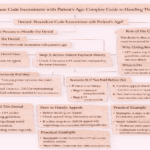
In medical billing, claim denials are a routine yet critical challenge. One common denial reason is “Procedure code was invalid on the date of service.” This issue can delay reimbursements, increase administrative workload, and impact revenue cycles if not handled correctly.
For beginners in medical billing and revenue cycle management (RCM), understanding this denial and how to resolve it efficiently is essential. This guide breaks down the concept in simple terms, outlines the step-by-step resolution process, and provides practical tips to avoid future occurrences.
What Does “Procedure Code Invalid on Date of Service” Mean?
This denial occurs when a CPT (Current Procedural Terminology) code submitted on a claim is not valid or not active for the specific date the service was performed.
Common Reasons for This Denial
The CPT code was not yet effective on the date of service
The CPT code was expired or discontinued
Incorrect use of new vs. established patient codes
Coding errors or outdated coding references
System or data entry mistakes
Example:
A provider bills CPT code 99204 for a visit in 2019, but due to coding updates, the payer considers it invalid for that date. The claim is denied.

Step-by-Step Process to Handle This Denial
Handling this denial requires a structured approach. Below is a simplified workflow used in medical billing operations:
- Verify Denial Details
Start by gathering key information:
Denial date
Claim number
Explanation of Benefits (EOB) details
This helps determine timelines and next steps.
- Check Payment History
Verify whether the same insurance has previously paid for the same CPT code.
Scenario A: Payment Found
If the same CPT was previously paid:
Request reprocessing of the claim
Provide proof of prior payment if needed
Ask for:
Turnaround Time (TAT)
Call reference number
Scenario B: No Payment Found
If no prior payment exists:
Confirm the timely filing limit for corrected claims
Gather:
Fax number or mailing address for appeals
Appeal submission deadline
- Assign to Coding Team
This is a critical step.
Send the claim to the coding team to:
Review the procedure code
Validate whether it was correctly coded
Suggest a corrected CPT code if necessary - Take Action Based on Coding Feedback
If Code is Incorrect:
Update the CPT code
Submit a corrected claim (if within time limit)
If Code is Correct:
File an appeal with supporting documentation
- Track Timely Filing Limits
Timelines are crucial in medical billing.
Corrected claims must be submitted within payer-defined limits
Appeals must be filed within a specific timeframe from the denial date
If timelines are exceeded:
The claim may need to be written off
Or proceed based on client instructions (some clients allow late submissions)
Important Considerations
- Client-Specific Instructions
Sometimes clients may request:
Submission of corrected claims even after time limits
Appeals despite expired deadlines
Always follow client guidelines carefully.
- New vs. Established Patient Errors
A frequent cause of this denial is incorrect classification:
New patient: No visit within the past 3 years
Established patient: Seen within the past 3 years
Using the wrong category can trigger invalid code denials.
- Documentation Matters
Ensure:
Proper clinical documentation supports the CPT code
Coding aligns with payer guidelines
Incomplete documentation can lead to repeated denials.
Key Tips to Avoid This Denial
Preventing denials is more efficient than fixing them. Here are some practical tips:
Stay Updated with CPT Changes
CPT codes are updated annually
Always use the latest coding manuals
Use Coding Software or Tools
Automated systems help detect invalid or outdated codes
Verify Code Validity Before Submission
Check if the CPT code is active for the service date
Train Billing and Coding Teams
Regular training reduces human errors
Maintain Communication Between Teams
Billing and coding teams should collaborate closely
FAQs
- What is a CPT code?
A CPT code is a standardized code used to describe medical, surgical, and diagnostic services for billing purposes. - Why would a valid CPT code be denied?
Even valid codes can be denied if they were not active on the date of service or used incorrectly. - Can I resubmit a denied claim?
Yes, you can submit a corrected claim if it is within the payer’s timely filing limit. - What if the time limit has passed?
Typically, the claim is written off unless the client instructs otherwise or an exception is granted. - When should I file an appeal?
File an appeal when:
The CPT code is correct
Documentation supports the service
The denial is unjustified
Conclusion:
The denial “Procedure code was invalid on the date of service” is common but manageable with the right approach. By verifying denial details, checking payment history, involving the coding team, and adhering to timelines, you can resolve these issues efficiently.
For beginners, the key is to understand the root cause, follow a structured workflow, and maintain strong coordination between billing and coding teams. Preventive measures like staying updated with CPT changes and validating codes before submission can significantly reduce such denials.
Mastering these processes not only improves claim acceptance rates but also strengthens the overall revenue cycle management system.