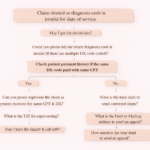
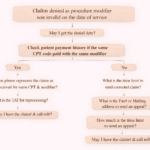
In medical billing, claim denials are a common challenge that can slow down reimbursements and impact revenue cycles. One frequently encountered denial is Denial Code 150, which states: “Payer deems the information submitted does not support this level of service.”
For beginners, this message can feel vague and confusing. What exactly does it mean? Why was the claim denied? And most importantly—how can you fix it?
This article breaks down Denial Code 150 in simple terms, explains the common reasons behind it, and provides practical steps to resolve and prevent it.
What is Denial Code 150?
Denial Code 150 indicates that the insurance payer believes the documentation or information submitted does not justify the level of service billed.
In simpler terms, the provider billed for a service (often a higher-level procedure or evaluation), but the payer thinks the medical records do not support that level.
Common Reasons for Denial Code 150
This denial usually occurs due to three main reasons:
- CPT Code Maximum Allowance Reached
Insurance plans often limit how many times a specific CPT code can be billed within a certain time frame.
Example:
A patient receives physical therapy sessions, but the payer allows only 10 sessions per year. If the provider bills for the 11th session, the claim may be denied under Code 150.
- Lack of Medical Necessity or Coding Issues
This is one of the most frequent causes.
The service billed may be considered not medically necessary
The level of service may be overcoded (upcoding)
Diagnosis codes may not support the procedure performed
Example:
A high-level evaluation is billed, but the documentation only supports a basic consultation. The payer denies it because the service level is not justified.
- Medical Records Requested or Insufficient Documentation
Sometimes the payer needs additional proof.
Missing clinical notes
Incomplete documentation
No supporting evidence for the procedure
Example:
A complex surgical procedure is billed, but operative notes are missing. The payer denies the claim until proper documentation is provided.
How to Identify the Exact Issue
Before taking action, always check the Remark Codes associated with the denial.
These codes provide more specific details about why the claim was denied.
Steps to Identify the Issue:
Review the Explanation of Benefits (EOB) or Electronic Remittance Advice (ERA)
Look for remark codes or additional notes
Cross-check with submitted documentation
Verify payer policies
Step-by-Step Resolution Process
Step 1: Analyze the Denial
Identify whether the issue is related to:
Frequency limits
Medical necessity
Documentation
Step 2: Verify Coding Accuracy
Check CPT and ICD codes
Ensure correct modifiers are used
Confirm the level of service matches documentation
Step 3: Review Medical Records
Ensure documentation supports:
Diagnosis
Procedure performed
Level of care
Step 4: Take Corrective Action
If Maximum Allowance Reached:
Verify payer policy
Appeal only if an exception applies (e.g., medical necessity)
If Medical Necessity Issue:
Add supporting documentation
Submit corrected claim or appeal
If Documentation Missing:
Attach required medical records
Resubmit claim or respond to payer request
Step 5: Submit Appeal (if applicable)
Include:
Detailed explanation letter
Supporting clinical documentation
Corrected coding (if needed)
Practical Example
Let’s say a provider bills for a Level 4 office visit, but the documentation only supports a Level 2 visit.
What happens?
The payer reviews the claim
Finds insufficient justification
Issues Denial Code 150
Fix:
Either downgrade the code and resubmit
Or provide additional documentation proving higher complexity
Key Tips to Prevent Denial Code 150
Document thoroughly: Always ensure clinical notes justify the service level
Avoid upcoding: Match the service level accurately with documentation
Check payer guidelines: Each payer has different rules
Use correct diagnosis codes: Ensure they support the procedure
Track frequency limits: Avoid exceeding allowed service counts
Audit claims regularly: Catch errors before submission
FAQs
- What does “level of service” mean?
It refers to the complexity and intensity of care provided, often represented by CPT codes. Higher levels require more detailed documentation. - Can Denial Code 150 be appealed?
Yes, if you can provide sufficient documentation proving that the billed service level was appropriate. - How do I know if it’s a coding issue?
Check if the CPT code matches the documentation. If the service appears overcoded or mismatched, it’s likely a coding issue. - What if medical records were requested?
Submit the requested records promptly. Ensure they clearly support the billed service. - Is this denial always avoidable?
Not always, but proper documentation, accurate coding, and payer policy checks can significantly reduce occurrences.
Conclusion:
Denial Code 150 may seem complex at first, but it essentially comes down to one key issue: the payer is not convinced that the billed service level is justified.
By understanding the common causes—such as frequency limits, medical necessity issues, and missing documentation—you can quickly identify the root problem and take corrective action.
The best way to handle this denial is prevention. Accurate coding, strong documentation, and regular audits can help ensure that your claims are accepted the first time, improving both efficiency and revenue flow.
Mastering Denial Code 150 is an important step toward becoming more effective in medical billing and revenue cycle management.