In medical billing, claim denials are a common challenge, and one frequently encountered issue is: “Procedure code is inconsistent with the provider type/specialty (taxonomy).” This denial can delay reimbursements and increase administrative workload if not handled correctly. If you’re new to medical billing or revenue cycle management, this guide will help you understand what this denial means, why it occurs, and how to resolve it efficiently. We’ll also walk through a practical approach and share tips to prevent future denials.
What Does This Denial Mean?
This denial occurs when the procedure code (CPT/HCPCS) billed does not align with the provider’s specialty or taxonomy code listed in the claim. In simple terms: Insurance payers expect certain procedures to be performed only by specific provider types. If the billed service doesn’t match the provider’s specialty, the claim is rejected.
Understanding Key Components
- Procedure Code (CPT/HCPCS) – Represents the service provided (e.g., surgery, consultation, diagnostic test).
- Provider Specialty – Defines the provider’s medical field (e.g., cardiology, dermatology).
- Taxonomy Code – A unique code identifying provider classification and specialization, linked to NPI.
Common Reasons for This Denial
- Mismatch Between CPT Code and Specialty – Procedure not typical for that specialty.
- Missing Taxonomy Code – Not included in claim.
- Incorrect Taxonomy Code – Wrong code submitted.
- System or Submission Errors – Data transmission issues.
Step-by-Step Process to Resolve the Denial
Step 1: Gather Basic Information – Get denial date and exact reason.
Step 2: Identify Root Cause
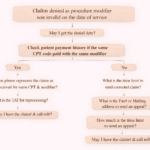
Scenario A: Specialty Not Allowed – Check NPI registry → Compare CPT vs specialty → If mismatch: escalate; If correct: request reprocess.
Scenario B: Taxonomy Missing – Check CMS-1500 (Box 24J, 33b) → If present: ask reprocess/resubmit → If missing: correct and resubmit.
Step 3: Communicate with Payer – Ask for reprocessing; If accepted: get TAT; If denied: collect claim & call reference.
Key Tips to Prevent This Denial
Verify taxonomy regularly; Match CPT with specialty; Audit claims before submission; Use updated billing systems; Train staff.
Practical Example
General physician bills a surgical procedure → denied → Check taxonomy → mismatch found → Correct provider details or escalate → Resubmit claim.
Frequently Asked Questions (FAQs)
- What is a taxonomy code in medical billing? A taxonomy code is a 10-character code that identifies a provider’s specialty and classification, linked to the NPI.
- Where is the taxonomy code located on a CMS-1500 form? Rendering provider: Box 24J; Billing provider: Box 33b.
- Can a claim be reprocessed without resubmission? Yes, if correct information is already present, payer can reprocess.
- What should I do if taxonomy is missing after submission? Resubmit claim with correct taxonomy; if issue continues, escalate to billing/clearinghouse team.
- How can I check a provider’s specialty? Use NPI registry, enter NPI, and review primary taxonomy.
Conclusion:
This denial is common but manageable. By verifying provider details, ensuring CPT-specialty alignment, and following a structured workflow, you can resolve issues quickly and improve claim success rates. A strong understanding of taxonomy and accurate claim submission helps strengthen overall revenue cycle performance.