In medical billing, claim denials are a common challenge but some are easier to fix than others once you understand the root cause. One such denial is MA120, which indicates a missing, incomplete, or invalid CLIA certification number. If you’re new to healthcare revenue cycle management or just encountering this denial for the first time, this guide will walk you through everything you need to know what CLIA is, why this denial happens, and how to resolve it efficiently.
What is a CLIA Certification Number?
CLIA stands for Clinical Laboratory Improvement Amendments. It is a regulatory program that ensures quality standards for laboratory testing. A CLIA number is a unique identifier assigned to a laboratory, required when billing for lab tests, and used by payers to verify that the lab is certified to perform testing.
Why is CLIA Important in Billing?
When a lab test is billed, the payer checks whether the performing lab is CLIA certified. The claim must include a valid CLIA number, and missing or incorrect CLIA details result in denial like MA120.
What Does MA120 Denial Mean?
The MA120 denial code indicates missing, incomplete, or invalid CLIA certification number.
Common Reasons for This Denial
CLIA number is missing from the claim such as Box 23 or electronic equivalent.
Incorrect or expired CLIA number.
CLIA number does not match the billing provider or facility.
Lab is not CLIA certified.
Required modifiers like QW are missing for waived tests.
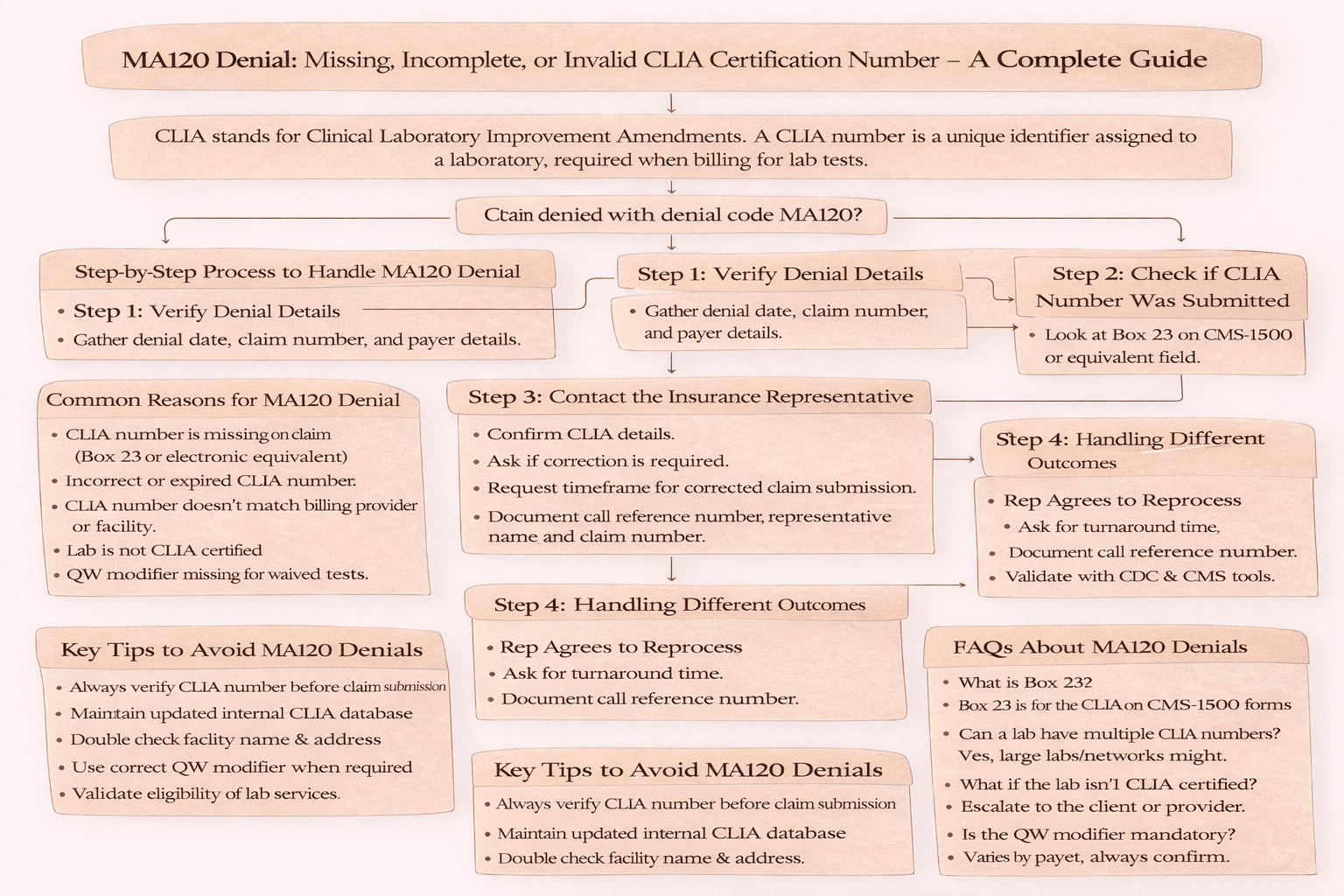
Step-by-Step Process to Handle MA120 Denial
Below is a simplified workflow you can follow when working on this denial.
1. Verify Denial Details
Start by gathering denial date, claim number, and payer details.
2. Check if CLIA Number Was Submitted
Look at Box 23 on CMS 1500 form or equivalent field in electronic claims and internal billing system.
Scenario A: CLIA Number is Present
Confirm with payer if the number is correct and ask them to verify if the CLIA number on the claim is valid. If correct, request reprocessing of the claim. If incorrect, ask for the correct CLIA number and proceed to correction and resubmission.
Scenario B: CLIA Number is Missing
Identify the correct CLIA number and update the claim before resubmission.
3. Contact the Insurance Representative
During the call, confirm CLIA details, ask if correction is required, and request timeframe for corrected claim submission. Always document call reference number, representative name, and claim number.
4. Handling Different Outcomes
If the representative agrees to reprocess, ask for turnaround time and call reference number. If correction is required, obtain correct CLIA number, ask submission timeframe, update, and resubmit the claim. If the representative refuses to provide CLIA, use external tools and validate independently.
How to Find the Correct CLIA Number
If the CLIA number is missing or incorrect, you can use official lookup tools.
Key sources include CDC CLIA lookup tool where you can search by CLIA number or laboratory name, and CMS CLIA database where you can search by facility name, address, or CLIA number.
Tips while searching: facilities may have multiple CLIA numbers, so always match address and facility name and confirm the correct location.
What If You Can’t Find the CLIA Number?
If the lab is not found in either database, it may not be CLIA certified. In that case, escalate to the client or billing supervisor.
Important Billing Considerations
Use QW modifier for waived tests as it is required for CLIA waived lab services and must be billed along with CLIA number.
If you cannot update the claim due to system access limitations, assign the task to client or clearinghouse team.
Always document everything including claim number, call reference number, actions taken, and timelines.
Key Tips to Avoid MA120 Denials
Always verify CLIA number before claim submission.
Maintain updated CLIA database internally.
Double check facility name and address.
Use correct modifiers such as QW when applicable.
Validate eligibility of lab services.
Example Scenario
Situation: Claim denied with MA120
Action taken: checked claim and found CLIA number missing, searched CMS portal and found correct CLIA, updated claim, and resubmitted within payer timeframe.
Result: Claim processed successfully.
Frequently Asked Questions (FAQs)
1. What is Box 23 in a claim form?
Box 23 is used to enter the CLIA number on a CMS 1500 claim form when billing lab services.
2. Can one facility have multiple CLIA numbers?
Yes, especially large labs or networks, so always match the correct address and department.
3. What happens if a lab is not CLIA certified?
The claim will likely be denied and you must escalate the issue to the client or provider.
4. Is the QW modifier mandatory?
Yes, for CLIA waived tests, the QW modifier is required along with the CLIA number.
5. How long do I have to resubmit a corrected claim?
It varies by payer, so always confirm the timely filing limit with the representative.
Conclusion
The MA120 denial may seem technical, but it is highly manageable once you understand the process. It mainly revolves around verifying and correcting the CLIA certification number. By following a structured workflow checking claim details, validating CLIA numbers, and communicating effectively with payers you can resolve these denials quickly and prevent future occurrences. Consistency, documentation, and attention to detail are your best tools in avoiding MA120 issues and ensuring smooth claim processing.