In medical billing and revenue cycle management, denial codes can be confusing—especially for beginners. One commonly encountered denial is Denial Code 100: Payment Made to Patient/Insured/Responsible Party.
This denial occurs when the insurance company sends payment directly to the patient instead of the healthcare provider. As a result, providers are left unpaid and must take additional steps to recover the amount.
Understanding why this happens and how to handle it efficiently is crucial for maintaining a healthy revenue cycle. This guide breaks down everything you need to know in simple terms.
What is Denial Code 100?
Denial Code 100 indicates that:
The insurance company has processed the claim
The claim has been paid
But the payment was sent directly to the patient, not the provider
This means the provider must now collect the payment from the patient instead of the insurer.
Why Does Denial Code 100 Occur?
- Missing Assignment of Benefits (AOB)
The Assignment of Benefits (AOB) is a form signed by the patient.
It allows the insurance company to pay the provider directly.
If this form is not signed or missing, payment goes to the patient. - Out-of-Network Provider
If the provider is not part of the insurance network, the insurer may:
Still process the claim
But send payment to the patient instead of the provider - Patient’s Insurance Plan Rules
Some insurance plans are structured to:
Always pay the patient first
Leave it up to the patient to pay the provider
What Happens in This Scenario?
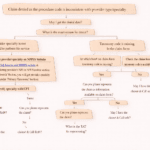
Here’s a simplified flow of events:
Claim is submitted by the provider
Insurance processes the claim
Payment is issued
Payment is sent to the patient
Provider receives a denial (Code 100)
Step-by-Step: How to Handle Denial Code 100
Step 1: Verify Claim Details
Start by gathering key information:
Processed date
Paid date
Allowed amount (AA)
Paid amount (PA)
Patient responsibility (PTR):
Coinsurance
Deductible
Copayment
Step 2: Validate Financial Accuracy
Make sure:
Paid Amount (PA) + Patient Responsibility (PTR) = Allowed Amount (AA)
If the numbers don’t match:
Contact the insurance representative
Clarify and correct the details
Step 3: Confirm Payment Destination
Ask:
Why was the payment sent to the patient?
Was AOB missing?
Is the provider out-of-network?
Step 4: Collect Reference Information
Always document:
Claim number
Call reference number
This helps in future follow-ups or audits.
What Should You Do Next?
- Bill the Patient Directly
Since the insurer has already paid the patient:
The provider should bill the patient
Include:
Explanation of Benefits (EOB)
Clear payment instructions - Do NOT Bill Secondary Insurance
Important rule:
This denial is not transferable
Do not send it to:
Secondary payer
Tertiary payer
It is fully the patient’s responsibility
- No Need to Track Payment
The payment was sent to the patient
Providers cannot track or retrieve it from insurance
Focus only on patient collection
Example Scenario
Let’s make this easier with an example:
Allowed Amount: ₹10,000
Insurance Paid: ₹7,000 (to patient)
Patient Responsibility: ₹3,000
What happens?
The patient receives ₹7,000
The provider must collect the full ₹10,000 from the patient
The patient is expected to pay using:
Insurance payment + personal share
Key Tips for Managing Denial Code 100
Preventive Measures
Always ensure AOB is signed before services
Verify network status before treatment
Educate patients about payment responsibilities
Operational Tips
Maintain proper documentation
Use clear billing statements
Follow up with patients promptly
Communication Tips
Be transparent with patients
Explain why they received the payment
Offer payment plans if needed
Common Mistakes to Avoid
Billing secondary insurance
Ignoring the denial
Not verifying AOB status
Delaying patient billing
Assuming insurance will reissue payment
Frequently Asked Questions (FAQs)
- Can the provider request payment from insurance again?
No. Once payment is made to the patient, the insurer will not reissue it to the provider. - What if the patient refuses to pay?
The provider may:
Send reminders
Offer payment plans
Escalate to collections (if necessary) - Is Denial Code 100 an actual denial?
Not exactly. The claim is paid, but the payment is redirected to the patient. - Can this denial be appealed?
Usually, no. It’s not a denial based on medical necessity or coding—it’s a payment routing issue. - How can providers avoid this in the future?
Always collect signed AOB forms
Verify insurance details before service
Confirm whether the plan pays providers directly
Conclusion:
Denial Code 100 can be frustrating, but it’s manageable once you understand the process. The key takeaway is simple: the claim is paid, but the money is in the patient’s hands.
To handle this efficiently:
Verify claim details carefully
Understand why payment went to the patient
Bill the patient promptly
Avoid unnecessary rework like billing secondary insurance
By following a structured approach and focusing on prevention, healthcare providers can minimize revenue loss and streamline their billing operations.
If you’re working in medical billing, mastering scenarios like Denial Code 100 will significantly improve your efficiency and accuracy.