In medical billing, claim denials are common—but some are more confusing than others. One such denial occurs when a diagnosis (DX) code is deemed inconsistent with the patient’s age. This type of denial can delay reimbursements and create extra work if not handled properly. If you’re new to medical billing or looking to refine your workflow, this guide will walk you through everything you need to know—from understanding the denial to resolving it efficiently.
What Does “Diagnosis Inconsistent with Patient’s Age” Mean?
Insurance companies use strict validation rules when processing claims. One of these checks ensures that the diagnosis code matches the patient’s age group. Example: A diagnosis code for age-related osteoporosis submitted for a child patient; A pediatric condition billed for an elderly patient. When such mismatches occur, the claim is denied because the diagnosis is considered medically inappropriate for that age.
Step-by-Step Workflow to Handle This Denial
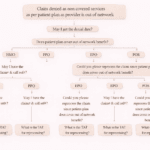
- Identify the Denial Details – Collect denial date, claim number, and invalid DX codes. Ask: “May I get the denial date?” “Which diagnosis code is invalid?”
- Check Patient Payment History – If previously paid, request reprocessing and collect TAT, claim & call reference; If not, proceed.
- Determine Timely Filing Limits – Ask correction timeline; If within limit → proceed; If expired → follow client instruction.
- Coordinate with Coding Team – If DX incorrect → update & resubmit; If correct → proceed with appeal.
- Submit Corrected Claim – Update diagnosis and resubmit within filing limits with proper documentation.
- Appeal the Denial – If DX valid → collect appeal details, submit with medical documentation; If deadline passed → follow client or write off.
Important Notes to Remember
Calculate timelines from denial date; Follow client instructions; Maintain documentation for calls, references, and submissions.
Practical Example
10-year-old patient billed with senile cataract DX → denied → Verify → Send to coding → Update to pediatric DX → Resubmit → Claim processed.
Key Tips for Handling Age-Related DX Denials
Double-check diagnosis codes; Use age-appropriate coding; Verify denial reason; Communicate with payer & coding team; Track deadlines.
Frequently Asked Questions (FAQs)
- Why do insurance companies reject diagnosis codes based on age?
Insurance systems automatically check for medical logic. If a diagnosis doesn’t match the patient’s age group, the claim is flagged and denied. - Can I resubmit the same claim without changes?
Only if you have proof of previous payment and the payer agrees to reprocess. Otherwise, correction or appeal is required. - What happens if the timely filing limit is exceeded?
Usually, the claim is written off. However, some clients may still request submission, so always confirm instructions. - Who is responsible for correcting diagnosis codes?
The coding team is responsible for reviewing and correcting diagnosis codes, not just the billing team. - When should I send an appeal instead of a corrected claim?
Send an appeal when the diagnosis code is correct, supported by documentation, and the denial is unjustified.
Conclusion:
Handling age-related diagnosis denials requires a structured approach with accurate coding, timely action, and clear communication. Following this workflow helps reduce denials and improve revenue cycle performance.