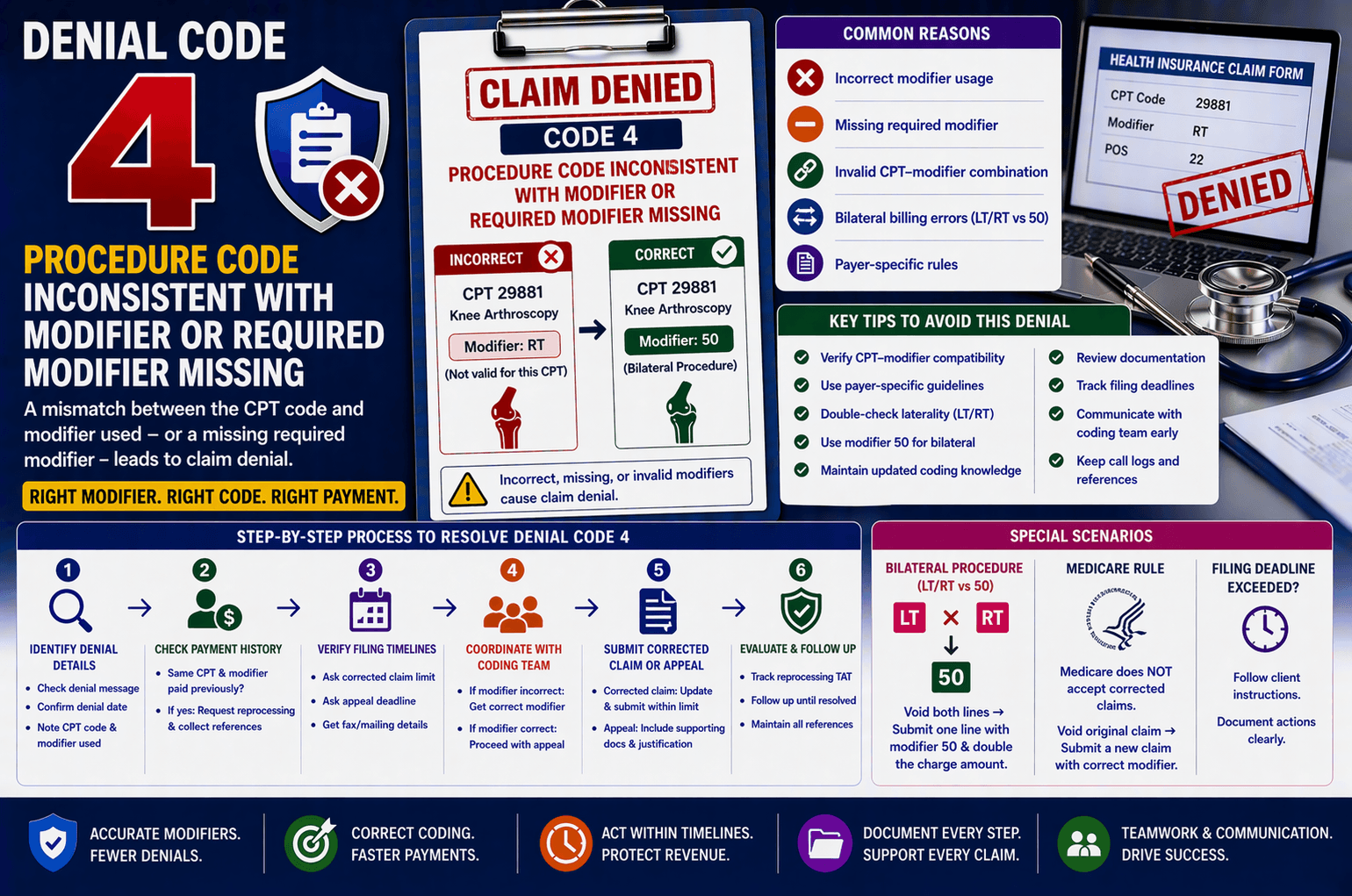
In medical billing, claim denials are a routine challenge—but understanding why they occur is the key to faster resolution and improved revenue cycle performance. One common denial reason is: “Procedure code inconsistent with the modifier used or a required modifier is missing.” This denial indicates a mismatch between the CPT (Current Procedural Terminology) code and the modifier applied—or the absence of a necessary modifier altogether. In this guide, we’ll break down this denial in simple terms, walk through real-world scenarios, and provide a clear step-by-step approach to resolving it efficiently.
What Does This Denial Mean?
A modifier is a two-character code added to a CPT code to provide additional information about the procedure performed. When a claim is denied for inconsistency between the procedure code and modifier, it typically means:
The modifier used is invalid for that CPT code
The modifier is incorrectly applied
A required modifier is missing
The combination violates payer-specific rules
Common Reasons for This Denial
Understanding the root cause helps resolve the issue quickly. Here are the most frequent reasons:
1. Incorrect Modifier Usage
Example: Using modifier RT (Right side) on a procedure that doesn’t support laterality
2. Missing Required Modifier
Some CPT codes require modifiers (e.g., professional vs technical components)
3. Invalid CPT-Modifier Combination
Certain modifiers are not allowed with specific CPT codes per payer guidelines
4. Bilateral Billing Errors
Using LT and RT separately when payer expects modifier 50 (Bilateral)
5. Payer-Specific Rules
Different insurance providers (especially Medicare) have unique billing rules.
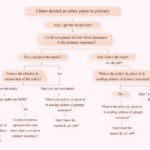
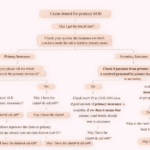
Step-by-Step Process to Handle This Denial
Here’s a structured workflow you can follow:
Step 1: Identify Denial Details
Check denial message
Confirm denial date
Note CPT code and modifier used
Step 2: Check Payment History
Ask:
Has the same CPT code with the same modifier been paid previously?
If YES:
Request reprocessing:
“Can you please reprocess the claim as payment was received for the same CPT and modifier?”
Ask for:
Turnaround time (TAT)
Claim reference number
Call reference number
If NO:
Proceed to next steps.
Step 3: Verify Filing Timelines
Ask:
What is the time limit to submit a corrected claim?
What is the appeal filing deadline?
This is critical because actions depend on whether timelines are still valid.
Step 4: Coordinate with Coding Team
Assign the claim to the coding team for review:
If modifier is incorrect:
Get the correct modifier
Submit a corrected claim
If modifier is correct:
Proceed with an appeal
Step 5: Submit Corrected Claim or Appeal
Corrected Claim:
Update with correct modifier
Submit within filing limit
Appeal:
Include:
Supporting documentation
Justification for modifier usage
Ensure submission within appeal timeframe.
Special Scenarios You Must Know
1. Bilateral Procedures (LT/RT vs Modifier 50)
Scenario:
CPT billed with LT and RT separately
One side paid, other denied
Solution:
Void both lines
Submit one line with modifier 50
Double the charge amount
2. Medicare-Specific Rule
Medicare does not accept corrected claims in the usual way.
Correct Process:
Void the original paid claim
Submit a new claim with correct modifier (e.g., modifier 50)
3. Timely Filing Exceptions
Sometimes:
Filing limit is crossed
Client still requests submission
In such cases:
Follow client instructions
Document actions clearly.
Key Tips for Avoiding This Denial
Always verify CPT-modifier compatibility
Use payer-specific guidelines
Double-check laterality modifiers (LT/RT)
Understand when to use modifier 50
Maintain updated coding knowledge
Track filing deadlines carefully
Communicate with coding team promptly.
Example Scenario
Situation:
CPT: 29881 (Knee arthroscopy)
Modifier used: RT
Denied for inconsistency
Resolution:
Check if bilateral procedure was done
If yes:
Replace RT/LT with modifier 50
Submit corrected claim
If modifier is valid:
Appeal with documentation.
FAQs
1. What is a modifier in medical billing?
A modifier provides additional information about a procedure, such as location, extent, or circumstances under which it was performed.
2. How do I know which modifier to use?
Refer to:
CPT guidelines
Payer-specific policies
Coding team recommendations
3. Can I resubmit a corrected claim after the deadline?
Generally no, but:
Some clients may still request submission
Always verify payer rules before proceeding
4. What should I do if the modifier is correct but claim is denied?
Submit an appeal with:
Medical records
Explanation of modifier usage
5. Why does Medicare handle corrected claims differently?
Medicare requires:
Voiding the original claim
Submitting a new claim instead of a corrected one
Conclusion:
Denials due to procedure code and modifier inconsistencies can be frustrating, but they are manageable with a structured approach. The key lies in:
Understanding modifier rules
Verifying payer-specific requirements
Collaborating with coding teams
Acting within filing deadlines
By following the workflow outlined in this guide, you can reduce denials, improve claim acceptance rates, and ensure a smoother revenue cycle process. Staying proactive and detail-oriented is what separates average billing operations from high-performing ones.