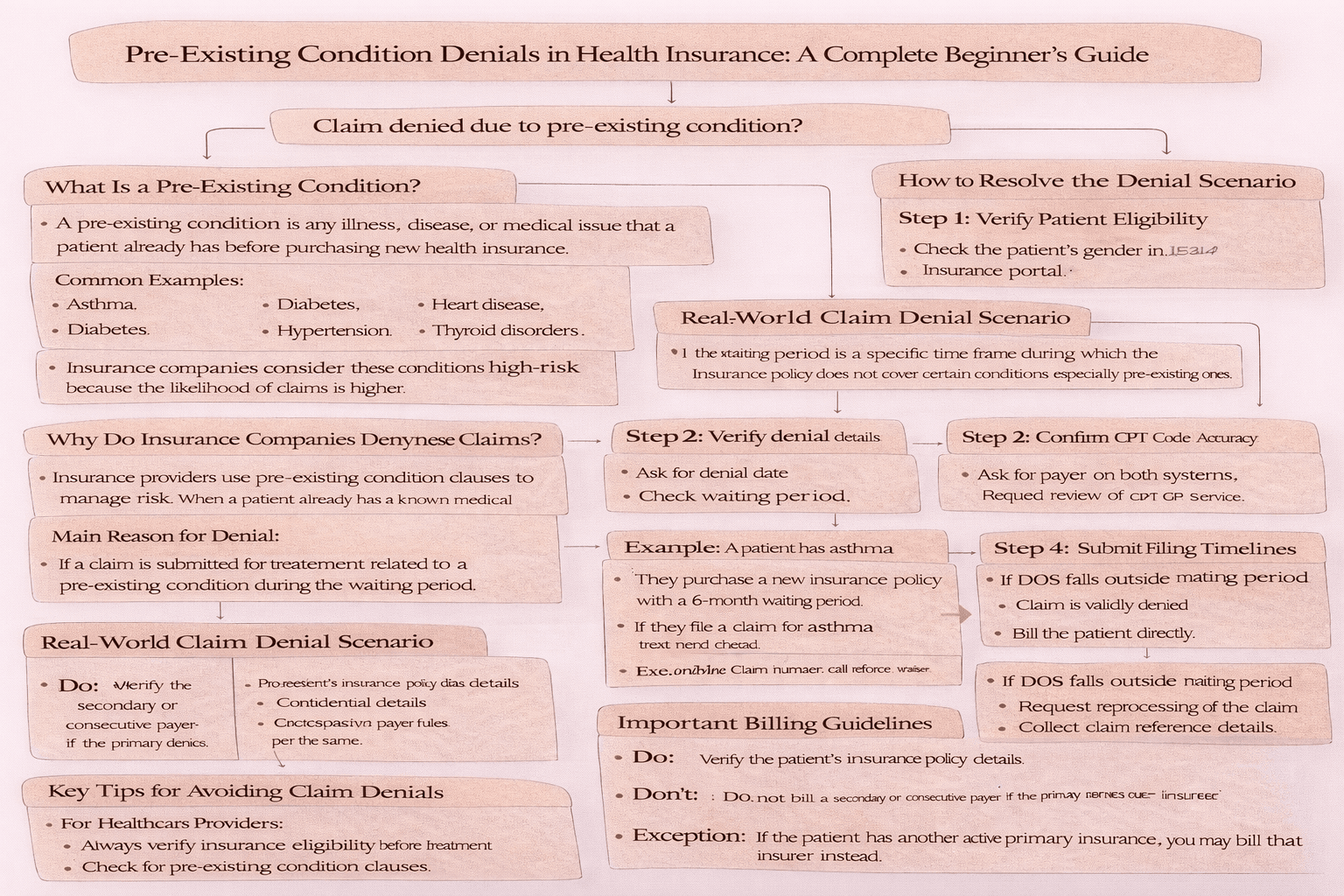
Health insurance is meant to protect patients from unexpected medical expenses. However, not all claims are approved. One common reason for claim denial is a pre-existing condition. If you’ve ever encountered a denial stating “non-covered services due to pre-existing condition,” it can be confusing and frustrating. In this article, we’ll break down what pre-existing condition denials mean, why they happen, how waiting periods work, and what steps healthcare professionals and patients can take to handle such situations effectively.
What Is a Pre-Existing Condition?
A pre-existing condition is any illness, disease, or medical issue that a patient already has before purchasing a new health insurance policy.
Common Examples:
Asthma
Diabetes
Hypertension
Heart disease
Thyroid disorders
Insurance companies consider these conditions high-risk because the likelihood of claims is higher.
Why Do Insurance Companies Deny These Claims?
Insurance providers use pre-existing condition clauses to manage risk. When a patient already has a known medical condition, insurers may exclude coverage entirely, apply a waiting period, or increase premium costs significantly.
Main Reason for Denial:
If a claim is submitted for treatment related to a pre-existing condition during the waiting period, the insurer will deny it as non-covered services.
Understanding the Waiting Period
The waiting period is a specific time frame during which the insurance policy does not cover certain conditions, especially pre-existing ones.
How It Works:
The policy begins on Day 1
A waiting period (e.g., 6 months or 12 months) is applied
Claims related to pre-existing conditions are not covered during this time
Example:
A patient has asthma
They purchase a new insurance policy with a 6-month waiting period
If they file a claim for asthma treatment within those 6 months → Claim will be denied
After the waiting period ends, the same claim may be eligible for coverage.
Real-World Claim Denial Scenario
Here’s a simplified flow of how such denials are handled in practice:
Step-by-Step Process:
Claim is denied
Reason: Pre-existing condition not covered
Verify denial details
Ask for denial date
Check waiting period
Confirm start and end dates
Compare with Date of Service (DOS)
If DOS falls within waiting period:
Claim is validly denied
Bill the patient directly
If DOS falls outside waiting period:
Request reprocessing of the claim
Ask for Turnaround Time (TAT)
Collect claim reference details
Important Billing Guidelines
When dealing with pre-existing condition denials, it’s critical to follow proper billing protocols:
Do:
Verify the patient’s insurance policy details
Confirm waiting period timelines
Keep documentation of claim and call reference numbers
Don’t:
Do not bill a secondary or consecutive payer if the primary denies due to pre-existing condition
Do not assume coverage without checking policy terms
Exception:
If the patient has another active primary insurance, you may bill that insurer instead.
Key Tips for Avoiding Claim Denials
For Healthcare Providers:
Always verify insurance eligibility before treatment
Check for pre-existing condition clauses
Educate patients about waiting periods
Maintain clear documentation
For Patients:
Disclose all medical history honestly
Understand your policy terms before purchasing
Ask about waiting periods and exclusions
Consider policies that offer shorter waiting periods
Frequently Asked Questions (FAQs)
1. What happens if I don’t disclose a pre-existing condition?
Failure to disclose can lead to claim rejection or even policy cancellation.
2. Can pre-existing conditions ever be covered?
Yes, most insurers cover them after the waiting period ends, depending on policy terms.
3. How long is a typical waiting period?
It usually ranges from 6 months to 4 years, depending on the insurer and condition.
4. Can I appeal a denied claim?
Yes, if you believe the denial is incorrect (for example, service occurred after the waiting period), you can request reprocessing or file an appeal.
5. Will all insurers treat pre-existing conditions the same way?
No, policies vary. Some insurers offer reduced waiting periods or higher premiums for immediate coverage.
Conclusion
Pre-existing condition denials are a common but manageable part of health insurance processing. The key lies in understanding policy terms, waiting periods, and proper billing practices. For healthcare professionals, accurate verification and documentation can prevent unnecessary delays and revenue loss. For patients, awareness and transparency can help avoid unexpected claim rejections. By staying informed and proactive, both providers and patients can navigate these denials effectively and ensure smoother healthcare and insurance experiences.