claim unless client advises otherwise.
Important Tips for Handling This Denial
Always verify age criteria before submitting claims and ensure the CPT code aligns with the patient’s age and procedure guidelines.
Document everything including calls with insurance, claim numbers, and reference IDs.
Communicate clearly with the coding team and provide complete denial details and payer feedback.
Track timely filing deadlines carefully because missing deadlines can lead to permanent revenue loss.
Follow client instructions since some clients want appeals even after deadlines.
Real-Life Example
Scenario: A claim for a pediatric wellness exam is submitted for a 30-year-old patient.
Outcome: Claim denied due to age mismatch.
Resolution: Sent to coding team, Code corrected to adult preventive exam, Resubmitted within time limit, Claim paid successfully.
FAQs
1. What is a CPT code?
A CPT code is a standardized code used to describe medical procedures and services for billing purposes.
2. Why do age-related denials happen?
They occur when the billed procedure is not appropriate for the patient’s age based on payer or coding guidelines.
3. Can I resubmit a denied claim?
Yes, you can submit a corrected claim if it is within the payer’s timely filing limit.
4. What if the coding is correct but still denied?
In that case, you should file an appeal with proper documentation to justify the procedure.
5. What happens if the time limit is crossed?
Typically, the claim is written off unless the client instructs otherwise or the payer allows exceptions.
Conclusion
The “Procedure Code Inconsistent with Patient’s Age” denial may seem complex at first, but with a structured approach, it becomes manageable. The key lies in identifying the issue quickly, collaborating with the coding team, understanding payer rules, and acting within timelines. By following the steps outlined in this guide, you can reduce denials, improve claim acceptance rates, and ensure smoother revenue cycle operations. Mastering these workflows not only improves efficiency but also builds confidence in handling real-world medical billing scenarios.