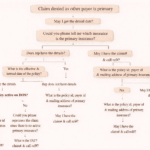
In medical billing and insurance processing, denial codes are a common part of the workflow. One such frequently encountered denial is Code 242, which indicates that services were provided by an out-of-network provider and are not covered under the patient’s insurance plan.
Understanding this denial is critical for billing professionals, revenue cycle teams, and healthcare providers. If handled correctly, it can either lead to claim reprocessing or appropriate billing to the patient or secondary payer.
This guide breaks down Denial Code 242 in simple terms, explains when it occurs, and provides actionable steps to resolve it effectively.
What Is Denial Code 242?
Denial Code 242 is issued when:
The provider is not contracted (out-of-network) with the insurance payer.
The patient’s insurance plan does not include out-of-network benefits, or the payer processes it as non-covered.
In Simple Terms:
If a patient receives care from a provider outside their insurance network, the claim may be denied unless their plan allows such services.
Why Does This Denial Occur?
There are a few key reasons behind this denial:

- Provider Is Out of Network
The healthcare provider is not part of the insurance company’s approved network. - Patient Plan Restrictions
Some plans do not cover out-of-network services at all. - Plan Type Limitations
Coverage depends heavily on the type of insurance plan:
HMO (Health Maintenance Organization) → No out-of-network coverage
EPO (Exclusive Provider Organization) → No out-of-network coverage
PPO (Preferred Provider Organization) → Covers out-of-network
POS (Point of Service) → Covers out-of-network
Understanding Insurance Plan Types
Knowing the patient’s plan is essential to resolve Denial 242 correctly.
HMO Plans
Strict network rules
No coverage outside the network
Requires referrals for specialists
EPO Plans
Similar to HMO
No out-of-network benefits
PPO Plans
Flexible provider choice
Covers both in-network and out-of-network services
Higher cost for out-of-network
POS Plans
Hybrid model
Allows out-of-network coverage with referrals
Step-by-Step Workflow to Handle Denial 242
Here’s a structured approach to manage this denial efficiently:
Step 1: Review the Denial
Confirm denial reason: “Non-covered services – provider out of network”
Note the denial date
Step 2: Verify Patient Plan
Ask:
Does the plan include out-of-network benefits?
What is the plan type (HMO, PPO, EPO, POS)?
Step 3: Take Action Based on Plan Type
If PPO or POS:
Contact payer and request:
Claim reprocessing
Ask:
“Since the patient has out-of-network benefits, can you reprocess the claim?”
Record:
Call reference number
Claim number
TAT (Turnaround Time)
If HMO or EPO:
Out-of-network services are not covered
Proceed with:
Billing to secondary insurance (if available)
Or patient responsibility
On-Call Scenario (Practical Approach)
When calling the insurance representative, follow this flow:
Confirm denial reason
Ask for denial date
Verify out-of-network coverage
Identify plan type
Take appropriate action:
For PPO/POS:
Request reprocessing
Ask for TAT
Document call details
For HMO/EPO:
Collect claim and reference details
Move claim to next billing step
Key Actions to Take
If Claim Can Be Reprocessed:
Follow up within the TAT provided
Track claim status regularly
If Claim Cannot Be Reprocessed:
Check for secondary or consecutive payer
Verify eligibility before billing
If No Other Coverage:
Release claim to patient billing
Important Tips for Billing Teams
Always verify eligibility before submission
Prevents unnecessary denials
Check provider network status in advance
Avoids out-of-network surprises
Document every call with payer
Helps during audits or escalations
Understand plan types thoroughly
Reduces errors in claim handling
Set timely follow-ups
Ensures faster revenue recovery
Example Scenario
Case:
A patient with a PPO plan receives treatment from an out-of-network provider.
Outcome:
Claim initially denied (Code 242)
Billing team contacts payer
Confirms PPO includes out-of-network benefits
Requests reprocessing
Claim gets approved after review
FAQs
- What does Denial Code 242 mean?
It means the service was provided by an out-of-network provider and is not covered under the patient’s plan. - Can Denial 242 be overturned?
Yes, if the patient has PPO or POS coverage, the claim can often be reprocessed. - What should be done for HMO or EPO plans?
Since they don’t cover out-of-network services:
Bill secondary insurance (if available)
Otherwise, bill the patient - Why is eligibility verification important?
It helps confirm:
Plan type
Coverage details
Prevents avoidable denials - What is TAT in claim reprocessing?
TAT (Turnaround Time) is the time the payer takes to reprocess the claim after request.
Conclusion:
Denial Code 242 is a common but manageable issue in medical billing. The key to resolving it lies in understanding insurance plan types, verifying out-of-network benefits, and following a structured workflow.
For PPO and POS plans, reprocessing is often possible, while HMO and EPO plans require shifting responsibility to secondary payers or patients. By applying the right steps and maintaining proper documentation, billing teams can minimize revenue loss and improve claim success rates.
A proactive approach—especially eligibility verification and network checks—can significantly reduce the occurrence of this denial in the first place.