In medical billing, claim denials are a common challenge, and one of the more confusing ones is when a claim is rejected due to a procedure code being inconsistent with the patient’s gender. This type of denial often leaves billing professionals wondering whether the issue lies in coding, patient demographics, or payer systems. Understanding how to identify, investigate, and resolve this denial is essential for maintaining revenue flow and reducing rework. In this guide, we’ll break down the process step by step in simple terms, making it easy for beginners and experienced billers alike.
What Does “Procedure Code Inconsistent with Patient’s Gender” Mean?
This denial occurs when a CPT code submitted on a claim does not align with the patient’s recorded gender in the insurance system. Example: CPT 77067 (Screening Mammography) is typically billed for female patients. If billed for a male patient, the claim will likely be denied. This mismatch triggers automated payer edits, resulting in claim rejection or denial.
Common Causes of This Denial
- Incorrect Patient Demographics – Gender entered incorrectly or data entry errors.
- Coding Errors – Wrong CPT code or incorrect gender-specific procedure assignment.
- Insurance System Mismatch – Gender updated in provider system but not in payer system.
- Special Medical Cases – Valid across genders but need documentation/modifiers.
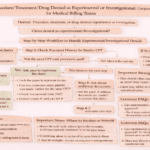
Step-by-Step Process to Handle the Denial
Step 1: Verify Denial Details – Collect denial date, claim number, and reason code.
Step 2: Check Patient Payment History – If previously paid, request reprocessing with proof; collect TAT and references. If not, proceed.
Step 3: Review Timely Filing Limits – Check corrected claim and appeal deadlines; collect submission details.
Step 4: Verify Patient Gender – Check PMS, EHR, and insurance portal. If incorrect: update and resubmit. If correct: move to coding.
Step 5: Send to Coding Team – Validate CPT code. If incorrect: update and resubmit. If correct: prepare appeal.
Step 6: Submit Corrected Claim or Appeal – Within limit → submit; If exceeded → follow client instruction or write off.
Important Tips for Handling This Denial
Verify eligibility first; Check demographics carefully; Know gender-specific CPT codes; Track deadlines; Maintain documentation; Communicate with payer and note references.
Real-World Example
CPT 77067 denied for male patient → Check gender (correct) → Coding error found → Update CPT → Resubmit → Claim processed.
Key Takeaways
Denial mainly due to demographic or coding mismatch; Always verify gender first; Follow structured steps; Track timelines; Use coding team support.
Frequently Asked Questions (FAQs)
- What are gender-specific CPT codes? Procedures usually linked to one gender.
- Can claim be approved for both genders? Yes, with proper documentation/modifiers.
- If gender wrong in insurance? Update and resubmit.
- When to involve coding team? When demographics are correct but denial continues.
- Filing deadline missed? Usually write-off unless exceptions apply.
Conclusion
Gender mismatch denials are manageable with proper verification, coding accuracy, and timely action. Attention to detail and a structured workflow help reduce errors and improve claim success rates.