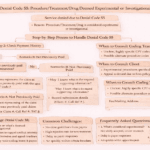
In medical billing, claim denials are a common challenge—but understanding them is key to resolving issues efficiently. One such denial is Code 119: Benefit Maximum for This Time Period or Occurrence Has Been Reached.
If you’re new to healthcare billing or revenue cycle management, this denial can seem confusing. However, it simply means that the insurance company has already paid the maximum benefit allowed under the patient’s policy.
In this guide, we’ll break down what Denial Code 119 means, why it happens, how to handle it, and what steps you should take next—all in clear, simple terms.
What is Denial Code 119?
Denial Code 119 indicates that:
The insurance company will not pay the claim because the patient has already used up the maximum benefits allowed under their policy.
These limits can be based on:
Dollar amount (financial limit)
Number of visits (usage limit)
Once the limit is reached, any additional services are not covered.
Why Does This Denial Occur?
Insurance policies often include benefit caps to control costs. These caps can apply annually or over a lifetime.
Common Reasons:
The patient exceeded the annual dollar limit
The patient used up the maximum number of visits
The service falls under a restricted benefit category (e.g., therapy, chiropractic care)
Types of Benefit Limits
- Dollar-Based Limit
This is when insurance covers services only up to a specific monetary amount.
Example:
Annual coverage limit: ₹80,000 ($1,000 approx.)
Patient already received services worth ₹80,000
New claim: Denied because limit is reached
- Visit-Based Limit
This is when insurance allows only a certain number of visits.
Example:
Allowed visits: 5 per year
Patient already completed 5 visits
6th visit: Denied due to limit exhaustion
How to Handle Denial Code 119 (Step-by-Step)
When you encounter this denial, follow a structured approach:
Step 1: Verify Denial Details
Ask:
What is the denial date?
Is the limit based on dollar amount or visits?
Step 2: Check Benefit Limits
If Dollar-Based:
What is the maximum allowed amount?
How much has the patient already used?
If Visit-Based:
How many visits are allowed?
How many visits has the patient already completed?
Step 3: Evaluate the Situation
Scenario A: Limit Already Met
If the patient has already reached the limit (excluding current claim):
The denial is valid
Move to next steps (secondary billing or patient billing)
Scenario B: Limit NOT Met
If the patient has not reached the limit:
Request reprocessing of the claim
Ask for:
Claim number
Call reference number
Turnaround time (TAT)
What to Do After Confirmation
If Benefit is Exhausted
You have two main options:
- Bill Secondary Insurance
Check if patient has secondary or consecutive insurance
Verify eligibility on the Date of Service (DOS)
Submit claim correctly (do NOT change payer sequence)
- Bill the Patient
If no secondary insurance exists:
Transfer responsibility to the patient
Send statement or invoice
If Benefit is NOT Exhausted
Request payer to reprocess the claim
Document:
Representative details
Call reference number
TAT (Turnaround Time)
Set a follow-up reminder
Important Tips for Handling Denial 119
Always verify benefit usage before resubmitting claims
Never assume the denial is correct—double-check limits
Maintain proper documentation of calls and references
Confirm secondary insurance eligibility before billing
Do not change payer sequence when billing secondary insurance
Track reprocessing timelines carefully
Real-Life Example
Let’s simplify with a scenario:
Patient Policy:
Covers physiotherapy
Limit: 10 visits per year
Situation:
Patient already completed 10 sessions
Visits for 11th session
Claim submitted → Denied (Code 119)
Action:
Verify visit count → Confirm 10 used
No secondary insurance → Bill patient
Common Mistakes to Avoid
Ignoring benefit verification before claim submission
Billing secondary insurance as primary
Not checking if denial is incorrect
Missing follow-ups on reprocessed claims
Failing to document payer communication
Frequently Asked Questions (FAQs)
- Can Denial Code 119 be appealed?
Yes, but only if the denial is incorrect. If the patient hasn’t actually reached the benefit limit, you can request reprocessing or file an appeal. - Who is responsible for payment after this denial?
If benefits are exhausted:
Secondary insurance (if available)
Otherwise, the patient is responsible
- How can I prevent this denial?
Verify benefits before treatment
Track patient usage (visits or dollar limits)
Communicate limits to patients in advance
- What is TAT in reprocessing?
TAT stands for Turnaround Time—the number of days the insurance company takes to reprocess a claim. - Should I always send denied claims to secondary insurance?
Only if:
Secondary insurance is active on the Date of Service
The claim is eligible under that plan
Conclusion:
Denial Code 119 is straightforward once you understand it: it simply means the patient has used up their insurance benefits for a specific service.
The key to managing this denial effectively lies in:
Verifying benefit limits
Identifying whether the denial is valid
Taking appropriate next steps (reprocessing, secondary billing, or patient billing)
By following a structured workflow and maintaining accurate records, you can reduce errors, improve claim success rates, and ensure smoother revenue cycle management.
Mastering denials like Code 119 is an essential skill in medical billing—and with practice, it becomes second nature.