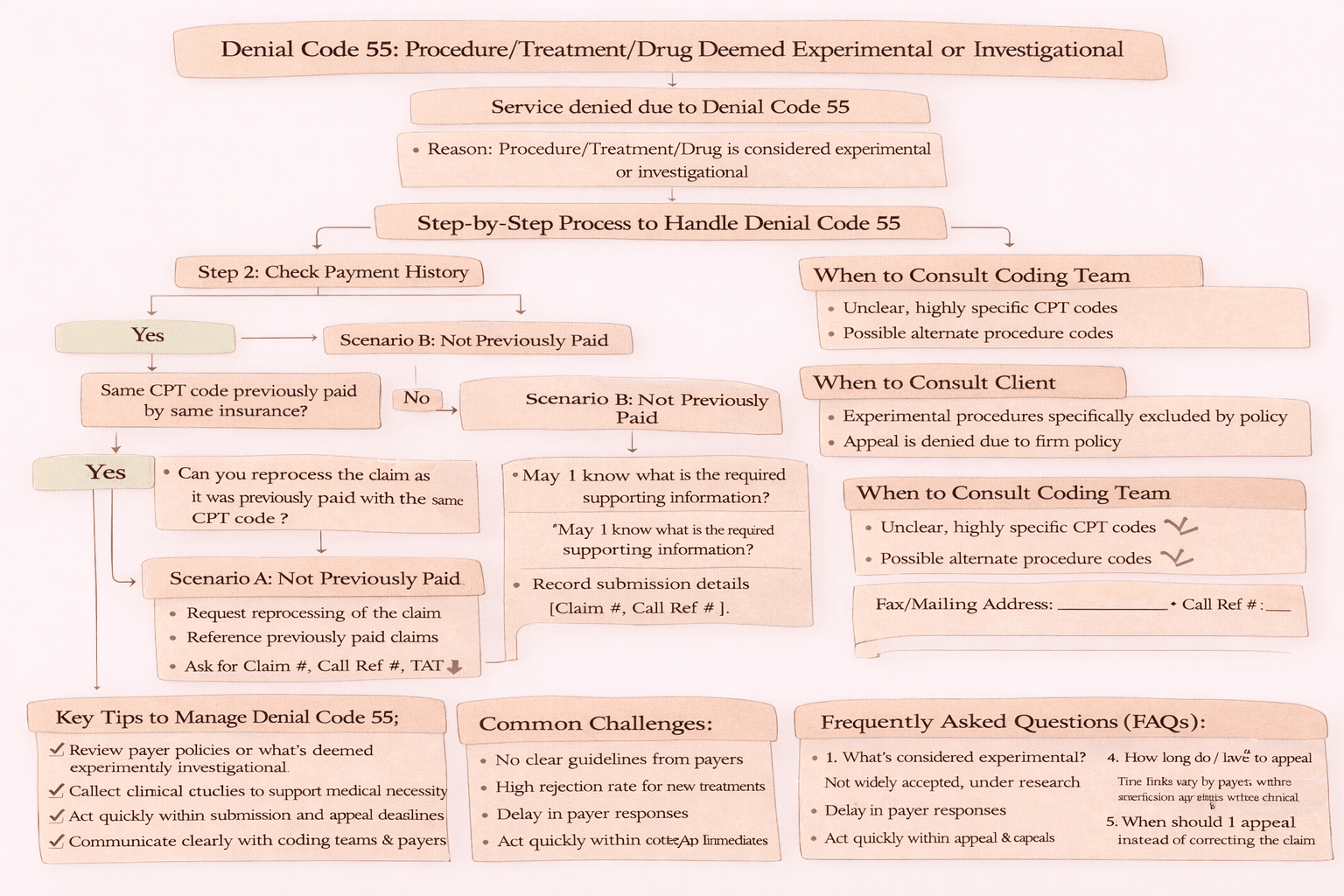
In medical billing and revenue cycle management, denial codes are a common challenge. One of the more complex denials to handle is Denial Code 55, which indicates that a procedure, treatment, or drug is considered experimental or investigational by the payer.
This type of denial can be frustrating because it often involves clinical judgment, payer policies, and coding accuracy. Understanding how to identify, analyze, and respond to this denial is crucial for maximizing reimbursements and minimizing revenue loss.
What Does Denial Code 55 Mean?
Denial Code 55 occurs when an insurance company determines that a billed service is:
Not widely accepted as standard medical practice
Considered experimental or under research
Not proven effective based on their guidelines
Simple Example
A provider performs a newly developed treatment that is still under clinical trials. Even if medically necessary, the insurance payer may deny the claim because it is not yet approved under their policy.
Step-by-Step Workflow to Handle Denial Code 55
1. Verify Denial Details
Start by confirming the denial reason, date of denial, and payer-specific policy.
2. Check Payment History
Ask whether the same CPT code has been paid previously by the same insurance.
If yes:
Request reprocessing of the claim
Provide reference of previously paid claims
Ask for turnaround time, claim number, and call reference number
If no:
Move to the next step
3. Ask for Additional Requirements
Contact the payer and check if they require supporting documents such as clinical notes, medical necessity documentation, or research or approval details.
If documents are required:
Ask what documents are needed and the submission deadline
Submit within the time limit
Record claim number and call reference number
4. Appeal the Denial
If no documents are requested or the denial continues, proceed with an appeal.
Ask for fax number or mailing address and appeal timeline
Submit a strong appeal including medical necessity justification, supporting clinical evidence, and provider notes
Role of CPT Codes in Denial Code 55
CPT codes play a major role in this denial.
Key Insight
Certain CPT codes may be flagged by payers as experimental, non covered, or under review.
What You Should Do
Send the case to the coding team and request alternate CPT codes if applicable.
If an alternate CPT is available:
Update and resubmit the claim
If no alternate CPT is available:
Proceed with appeal or follow payer guidance
When to Escalate to Coding or Client
Denial Code 55 often requires collaboration.
Escalate to coding team when the CPT code is unclear or alternative coding options may exist.
Inform the client when the CPT is consistently denied or payer policy clearly excludes the procedure.
The client may decide to write off the charge or avoid future billing for that CPT.
Key Tips to Handle Denial Code 55 Effectively
Always verify payer policy before billing new or uncommon procedures
Maintain proper documentation for medical necessity
Track previously paid claims for similar CPT codes
Act quickly within appeal and submission timelines
Communicate clearly with payers, coding teams, and clients
Common Challenges
Lack of clear payer guidelines
Delays in appeal processing
No alternate CPT available
High rejection rate for experimental procedures
FAQs
1. What is considered an experimental procedure?
A procedure is considered experimental if it is not widely accepted, lacks sufficient clinical evidence, or is still under research or trials.
2. Can Denial Code 55 be overturned?
Yes, depending on strong medical documentation, payer policies, and supporting evidence.
3. What documents help in appeals?
Physician notes, clinical studies, approval details, and medical necessity letters.
4. What if no alternate CPT code is available?
Follow payer instructions, submit documentation, file an appeal, or consider write off if advised.
5. How long do I have to appeal?
Appeal timelines vary by payer but usually range from 30 to 180 days. Always confirm with the insurance company.
Conclusion
Denial Code 55 is one of the more complex denials in medical billing because it involves both clinical and administrative factors. Successfully managing this denial requires careful review of payer policies, collaboration with coding teams, and strong documentation.
In some cases, reimbursement may not be possible. However, by following a structured approach and maintaining clear communication, you can improve your chances of resolving the denial or making informed decisions such as resubmission or write off.
Understanding this denial helps improve claim success rates and strengthens overall revenue cycle management.