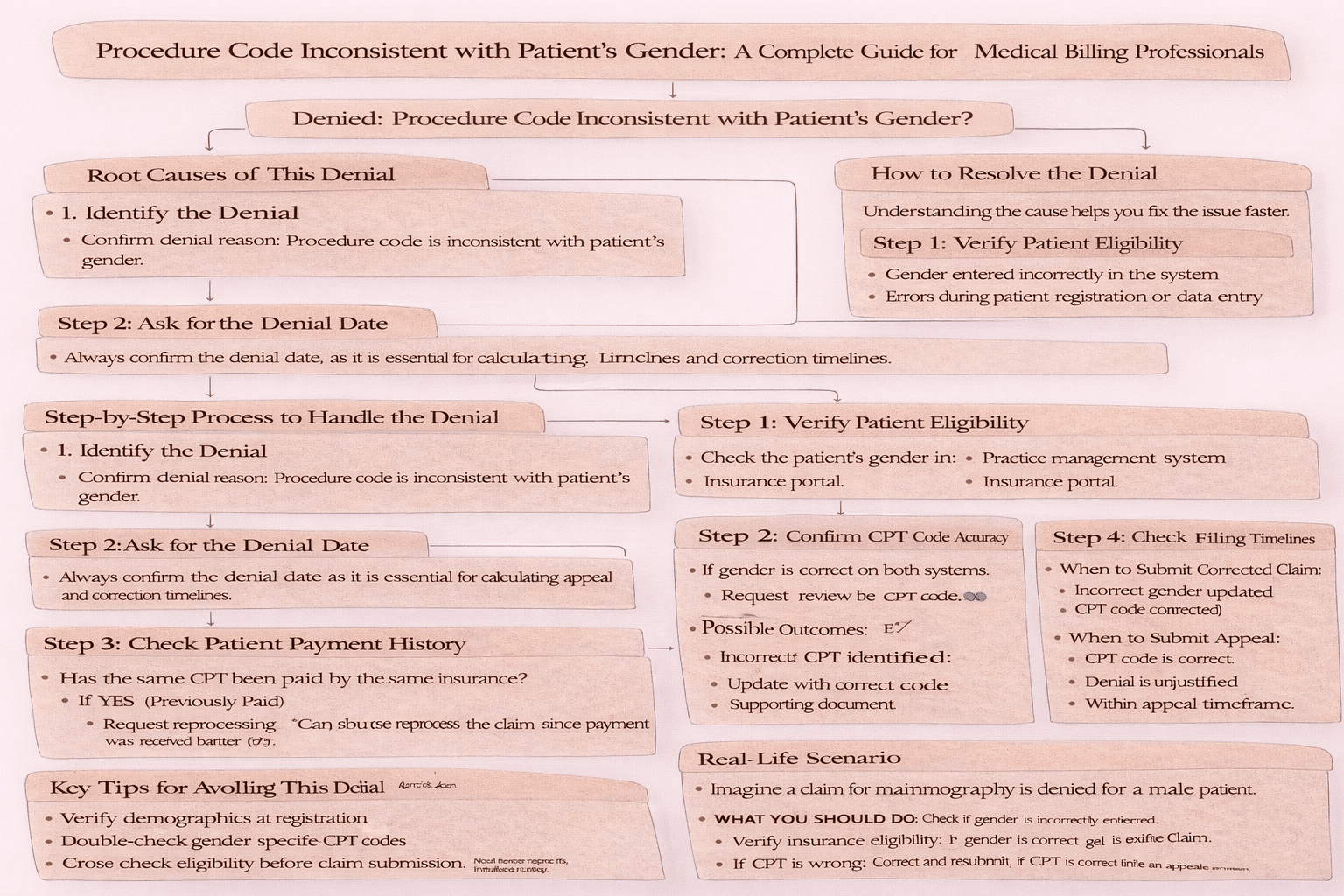
In medical billing, claim denials are a common challenge but some are easier to fix than others. One such denial is “Procedure/Revenue Code is inconsistent with the patient’s gender.” This denial typically occurs when a procedure code (CPT code) submitted on a claim does not align with the patient’s recorded gender. While it may seem like a simple issue, resolving it requires careful verification, correct workflow, and proper communication with insurance payers. This guide explains everything you need to know from identifying the root cause to resolving the denial effectively.
What Does This Denial Mean?
This denial indicates that the procedure billed is gender-specific, but the patient’s gender on file does not match the expected gender for that procedure.
Example:
CPT 77067 (Breast Mammography) is generally applicable to female patients. If billed for a male patient, the claim will likely be denied.
Step-by-Step Process to Handle the Denial
1. Identify the Denial
When you receive the denial, verify the reason: Procedure code is inconsistent with the patient’s gender.
2. Ask for the Denial Date
Always confirm the denial date, as it is crucial for calculating timelines for appeals or corrected claims.
3. Check Patient Payment History
Determine whether the same CPT code has been previously paid by the same insurance.
If YES (Previously Paid): Request reprocessing. “Can you please reprocess the claim as payment was received earlier for the same CPT?” Ask: Turnaround Time (TAT) for reprocessing, Claim number, Call reference number.
If NO (Not Paid Before): Ask the payer: Time limit to submit a corrected claim, Fax number or mailing address for appeal, Time limit for appeal submission. Document: Claim number, Call reference number.
Root Causes of This Denial
Understanding the cause helps you fix the issue faster.
1. Incorrect Patient Demographics
Gender entered incorrectly in the system, Errors during patient registration or data entry.
2. Eligibility Data Mismatch
Insurance records may have outdated or incorrect gender information.
3. Incorrect CPT Code
The procedure may have been coded incorrectly. Some procedures are strictly gender-specific.
How to Resolve the Denial
Step 1: Verify Patient Eligibility
Check the patient’s gender in: Practice management system, Insurance portal. If incorrect: Update the correct gender and resubmit the claim.
Step 2: Confirm CPT Code Accuracy
If gender is correct on both systems: Assign the case to the coding team and request review of the CPT code.
Possible Outcomes:
Incorrect CPT identified: Update with correct code and submit a corrected claim.
CPT confirmed correct: Proceed with an appeal.
Step 3: Check Filing Timelines
Always verify time limits.
For Corrected Claims: Must be submitted within payer’s correction window.
For Appeals: Calculate from denial date and ensure submission within allowed timeframe.
Important: Some clients may request submission even after deadlines, follow client instructions.
Step 4: Submit Corrected Claim or Appeal
When to Submit Corrected Claim: Incorrect gender updated, CPT code corrected, Time limit not crossed.
When to Submit Appeal: CPT code is correct, Denial is unjustified, Within appeal timeframe.
Key Tips for Avoiding This Denial
Verify demographics at registration, Double-check gender-specific CPT codes, Cross-check eligibility before claim submission, Maintain proper documentation for appeals, Track payer-specific timelines carefully.
Real-Life Scenario
Imagine a claim for mammography is denied for a male patient.
What You Should Do: Check if gender is incorrectly entered, Verify insurance eligibility.
If gender is correct: Send to coding team.
If CPT is wrong: Correct and resubmit.
If CPT is correct: File an appeal.
Frequently Asked Questions (FAQs)
1. What are gender-specific CPT codes?
These are procedure codes applicable only to a specific gender, such as mammograms for females or prostate exams for males.
2. What should I do if patient gender is entered incorrectly?
Update the correct gender in the system and resubmit the claim as a corrected claim.
3. When should I send the claim to the coding team?
If the patient’s gender is correct but the denial persists, the CPT code must be reviewed by coding experts.
4. Can I appeal if the time limit has passed?
Generally, no. However, some clients may request appeals even after the deadline, follow client guidelines.
5. What is the most common cause of this denial?
Incorrect patient gender entry or misuse of gender-specific CPT codes.
Conclusion
The denial “Procedure code inconsistent with patient’s gender” is usually straightforward but requires a structured approach. By verifying patient demographics, checking eligibility, and reviewing CPT coding accuracy, most of these denials can be resolved efficiently. The key lies in attention to detail, proper documentation, and adherence to payer timelines. When handled correctly, you can reduce revenue loss and improve claim acceptance rates significantly. By implementing best practices and maintaining strong coordination between billing and coding teams, you can prevent such denials from recurring in the future.