In medical billing, claim denials are a common challenge that can delay payments and increase administrative workload. One such denial reason that often confuses beginners is when the date of death precedes the date of service. At first glance, this may seem straightforward, but in real-world scenarios, this denial usually occurs due to data entry errors, incorrect updates, or system mismatches. This guide explains the issue in simple terms and shows how to handle it step by step.
What Does This Denial Mean?
This denial occurs when the date of service on the claim is after the patient’s recorded date of death in the payer’s system.
Example:
Date of death March 10, 2023
Date of service March 15, 2023
In this situation, the insurance system assumes the patient was already deceased when the service was provided, leading to claim rejection.
Why Does This Happen?
Even though it seems unusual, this denial is often caused by administrative or system issues.
1. Incorrect Date of Service Entry
Typing mistakes during claim submission or selecting the wrong date from the system.
2. Incorrect Date of Death in Payer System
Insurance records may be updated incorrectly or not synchronized properly.
3. Data Sync Issues
Mismatch between hospital records and payer systems due to delayed updates.
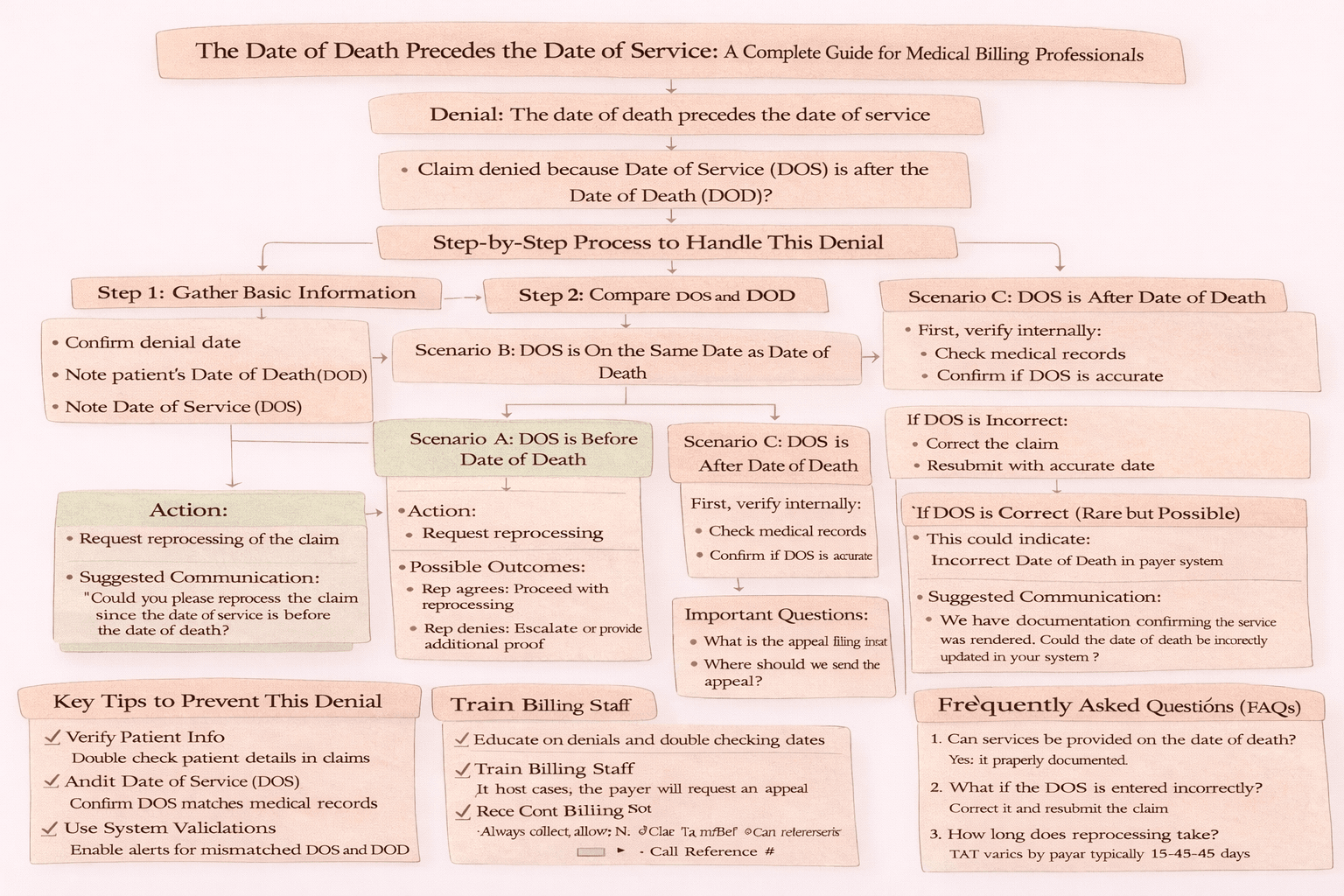
Step-by-Step Process to Handle This Denial
A structured approach helps resolve this denial efficiently.
Step 1: Gather Basic Information
Collect denial date, date of death, and date of service.
Step 2: Compare Date of Service and Date of Death
Scenario A: Date of Service is Before Date of Death
This means the service was valid. Request reprocessing of the claim and ask for turnaround time, claim number, and call reference number.
Scenario B: Date of Service is On the Same Date as Date of Death
This is also valid since services can be provided on the same day. Request reprocessing. If denied, escalate or provide additional proof. Always collect turnaround time and reference details.
Scenario C: Date of Service is After Date of Death
This is the most complex case. First verify internally by checking medical records.
If the date of service is incorrect, correct the claim and resubmit.
If the date of service is correct, this may indicate an incorrect date of death in the payer system. Inform the payer and provide proof of service.
If Payer Requests Appeal
In many cases, the payer may ask for an appeal.
Next steps include asking for fax number or mailing address, appeal submission guidelines, and filing deadline. Always collect claim number and call reference number for tracking.
Key Tips to Prevent This Denial
Verify patient information carefully before claim submission.
Double check date of service against medical records.
Use system validations to catch mismatched dates.
Maintain proper documentation including medical notes and service logs.
Train billing staff to review critical fields before submission.
Real-World Example
A claim was submitted with date of service June 12 and payer recorded date of death June 10. After review, the patient was alive during service and the payer had incorrect records. The provider submitted an appeal with medical documentation, the payer corrected the date of death, and the claim was reprocessed successfully.
Frequently Asked Questions (FAQs)
1. Can services be billed on the same day as death?
Yes, services provided on the same day are valid if properly documented.
2. What if the payer refuses reprocessing?
Submit a formal appeal with supporting medical records.
3. How long does reprocessing take?
It usually takes around 15 to 45 days depending on the payer.
4. What documents are needed for appeal?
Medical records, physician notes, proof of service date, and claim details.
5. Is this denial always due to billing errors?
No, it can also happen due to incorrect updates in the payer’s system.
Conclusion
This denial may look simple but often requires careful investigation. The issue usually comes from incorrect data entry or system mismatches. By verifying dates, communicating clearly with payers, documenting everything, and following a structured workflow, you can resolve this denial efficiently. A careful and consistent approach will help ensure faster reimbursements and smoother billing operations.