In medical billing, claim denials are common—but understanding why a claim is denied is critical to resolving it efficiently. One such denial scenario is when a claim is rejected because the injury or illness is work-related, making it the responsibility of the Worker’s Compensation (WC) carrier, not the regular health insurance payer.
This article breaks down the workflow, decision-making process, and best practices for handling such denials. Whether you’re new to medical billing or looking to sharpen your skills, this guide will help you navigate Worker’s Compensation cases with clarity and confidence.
What Does This Denial Mean?
When a payer denies a claim stating:
“This is a work-related injury/illness and thus the liability of the Worker’s Compensation Carrier”
…it indicates that the treatment provided is linked to a workplace incident. Therefore, the billing responsibility shifts from commercial or private insurance to the Worker’s Compensation insurance provider.
Step-by-Step Workflow to Handle the Denial
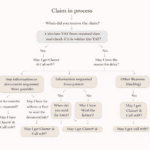
Handling this denial requires a structured approach. Below is a simplified workflow used in real-world billing scenarios.
- Confirm the Denial Date
Start by asking:
“May I get the denial date?”
This helps track timelines and ensures compliance with filing deadlines. - Request Worker’s Compensation Details
Next, gather essential information:
Name of the WC insurance company
Policy ID
Payer ID
Mailing address
Ask clearly:
“Could you please provide the worker compensation details?” - Check if the Representative Has the Details
This step determines your next move:
✔ If YES (Details Available)
Proceed to collect:
Claim number
Call reference number
Then:
Update the WC insurance as primary insurance
Resubmit the claim to the WC payer
✖ If NO (Details Not Available)
Ask:
“May I have the claim number and call reference number?”
Then move to internal verification steps (explained below).
What to Do If WC Details Are Missing
Sometimes, the insurance representative doesn’t have Worker’s Compensation information. In such cases:
Check Internal Systems
Look for:
Existing WC insurance records
Patient payment history
Any indication of WC as primary insurance
Verify Eligibility
If WC insurance is found:
Check eligibility status
Confirm coverage dates
Ensure claim aligns with the injury
Resubmit the Claim
If valid WC insurance exists:
Update it as primary insurance
Submit the claim to the WC payer
If No WC Insurance Is Found
If all checks fail:
Release the claim to the patient
Document all efforts made
Using Payer Portals for WC Information
Many payer portals provide additional insights. If you have access:
Search for WC-related claims
Look for accident-related notes
Retrieve missing insurance details
This step can save time and prevent unnecessary delays.
Coordination of Benefits (COB): Important Rules
Handling multiple insurances requires attention to hierarchy.
Key Guidelines:
Worker’s Compensation = Primary Insurance
Do NOT keep commercial insurance as secondary
Medicare CAN be secondary
When Medicare Is Secondary
If WC processes the claim but leaves a balance:
Update the MSP (Medicare Secondary Payer) code
Bill Medicare for the remaining amount
Common Mistakes to Avoid
Avoid these frequent errors:
Billing commercial insurance before WC
Not verifying WC eligibility
Missing claim resubmission deadlines
Keeping incorrect insurance order
Failing to document calls and references
Practical Example
Scenario:
A patient visits for a back injury. The claim is sent to commercial insurance and gets denied as work-related.
Correct Action:
Confirm denial reason and date
Ask for WC details
Check system for existing WC policy
Update WC as primary
Resubmit claim to WC payer
If WC pays partially, bill Medicare (if applicable).
Key Tips for Efficient Handling
Always verify injury cause at registration
Maintain clear documentation of all calls
Use payer portals whenever possible
Follow up consistently on pending WC claims
Train staff to identify work-related cases early
Frequently Asked Questions (FAQs)
- What is Worker’s Compensation in medical billing?
Worker’s Compensation is insurance that covers medical expenses for injuries or illnesses that occur due to work-related activities. - Why was my claim denied as work-related?
The payer determined that the treatment is linked to a workplace injury, making WC insurance responsible instead of regular health insurance. - Can I bill both WC and commercial insurance?
No. WC must always be billed as primary. Commercial insurance should not be billed unless WC denies liability. - What if WC insurance details are unavailable?
Check internal systems, patient history, and payer portals. If no information is found, the claim may be transferred to patient responsibility. - When can Medicare be billed?
Medicare can be billed as secondary after WC processes the claim and leaves a remaining balance.
Conclusion:
Handling Worker’s Compensation denials may seem complex at first, but with a structured approach, it becomes manageable. The key lies in accurate information gathering, proper insurance sequencing, and timely claim resubmission.
By following the workflow outlined in this guide, you can reduce denials, improve reimbursement rates, and ensure compliance with billing regulations. Mastering this process is an essential skill for anyone working in medical billing and revenue cycle management.








