In medical billing and revenue cycle management, denial codes can often be confusing—especially for beginners. One such commonly encountered denial is CARC 151, which states: “Payment adjusted because the payer deems the information submitted does not support this many/frequency of services.”
In simpler terms, this denial means that the insurance company believes the number of times a service was billed—or how often it was performed—is not justified based on their guidelines.
Understanding how to analyze and resolve CARC 151 denials is essential for reducing revenue loss and improving claim acceptance rates. This guide breaks down the concept in an easy-to-understand way and provides practical steps to handle it effectively.
What is CARC 151 Denial?
CARC 151 occurs when a payer limits how often a particular CPT (Current Procedural Terminology) code can be billed within a specific timeframe.
Common Reasons for CARC 151:
The service exceeds the allowed frequency (e.g., once per day)
Duplicate billing of the same CPT code
Lack of documentation supporting repeated services
Services billed more often than payer policy allows
Example:
If a CPT code is allowed once per day, but it is billed twice on the same day, the second charge may be denied under CARC 151.
Step-by-Step Process to Handle CARC 151
Handling this denial requires a structured approach. Here’s how you can investigate it effectively:
- Confirm the Denial Date
Start by identifying when the claim was denied. This helps determine deadlines for appeals or corrections. - Check the CPT Reimbursement Guidelines
Contact the payer or refer to their policy to understand:
How many times the CPT code is allowed
Whether it’s limited per day, per visit, or per time period
Example Questions to Ask:
Is this CPT allowed once per day or multiple times?
Are there any modifiers required for multiple services?
- Verify Billing History in Your System
Now check your internal billing system:
Was the same CPT already billed on the same date?
Was it billed by another provider in the same facility? - Determine if the Denial is Correct or Incorrect
✔ Denial is Correct:
CPT was already billed within the allowed timeframe
Frequency exceeds payer policy
✘ Denial is Incorrect:
CPT was not billed previously
No duplicate or excess frequency found
What to Do if the Denial is Correct
If the payer’s decision is accurate, follow these steps:
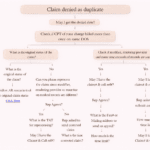
- Check Timely Filing for Corrections
Ask the payer: “What is the time limit to send a corrected claim?” - Gather Appeal Details
Obtain:
Fax number or mailing address
Appeal submission deadline - Decide Next Action
Depending on your organization’s policy:
Submit an appeal with justification
Or write off the claim if not recoverable - Document the Call
Always record:
Claim number
Call reference number
Details provided by the payer
What to Do if the Denial is Incorrect
If you believe the denial is wrong, take corrective action:
- Request Reprocessing
Ask the payer:
“Could you please reprocess the claim since the CPT has not met the maximum allowance?” - Confirm Turnaround Time (TAT)
Ask how long reprocessing will take - Record Important Details
Claim number
Call reference number
Expected resolution date
Special Scenario: CPT Not Found in Your System
Sometimes, you may not find the CPT in your records, but the payer insists it was already billed.
Possible Reasons:
The charge was not posted in your system
Another provider from the same facility billed it
What You Should Do:
Ask the payer for:
Date of service
Billing provider name
Document this information in your notes
Treat the denial as correct
Key Tips to Prevent CARC 151 Denials
Reducing denials is always better than fixing them. Here are some practical tips:
✔ Understand Payer Policies
Maintain a reference list of CPT frequency limits for major payers
✔ Use Billing Edits
Implement system alerts for duplicate or excessive billing
✔ Ensure Proper Documentation
Clearly justify repeated services in medical records
✔ Use Modifiers Correctly
Some services require modifiers to indicate distinct procedures
✔ Regular Audits
Conduct periodic checks to identify recurring issues
Real-Life Example
Let’s say a provider bills CPT code X-ray imaging twice on the same day.
Payer guideline: Allowed once per day
System check: CPT billed twice
Result:
First claim → Paid
Second claim → Denied (CARC 151)
If no valid modifier or justification is present, the denial is correct.
Frequently Asked Questions (FAQs)
- What does CARC 151 mean in simple terms?
It means the insurance company thinks the service was billed too many times or too frequently. - Can CARC 151 denials be appealed?
Yes, if you have proper documentation proving the service was medically necessary and correctly billed. - How do I know if the denial is correct?
Compare payer guidelines with your billing records to see if the frequency limit was exceeded. - What if the payer says the CPT was already billed but I can’t find it?
Request details from the payer. It may have been billed by another provider or not posted in your system. - How can I avoid CARC 151 denials?
By understanding payer rules, using billing edits, and ensuring accurate documentation and coding.
Conclusion:
CARC 151 is a common denial in medical billing that revolves around frequency limitations of services. While it may seem complex at first, a systematic approach—checking guidelines, verifying billing history, and confirming payer policies—can help you quickly determine whether the denial is valid.
By strengthening internal processes, maintaining accurate records, and staying informed about payer rules, healthcare organizations can significantly reduce these denials and improve revenue cycle efficiency.
Mastering CARC 151 not only helps in faster claim resolution but also builds a strong foundation for handling other denial codes with confidence.








