In medical billing, one of the most common reasons for claim denials is confusion between new patient and established patient codes. These are part of Evaluation and Management (E/M) coding, and selecting the wrong code can directly impact reimbursement. If you’re new to healthcare billing or working in revenue cycle management, understanding this distinction is essential. This guide breaks down the concept in simple terms, explains common denial scenarios, and provides actionable tips to avoid mistakes.
What is a New Patient?
A new patient is someone who is visiting the provider for the first time or has not received any professional services from the same physician or another physician of the same specialty in the same group practice within the last 3 years.
New Patient CPT Codes
99202
99203
99204
99205
These codes generally involve more detailed documentation because the provider is evaluating the patient for the first time.
What is an Established Patient?
An established patient is someone who has received services from the same physician or another physician of the same specialty in the same group within the past 3 years.
Established Patient CPT Codes
99211
99212
99213
99214
99215
These visits are typically less complex since the provider already has the patient’s medical history.
Why This Distinction Matters
Choosing the correct patient type is critical because it affects reimbursement rates, determines documentation requirements, and directly impacts claim approval or denial. Common issue: insurance companies frequently deny claims when the patient status is incorrectly coded.
Understanding the 3-Year Rule
The 3-year rule is the backbone of this classification.
If a patient has not been seen in 3 years they are considered a new patient.
If a patient has been seen within 3 years they are considered an established patient.
Example
Patient visited in January 2022
Returns in March 2025 → still an established patient (within 3 years)
Returns in February 2026 → considered a new patient (more than 3 years)
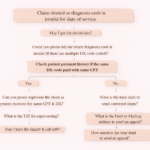
Common Denial Scenario (Step-by-Step Workflow)
When a claim is denied due to patient status mismatch, follow this structured approach.
Step 1: Identify the Issue
Claim denied for new or established patient criteria not met.
Step 2: Gather Basic Details
Ask for denial date and claim number.
Step 3: Check Billed CPT Code
Verify whether it is a new patient code (99202 to 99205) or an established patient code (99211 to 99215).
Step 4: Verify Patient History
Check your system to confirm whether the patient received services in the last 3 years.
Scenario-Based Resolution
Scenario 1: New Patient Code Billed but Denied as Established
Check internal records for past visits. If no history is found, call insurance to verify. If insurance confirms a prior visit, send to coding team for correction. If no prior visit is found, request claim reprocessing.
Scenario 2: Established Patient Code Billed but Denied as New
Check patient history in the system. If a visit exists within 3 years, contact insurance and request reprocessing. If no visit exists, assign to coding team to update CPT.
Important Coding Guidelines
Do not change codes without authorization. E/M coding depends on medical history, examination, and time spent. If you are not a certified coder, do not modify CPT codes independently and always consult the coding team.
Key Tips to Avoid Denials
Always verify patient visit history.
Follow the 3-year rule strictly.
Double check CPT codes before submission.
Maintain accurate patient records.
Confirm discrepancies with insurance when needed.
Document call reference numbers for tracking.
Quick Comparison Table
Criteria: New Patient vs Established Patient
Visit history: No visit in last 3 years vs Seen within last 3 years
CPT codes: 99202 to 99205 vs 99211 to 99215
Documentation: More detailed vs Moderate
Risk of denial: High if history unclear vs High if misclassified
Frequently Asked Questions (FAQs)
1. What if a patient saw a different doctor in the same hospital?
If the doctor is of the same specialty and same group practice, the patient is still considered established.
2. Does location matter such as different clinic branches?
No, if it is the same group practice, location does not change patient status.
3. What if records are missing in the system?
Always contact the insurance provider, confirm patient history, and document the conversation.
4. Can a patient be both new and established?
No, a patient can only fall into one category per visit based on the 3-year rule.
5. Who decides the final CPT code?
The certified coding team determines the correct code based on clinical documentation.
Conclusion
Understanding the difference between new and established patient codes is fundamental in medical billing. Most denials occur due to simple oversights primarily failure to verify patient history within the 3-year window. By following a structured workflow, verifying records carefully, and collaborating with the coding team, you can significantly reduce claim denials and improve reimbursement efficiency. Treat this process not just as a checklist but as a quality control mechanism in your billing workflow. Accuracy here directly translates into faster payments and fewer rework cycles.