In medical billing and revenue cycle management, denial codes can significantly impact cash flow if not handled correctly. One common denial is “Patient Cannot Be Identified” (Denial Code 31). This occurs when the insurance payer cannot match the submitted claim with a valid patient record in their system.
For beginners in healthcare billing, this denial may seem confusing, but it is usually caused by simple data errors. This guide explains the reasons behind this denial, how to resolve it efficiently, and best practices to prevent it in the future.
What Does “Patient Cannot Be Identified” Mean?
This denial indicates that the insurance company is unable to locate the patient based on the information submitted in the claim.
Common Causes:
Incorrect patient name
Wrong date of birth (DOB)
Invalid or missing policy ID
Incorrect gender
Data entry errors or formatting issues
Even a minor mismatch (like spelling errors or swapped first/last names) can trigger this denial.
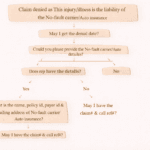
Step-by-Step Process to Handle This Denial
Handling this denial requires a structured approach. Below is a simplified workflow used in Accounts Receivable (AR) follow-ups:
- Verify Patient Information
Start by confirming:
Full name (as per insurance card)
Date of birth
Gender
Social Security Number (if applicable)
Ask the payer representative to search using these details.
- If Patient Is Found
If the payer successfully locates the patient:
Next Steps:
Request the correct policy ID
Verify if the claim exists for the Date of Service (DOS)
Scenario A: Claim Exists
Follow standard AR procedures based on claim status (paid, denied, pending)
Scenario B: Claim Not Found
Check:
Policy effective date
Policy termination date
- Check Policy Eligibility
Confirm whether the Date of Service falls within the policy period:
If DOS is within active coverage:
Check Timely Filing Limit (TFL)
If DOS is outside coverage:
Request a call reference number
Consider billing the patient if no other insurance is active
- Evaluate Timely Filing Limit (TFL)
Timely filing is crucial in claim submission.
If DOS is within TFL:
Ask for:
Payer ID
Mailing address
Fax number
Resubmit the claim
If DOS is outside TFL:
Ask:
Can the claim be faxed or mailed with Proof of Timely Filing (POTF)?
- Based on Payer Response
If POTF is Accepted:
Send claim via fax/mail with documentation
If POTF is Not Accepted:
Resubmit claim
Wait for TFL denial
File an appeal with POTF
If No POTF Available:
Claim may need to be written off
Special Cases and Important Notes
- When Patient Cannot Be Found at All
If the payer cannot identify the patient:
Request a call reference number
Verify details via payer portal
If no active insurance exists → Bill the patient - Medicare-Specific Guidelines
Ensure:
Correct MBI (Medicare Beneficiary Identifier)
Accurate name and DOB
Tip:
Try variations like:
Swapped first/last name
Adding suffixes (Jr, Sr, II, III)
- BCBS (Blue Cross Blue Shield) Cases
Requires a 3-character alpha prefix
Missing prefix = automatic denial
Example:
Prefix varies by state
Sometimes can be derived using SSN via payer portals (like Availity)
- Secondary Insurance Billing Rule
Never bill secondary insurance if primary denied for identification issues.
Reason:
Secondary payer will also deny the claim.
Best Practices to Prevent This Denial
Prevention is always better than rework. Here are key tips:
Verify Patient Details at Registration
Match with insurance card exactly
Avoid abbreviations unless required
Double-Check Data Entry
Ensure no typos in:
Name
DOB
Policy ID
Use Insurance Portals
Validate eligibility before claim submission
Maintain Updated Records
Track changes in:
Policy numbers
Coverage periods
Train Staff Regularly
Educate front desk and billing teams about common errors
Real-Life Example
Scenario:
A claim is denied because the patient cannot be identified.
Issue Found:
The last name was entered incorrectly (missing one letter).
Resolution:
Corrected the spelling
Resubmitted the claim within TFL
Claim processed successfully
Small errors can lead to big delays—accuracy matters.
Frequently Asked Questions (FAQs)
- What is Denial Code 31?
It means the insurance company cannot identify the patient based on submitted details. - Can a small spelling mistake cause this denial?
Yes. Even minor errors in name or DOB can result in rejection. - What should I do first after receiving this denial?
Verify patient demographics and request the payer to search using correct details. - Can I resubmit the claim after correction?
Yes, if it is within the Timely Filing Limit. - What if the claim is past TFL?
You may:
Submit with Proof of Timely Filing
Appeal after denial
Or write off if no documentation exists
Conclusion:
The “Patient Cannot Be Identified” denial is one of the most common yet avoidable issues in medical billing. It typically arises from simple data mismatches but can lead to significant delays if not handled properly.
By following a structured workflow—verifying patient details, checking eligibility, and understanding payer-specific rules—you can resolve this denial efficiently. More importantly, implementing strong front-end verification processes can help prevent it altogether.
Accuracy, attention to detail, and timely follow-ups are the keys to minimizing denials and maintaining a healthy revenue cycle.