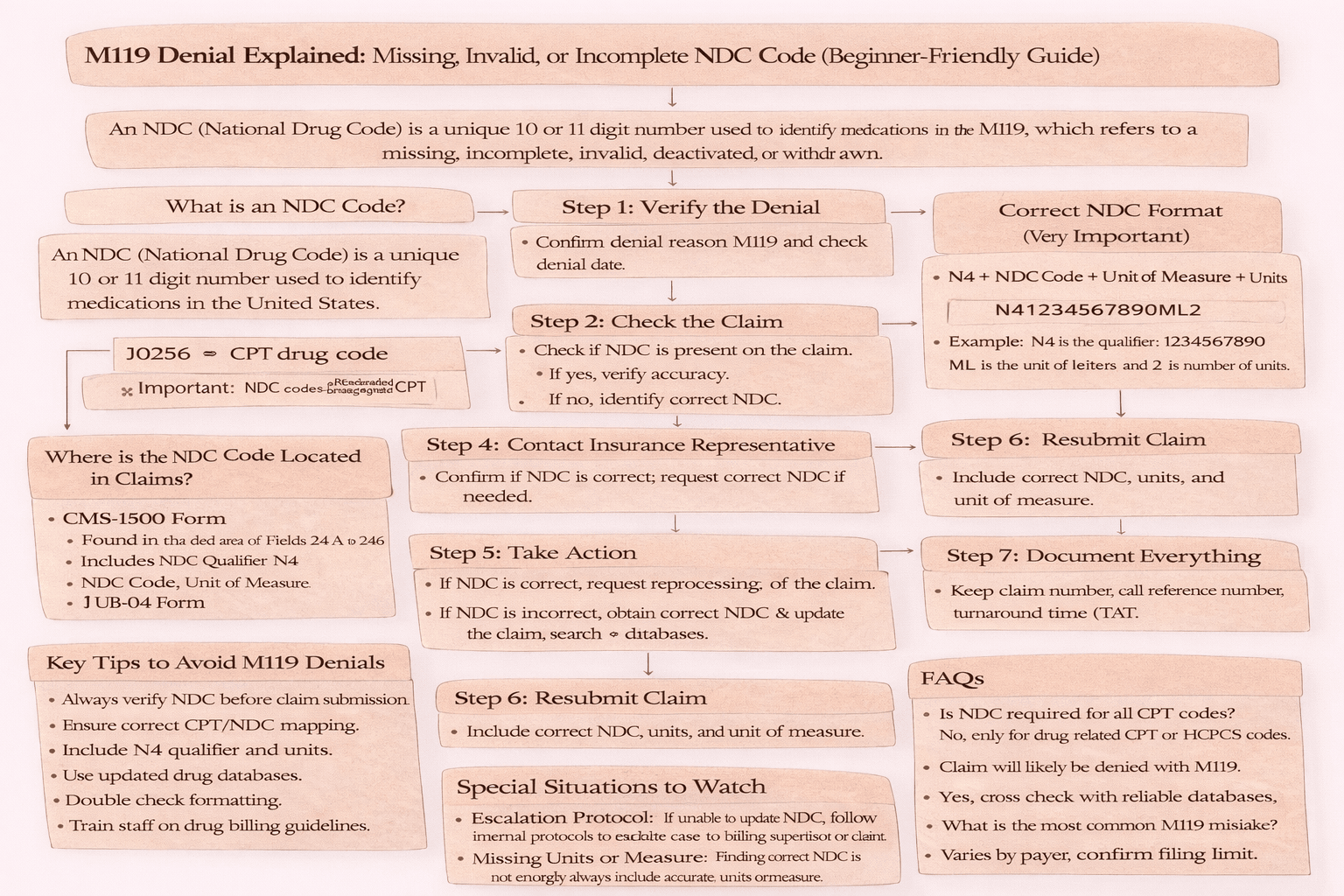
In medical billing, claim denials are a common challenge and one of the frequent ones is M119, which refers to a missing, incomplete, invalid, deactivated, or withdrawn National Drug Code (NDC). If you’re new to healthcare revenue cycle management (RCM), this denial can feel confusing, especially because it involves both coding accuracy and claim formatting. This guide breaks down everything you need to know about M119 denials in simple terms what they mean, why they happen, and how to fix them efficiently.
What is an NDC Code?
An NDC (National Drug Code) is a unique 10 or 11 digit number used to identify medications in the United States. It provides detailed information about the drug manufacturer, the specific drug product, and the package size.
Example:
J0256 → CPT drug code
Corresponding NDC code identifies the exact drug used
Important: NDC codes are required only for drug-related CPT or HCPCS codes which typically start with a letter such as J codes like J7649 or J2425.
What Does M119 Denial Mean?
The M119 denial code indicates that the claim was rejected due to an issue with the NDC code. This could be because the NDC is missing, incorrect or invalid, incomplete, or inactive or withdrawn. In simple terms, the payer cannot process the drug claim because the drug identification details are incorrect or absent.
Where is the NDC Code Located in Claims?
Understanding where to find or enter the NDC code is critical.
CMS-1500 Form: Found in the shaded area of fields 24A to 24G and must include NDC Qualifier such as N4, NDC Code, Unit of Measure, and Number of Units.
UB-04 Form: Located in Field 43.
Correct NDC Format (Very Important)
When billing, the NDC must follow a structured format.
N4 + NDC Code + Unit of Measure + Units
Example:
N41234567890ML2
Where N4 is the qualifier, 1234567890 is the NDC, ML is the unit of measure in milliliters, and 2 is the number of units.
Common Causes of M119 Denials
1. Missing NDC Code
Drug CPT billed without NDC information.
2. Incorrect NDC Code
Wrong drug linked to CPT code.
3. Invalid or Deactivated NDC
Drug is discontinued or no longer recognized.
4. Incomplete NDC Details
Missing units or unit of measure.
5. Formatting Errors
Missing qualifier N4 or incorrect digit count.
Step-by-Step Process to Handle M119 Denial
Here’s a practical workflow you can follow.
Step 1: Verify the Denial
Confirm denial reason M119 and check denial date.
Step 2: Check the Claim
Check if NDC is present on the claim. If yes, verify accuracy. If no, identify the correct NDC.
Step 3: Validate NDC Code
Ask if the NDC is correct for the drug billed and whether it is active and valid.
Step 4: Contact Insurance Representative
Confirm if NDC is correct and request correct NDC if needed.
Step 5: Take Action
If NDC is correct, request reprocessing of the claim. If NDC is incorrect, obtain the correct NDC and update the claim. If the representative refuses to provide it, search reliable sources such as drug databases and cross check.
Step 6: Resubmit Claim
Include correct NDC, units, and unit of measure.
Step 7: Document Everything
Keep claim number, call reference number, and turnaround time (TAT).
Key Tips to Avoid M119 Denials
Always verify NDC before claim submission.
Ensure correct mapping between CPT and NDC.
Include all required components such as qualifier and units.
Use updated drug databases.
Double check formatting.
Train staff on drug billing guidelines.
Special Situations to Watch
When you cannot update the NDC, assign the case to the client or billing team and follow internal escalation protocols.
For missing units or measure, even if you find the correct NDC you still need the unit of measure such as ML, UN, or GR and the quantity. Without these, the claim will still be rejected.
FAQs
1. Is NDC required for all CPT codes?
No, NDC is required only for drug related CPT or HCPCS codes, typically J codes.
2. What happens if I submit a claim without NDC?
The claim will likely be denied with M119.
3. Can I find NDC codes online?
Yes, but always verify accuracy using reliable drug databases or confirm with the payer.
4. What is the most common mistake causing M119?
Incorrect format or missing units is one of the most frequent issues.
5. How long do I have to resubmit a corrected claim?
It depends on the payer, always ask for the timely filing limit or correction window.
Conclusion
The M119 denial may seem technical, but it comes down to one key issue incorrect or missing drug identification details. By understanding how NDC codes work, where to locate them, and how to format them properly, you can resolve and even prevent these denials efficiently. The key is attention to detail ensure every drug claim includes a complete and accurate NDC entry. When in doubt, verify, document, and follow up. Mastering this process will not only reduce denials but also improve overall billing accuracy and revenue flow.