In medical billing, claim denials are common—but some can be particularly confusing. One such denial is “This procedure is not paid separately.” This typically means that a billed CPT (Current Procedural Terminology) code is considered part of another primary procedure and therefore not reimbursed independently.
For beginners in medical billing or revenue cycle management (RCM), understanding how to handle this denial efficiently is crucial. This guide breaks down the process step by step, explains key concepts, and provides actionable tips to resolve such denials successfully.
What Does “Procedure Not Paid Separately” Mean?
When an insurance payer denies a claim stating that a procedure is not paid separately, it usually indicates:
The procedure is bundled with another primary service
Payment for the secondary procedure is included in the primary CPT code
The payer follows bundling rules such as NCCI (National Correct Coding Initiative) edits
Example:
If a minor procedure is performed along with a major surgery, the minor one may not be paid separately because it is considered part of the main procedure.
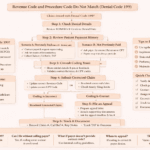
Step-by-Step Call Handling Process
When you encounter this denial, follow a structured approach during the insurance call.
- Confirm the Denial Details
Start by verifying:
Denial reason: Procedure not paid separately
Date of denial
Why this matters: Ensures you’re working with accurate and updated claim information. - Identify the Primary CPT Code
Ask the representative:
“May I know the primary CPT code associated with this claim?”
Possible Outcomes:
If the Primary CPT Code is Provided
Check Claim Submission:
Were both CPT codes billed on the same claim form?
If YES:
Request reprocessing:
“Can you please reprocess the claim as both CPTs were billed correctly?”
Ask:
Turnaround Time (TAT) for reprocessing
Claim number and call reference number
If NO:
Ask:
Time limit to send a corrected claim
Fax number or mailing address for submission
If the Primary CPT Code is NOT Provided
Ask:
Time limit to send an appeal
Appeal submission details (fax/mail)
Claim number and call reference number
What to Do After the Call
Scenario 1: Need Correct Primary CPT Code
If the representative cannot provide the correct primary CPT:
Assign the claim to the coding team
Request identification of:
Correct primary CPT
Whether bundling applies
Scenario 2: CPT Not Available in System
If the coding team identifies a valid CPT that is missing:
Create the CPT in your system
Resubmit the claim with:
Primary CPT
Secondary CPT (if applicable)
Scenario 3: CPT Can Be Billed Separately
Using tools like:
Encoder software
Coding reference platforms
You may find that the CPT should be paid separately.
In this case:
Call insurance and request reprocessing
If denied again → Submit an appeal with documentation
Understanding Bundling in Medical Billing
Bundling is a key concept behind this denial.
What is Bundling?
Bundling means combining multiple procedures into a single payment. Insurance companies do this to:
Prevent duplicate billing
Ensure cost control
Common Bundling Scenarios:
Surgical procedures + pre/post care
Diagnostic tests included in a larger procedure
Minor services performed alongside major ones
Tools to Identify Bundled CPT Codes
To verify whether a procedure is bundled, use:
Coding software (Encoder tools)
Medical coding databases
Payer-specific guidelines
NCCI edit tables
These tools help determine:
Whether two CPTs can be billed together
If modifiers (like -59) are required
Key Tips for Handling This Denial
Always verify the primary CPT code
Check if both CPTs were billed on the same claim
Use coding tools to confirm bundling rules
Document:
Call reference number
Representative name
Claim details
Know timely filing limits for:
Corrected claims
Appeals
Escalate to coding team when unsure
Common Mistakes to Avoid
Submitting appeals without verifying bundling rules
Missing deadlines for corrected claims
Not documenting payer communication
Assuming all denied CPTs are bundled (some are payable separately)
FAQs
- What does “not paid separately” mean in simple terms?
It means the procedure is included in another service and won’t be reimbursed on its own. - Can I still get paid for the denied CPT?
Yes, if:
It was billed incorrectly
It qualifies for separate payment with proper modifiers
The denial is incorrect and appealed successfully - What is a primary CPT code?
It’s the main procedure code that other services may be bundled into. - When should I send a corrected claim vs an appeal?
Corrected claim: When billing error exists
Appeal: When you believe the denial is incorrect - What if I don’t know the correct CPT code?
Assign the case to the coding team or use coding tools to identify it.
Conclusion:
Handling a “procedure not paid separately” denial requires a combination of coding knowledge, payer communication, and attention to detail. By following a structured workflow—verifying CPT codes, checking claim submissions, and leveraging coding tools—you can significantly improve your claim resolution success rate.
For beginners, mastering this denial type is a big step toward becoming proficient in medical billing. With practice and proper documentation, these scenarios become much easier to manage, ensuring faster reimbursements and fewer revenue losses.








