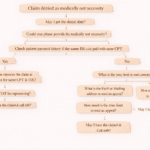
In medical billing, denial codes can be confusing—especially for beginners. One of the most common yet misunderstood codes is Denial Code 23, which refers to “the impact of prior payer(s) adjudication including payments and/or adjustments.”
Simply put, this denial happens when the primary insurance has already paid enough—or more than what the secondary insurance allows. As a result, the secondary payer either pays a reduced amount or denies the remaining balance altogether.
Understanding this denial is critical for revenue cycle management professionals, as it directly impacts reimbursement and write-offs. This guide breaks down Denial 23 in a clear, beginner-friendly way with practical examples and actionable tips.
What Is Denial Code 23?
Denial Code 23 occurs during coordination of benefits (COB) when:
A patient has more than one insurance plan
The primary insurance processes the claim first
The secondary insurance reviews what the primary has already paid
If the primary payment is equal to or greater than the secondary allowable amount, the secondary payer will:
Pay nothing, or
Pay only a small remaining balance
This leads to a denial or partial denial under Code 23.
How Coordination of Benefits Works
Before diving deeper, let’s understand the process:
Primary Insurance Pays First
The claim is processed, and payment is made based on their allowed amount.
Secondary Insurance Reviews the Claim
It considers:
What the primary paid
Its own allowed amount
Comparison Happens
If primary payment ≥ secondary allowed → denial or no payment
If primary payment < secondary allowed → partial payment
Real-Life Examples of Denial 23
Example 1: Full Secondary Payment
Billed Amount: $90
Primary Allowed: $20
Primary Paid: $16
Coinsurance (Patient Responsibility): $4
Secondary Allowed: $20
Since primary paid $16, the secondary pays the remaining $4.
Result: No denial—secondary covers the balance.
Example 2: Partial Denial
Billed Amount: $120
Primary Allowed: $30
Primary Paid: $24
Coinsurance: $6
Secondary Allowed: $28
Primary paid: $24
Secondary allowed: $28
Remaining payable: $4
The leftover $2 is denied under Code 23.
Result: Partial payment + partial denial.
Example 3: Full Denial
Billed Amount: $100
Primary Allowed: $25
Primary Paid: $20
Coinsurance: $5
Secondary Allowed: $20
Since primary already paid $20 (equal to secondary allowed):
Result: Entire remaining balance denied under Code 23.
Why Denial 23 Happens
Denial 23 is not an error—it’s usually contractual logic based on payer rules. Common causes include:
Secondary payer has lower allowable rates
Incorrect expectations of secondary coverage
Misinterpretation of coinsurance or patient responsibility
Lack of understanding of payer contracts
What to Do When You Receive Denial 23
Handling Denial 23 correctly can save time and prevent unnecessary appeals.
Step-by-Step Action Plan
- Verify Primary Payment
Check how much the primary insurance paid
Confirm allowed amount and adjustments - Compare with Secondary Allowed
Review secondary payer’s allowable amount - Make a Decision
If primary paid ≥ secondary allowed:
Write off the remaining balance
No further action needed
If primary paid < secondary allowed:
Contact secondary insurance
Request reprocessing if applicable
On-Call Scenario: How to Handle with Insurance
When calling insurance, follow a structured approach:
Ask for denial date
Confirm allowed amount
Verify primary payment details
Compare both values
Possible Outcomes:
If Primary Paid More or Equal
Document claim number and call reference
Proceed with write-off
If Primary Paid Less
Request claim reprocessing
Ask for Turnaround Time (TAT)
Set follow-up reminder
Key Tips to Avoid Denial 23 Issues
Always verify Coordination of Benefits (COB) details
Check both primary and secondary allowable amounts
Educate patients about coverage limitations
Maintain accurate billing and claim submission data
Avoid unnecessary appeals—this denial is often valid
Common Mistakes to Avoid
Appealing valid Denial 23 cases
Ignoring payer-specific allowable differences
Not reviewing Explanation of Benefits (EOB) carefully
Missing follow-ups when reprocessing is possible
Frequently Asked Questions (FAQs)
- Is Denial Code 23 always valid?
Yes, in most cases. It reflects payer coordination rules rather than billing errors. However, verification is still necessary. - Can Denial 23 be appealed?
Only if there is a processing error. If the denial is due to correct COB logic, appeals are usually not successful. - Who is responsible for the denied amount?
Typically, the provider writes off the amount, unless specified otherwise by payer contracts. - What if primary insurance paid incorrectly?
In that case:
Contact primary payer
Request correction
Then resubmit to secondary - How can I prevent Denial 23?
Ensure accurate COB information
Verify payer contracts
Review claims before submission
Conclusion:
Denial Code 23 may seem complex at first, but it becomes straightforward once you understand how primary and secondary insurance interact. The key takeaway is simple:
If the primary payer has already met or exceeded what the secondary allows, the remaining balance is not payable.
For billing professionals, the focus should be on verification, correct interpretation, and efficient handling rather than unnecessary appeals. By mastering this denial, you can improve claim resolution speed and maintain a healthy revenue cycle.
Understanding Denial 23 isn’t just about fixing claims—it’s about working smarter with payer systems.