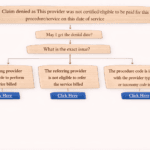
In medical billing, claim denials are a common challenge—but each denial comes with a reason code that helps identify the issue. One such denial is M119, which indicates a problem with the National Drug Code (NDC) on a claim.
If you’ve encountered an M119 denial, don’t worry. This guide will walk you through what it means, why it happens, and how to resolve it efficiently. Whether you’re new to medical billing or looking to sharpen your skills, this article breaks everything down in simple, practical terms.
What is an NDC Code?
The National Drug Code (NDC) is a unique identifier assigned to medications in the United States. It is used to specify:
The drug manufacturer
The specific drug
The packaging
Why NDC Codes Matter
NDC codes are required when billing for drug-related CPT/HCPCS codes, especially those that start with a letter like:
J0256
J2425
J7649
Without a valid NDC code, insurance payers cannot process the drug portion of the claim accurately.
What Does M119 Denial Mean?
M119: Missing, incomplete, invalid, deactivated, or withdrawn NDC code
This denial occurs when:
The NDC code is missing
The NDC format is incorrect
The code is invalid or outdated
Required NDC details are incomplete
In simple terms, the payer is saying:
“We cannot process this drug claim because the NDC information is incorrect or insufficient.”
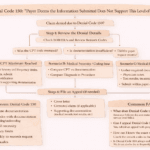
Where to Find the NDC Code on Claim Forms
Understanding where NDC codes should appear is essential.
CMS-1500 Form
Found in the shaded area of fields 24A–24G
Must include:
NDC Qualifier (e.g., N4)
NDC Code
Unit of Measure
Number of Units
UB-04 Form
Located in Field 43
Same formatting requirements apply
Correct NDC Format Explained
A properly formatted NDC entry includes:
Qualifier: Usually “N4”
NDC Code: 11-digit code (no dashes)
Unit of Measure:
F2 (International Unit)
GR (Gram)
ML (Milliliter)
UN (Unit)
Quantity: Number of units administered
Example
N412345678901ML2
This means:
N4 = Qualifier
12345678901 = NDC code
ML = Milliliters
2 = Quantity
Step-by-Step Process to Resolve M119 Denial
Here’s a practical workflow you can follow when handling this denial:
- Verify the Denial Details
Check the denial date
Review the claim form and system records
Confirm whether an NDC code was submitted - Check If NDC Code Exists
If NDC is Present:
Confirm with the payer:
“We billed the claim with an NDC code. Can you verify if it is correct?”
Outcomes:
Correct: Request reprocessing
Incorrect: Ask for the correct NDC
If NDC is Missing:
Request the correct NDC code from the payer or provider
- If Payer Provides Correct NDC
Update the claim in:
Billing software OR
Clearinghouse
Resubmit the corrected claim - If Payer Does NOT Provide NDC
Search reliable sources (drug databases or official references)
Verify the code with the payer before submitting - Confirm Additional Required Details
Even with a correct NDC code, you still need:
Unit of Measure
Number of Units
Without these, the claim may still be rejected. - Ask Key Follow-Up Questions
What is the timely filing limit for corrected claims?
Can you provide the claim number and call reference number?
Common Causes of M119 Denial
Understanding root causes helps prevent future issues:
Missing NDC code
Incorrect format (not 11 digits)
Missing qualifier (N4)
Invalid or expired NDC
Missing units or measurement type
Typographical errors
Important Tips for Avoiding M119 Denials
Always Validate NDC Codes
Before submitting claims, double-check:
Accuracy
Format
Units
Use Updated Drug Databases
Ensure you are using current and active NDC codes.
Train Staff Regularly
Billing teams should understand:
When NDC is required
How to format it correctly
Document Everything
Keep records of:
Calls with payers
Reference numbers
Corrections made
Coordinate with Clients
If you cannot update claims:
Escalate to the client
Follow client-specific workflows
What If You Cannot Find the Correct NDC?
If you’re stuck:
Assign the task to the client
Contact the appropriate department (pharmacy/billing specialist)
Follow internal escalation procedures
Never guess or submit incomplete information—it can lead to repeated denials.
Frequently Asked Questions (FAQs)
- Is NDC required for all CPT codes?
No. NDC is required only for drug-related CPT/HCPCS codes, usually starting with “J”. - What happens if I submit an incorrect NDC code?
The claim will likely be denied with code M119 or similar errors. - Can I resubmit a corrected claim?
Yes. Once corrected, you can resubmit within the timely filing limit. - What if I don’t have NDC units or measurement?
You must obtain them before resubmission. Without these, the claim remains incomplete. - Who can provide the correct NDC code?
Insurance representative
Healthcare provider
Drug reference databases
Conclusion:
The M119 denial may seem complex at first, but it becomes manageable once you understand the role of NDC codes in medical billing. Most issues stem from missing or incorrectly formatted information—problems that are entirely preventable with proper checks.
By following a structured approach—verifying details, correcting errors, and ensuring complete NDC data—you can resolve these denials efficiently and reduce their occurrence in the future.
Mastering NDC handling not only improves claim acceptance rates but also strengthens your overall billing accuracy.