In medical billing, claim denials are a common challenge that can delay payments and disrupt revenue cycles. One such denial is Denial Code 199: Revenue Code and Procedure Code Do Not Match.
If you’re new to healthcare billing or revenue cycle management, this error might seem confusing, but it becomes manageable once you understand the root cause and resolution steps.
This guide explains the denial in simple terms, how to handle it, and how to prevent it.
What is Denial Code 199?
Denial Code 199 occurs when the revenue code billed does not align with the procedure code submitted on the claim.
Breaking it Down
Revenue code indicates the department or service category such as room charges or lab services.
Procedure code (CPT or HCPCS) specifies the exact service or procedure performed.
When these two do not logically match, the insurance payer denies the claim.
Why Does This Denial Happen?
1. Incorrect Code Pairing
A CPT code is assigned that does not belong to the selected revenue code category.
2. Data Entry Errors
Manual mistakes during charge entry or claim submission.
3. Outdated Coding Guidelines
Using incorrect or old coding combinations.
4. System Mapping Issues
Billing software incorrectly maps CPT codes to revenue codes.
Real-World Example
Revenue Code 0450 (Emergency Room)
CPT Code 80050 (General Health Panel)
These do not match because lab services should be billed under a lab revenue code, not emergency room.
Result: Denial Code 199
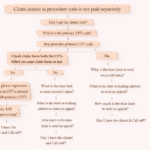
Step-by-Step Process to Resolve Denial Code 199
Step 1: Check Denial Details
Confirm the denial date and review the EOB or ERA.
Step 2: Review Patient Payment History
Check if the same CPT and revenue code combination was previously paid.
Scenario A: If Previously Paid
Contact the payer and request reprocessing of the claim.
Ask for reason for inconsistency.
Collect claim number, call reference number, and turnaround time.
Scenario B: If Not Previously Paid
Ask the payer if they can suggest the correct revenue code or CPT code.
Note that payers may not always provide this information.
Step 3: Consult Coding Team
Assign the case to the coding team with denial details and payer feedback.
They will validate the coding and recommend corrections if needed.
Step 4: Submit Corrected Claim
If correction is required, update the correct revenue code or CPT code and submit a corrected claim.
Always check timely filing limits before resubmission.
Step 5: Appeal if Necessary
If coding is already correct, prepare and submit an appeal with supporting documentation, coding justification, and medical necessity.
Ask for appeal deadline and submission details.
Step 6: Track and Document
Always document claim number, call reference number, and actions taken.
Important Notes for Billing Teams
Always involve the coding team to confirm whether the denial is valid or requires correction.
Follow timely filing limits strictly when submitting corrected claims or appeals.
Follow client-specific instructions, even in cases where timelines are exceeded.
If no action is allowed due to deadlines, write off the claim as per guidelines.
Tips to Prevent Denial Code 199
Use updated coding guidelines
Implement claim validation edits in billing software
Train staff regularly on correct coding combinations
Perform pre-bill audits
Maintain access to coding manuals and payer guidelines
Quick Checklist for Resolution
Verify denial reason
Check payment history
Contact payer if needed
Assign to coding team
Correct and resubmit or appeal
Track timelines
Document everything
Frequently Asked Questions (FAQs)
1. What is the difference between a revenue code and a CPT code?
A revenue code identifies the service category, while a CPT code describes the exact procedure performed.
2. Can I correct the claim without contacting the payer?
Yes, if the error is clear and confirmed by the coding team.
3. What if the payer does not provide the correct code?
Use internal coding guidelines or consult the coding team.
4. How long do I have to fix this denial?
It depends on the payer’s timely filing limit, usually between 30 and 180 days.
5. When should I appeal instead of correcting the claim?
If the coding is correct and follows guidelines, you should appeal instead of modifying the claim.
Conclusion
Denial Code 199 is a common but preventable issue in medical billing. By understanding how revenue codes and procedure codes work together, reviewing claims carefully, and involving the coding team, you can resolve these denials efficiently.
A structured approach helps: verify, review, correct, and resubmit or appeal.
With proper validation, training, and attention to detail, you can reduce these denials and improve overall revenue cycle performance.