Health insurance can feel confusing, especially when terms like deductible, co-payment, and coinsurance come into play. One of the most important concepts to understand is the deductible amount—because it directly impacts how much you pay out of pocket before your insurance starts contributing. In this guide, we’ll break down the deductible in simple terms, explain how it works with real-life scenarios, and walk you through how it affects claim processing. Whether you’re new to insurance or looking to refresh your knowledge, this article will help you clearly understand the concept.
What is a Deductible Amount?
A deductible is a fixed amount that a policyholder must pay before the insurance company starts paying for medical expenses.
Simple Definition:
It’s the amount you pay first, out of your own pocket, before your insurance kicks in.
Example:
Deductible: $2,000
Medical bill: $1,500
Insurance pays: $0
You pay: $1,500 (applied toward deductible)
You still have $500 left to meet your deductible.
How Deductibles Work: Step-by-Step Example
Let’s understand this with a real scenario:
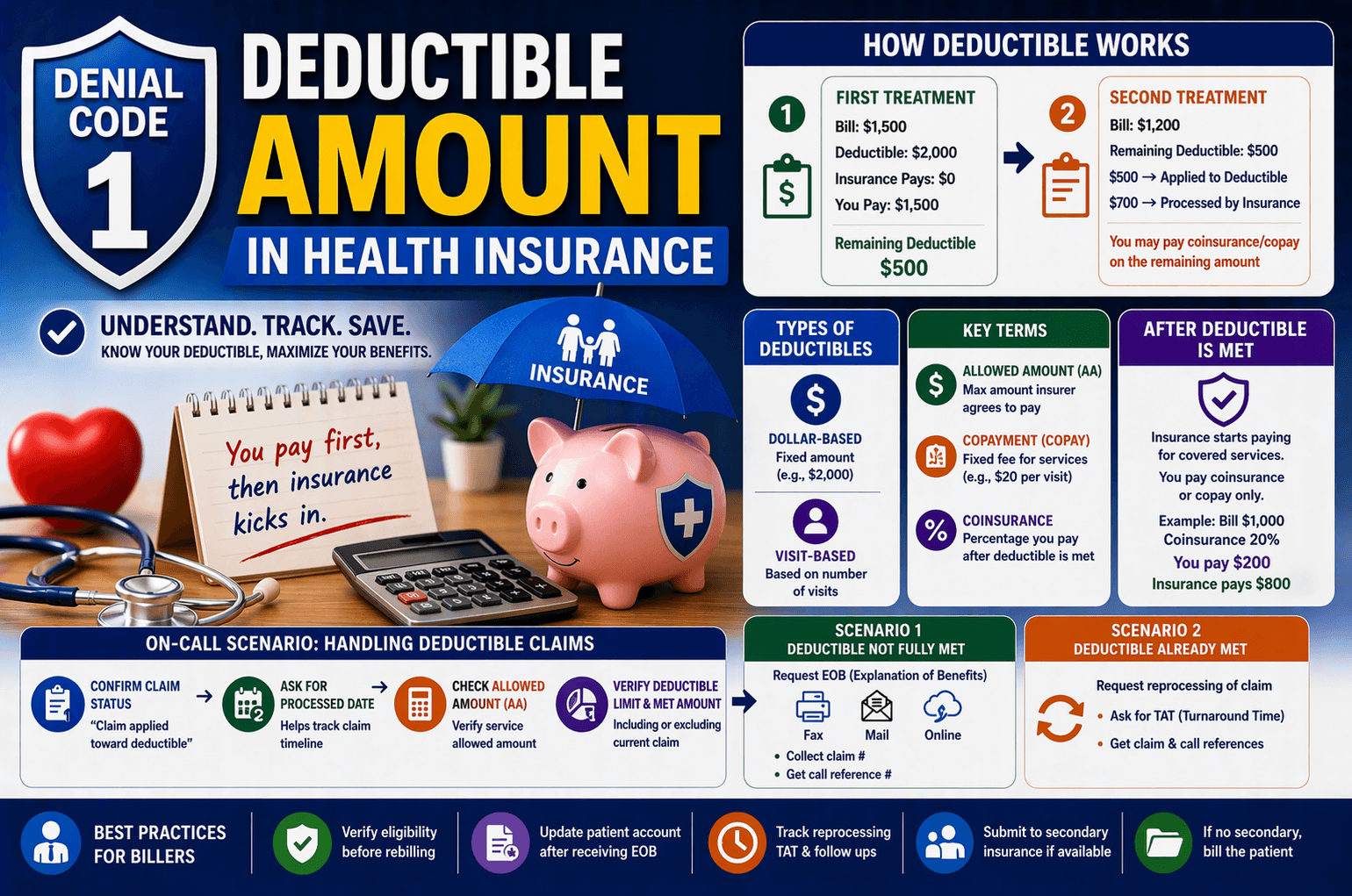
First Treatment
Treatment cost: $1,500
Deductible: $2,000
Insurance pays: $0
Patient pays: $1,500
Remaining deductible: $500
Second Treatment
Treatment cost: $1,200
Remaining deductible: $500
Now:
$500 → applied to deductible
Remaining $700 → processed by insurance
However, from this $700:
You may still pay a portion (coinsurance/copay)
Types of Deductibles
Deductibles can be structured in different ways depending on the insurance policy.
1. Dollar-Based Deductible
Fixed monetary amount (e.g., $1,000, $2,000)
Most common type
2. Visit-Based Deductible
Based on the number of visits
Example: First 3 visits fully paid by patient
After reaching the limit, insurance starts covering costs.
Key Terms You Should Know
Understanding deductibles becomes easier when you know related terms:
Allowed Amount (AA)
The maximum amount an insurer agrees to pay for a service.
Copayment (Copay)
A fixed fee you pay for services (e.g., $20 per visit).
Coinsurance
A percentage of the cost you share with the insurer after deductible is met.
On-Call Scenario: Handling Deductible Claims
When working in medical billing or insurance follow-up, here’s a typical flow when a claim is applied to a deductible:
Step-by-Step Process:
Confirm Claim Status
“Claim applied toward deductible”
Ask for Processed Date
Helps track claim timeline
Check Allowed Amount (AA)
Verify Deductible Limit
Total deductible for the policy
Check Deductible Met Amount
Including or excluding current claim
Decision Paths
Scenario 1: Deductible NOT Fully Met
Request EOB (Explanation of Benefits)
Options:
Fax
Mail
Online source
Collect:
Claim number
Call reference number
Scenario 2: Deductible Already Met
Request reprocessing of claim
Ask:
Turnaround Time (TAT)
Claim reference details
What Happens After Deductible is Met?
Once the deductible is fully met:
Insurance starts paying for covered services
Patient pays:
Coinsurance or copay only
Example:
Deductible met
Bill: $1,000
Coinsurance: 20%
You pay $200, insurance pays $800
Important Actions for Billing Professionals
If you work in healthcare billing, here are key steps to follow:
After Receiving EOB:
Update patient account
Send EOB for posting
If Claim Sent for Reprocessing:
Track TAT
Set follow-up reminders
Billing to Secondary Insurance:
Before rebilling:
Verify patient eligibility
Check active coverage on Date of Service (DOS)
If Secondary Insurance Exists:
Submit claim to secondary payer
If No Secondary Insurance:
Bill patient directly
Special Case: Medicare Claims
When dealing with Medicare:
Medicare often forwards claims to secondary payers automatically
If no response after 30 days:
Follow up with insurance
Out-of-Network Considerations
If a claim is processed as out-of-network:
Full amount may become patient responsibility
You can:
Bill secondary payer (if available)
Otherwise, bill patient directly
Key Tips to Remember
Always track how much deductible is met
Request EOB for accurate details
Verify eligibility before rebilling
Monitor reprocessing timelines
Don’t assume insurance will pay until deductible is met
Frequently Asked Questions (FAQs)
1. What happens if I never meet my deductible?
You will continue to pay for covered services out of pocket, and insurance may not contribute (except for preventive services in some plans).
2. Does deductible apply to all medical services?
Not always. Some services like preventive care may be covered without requiring you to meet the deductible.
3. Is deductible the same as out-of-pocket maximum?
No.
Deductible: Amount you pay before insurance starts
Out-of-pocket maximum: The total limit you pay in a year
4. Can I have multiple deductibles?
Yes. Some plans have:
Individual deductible
Family deductible
Separate deductibles for services (e.g., prescriptions)
5. What is an EOB and why is it important?
An Explanation of Benefits (EOB) shows:
What was billed
What insurance paid
What you owe
It’s essential for tracking deductible and payments.
Conclusion:
Understanding the deductible amount is crucial for managing both your healthcare expenses and insurance claims effectively. It determines how much you need to pay upfront and influences how your insurance benefits are applied. Whether you’re a patient trying to control costs or a billing professional handling claims, knowing how deductibles work helps you make informed decisions, avoid billing errors, and ensure accurate claim processing. Take time to review your insurance policy, track your deductible progress, and always verify details when dealing with claims—this knowledge can save you both time and money.