Procedure Code is Not Paid Separately (Denial Code 234) – Simple Guide for Claim Follow-Up
Many medical billing professionals face Denial Code 234, which means:
“This procedure is not paid separately.”
In simple words, the insurance is saying that the denied CPT code is bundled with another CPT code and will not be paid individually.
This guide explains the exact on-call workflow you should follow to handle this denial quickly and correctly.
What Does Denial Code 234 Mean?
Denial Code 234 = Procedure not paid separately
This happens when:
• The procedure is bundled
• It must be billed along with a primary CPT
• It is considered included in another service
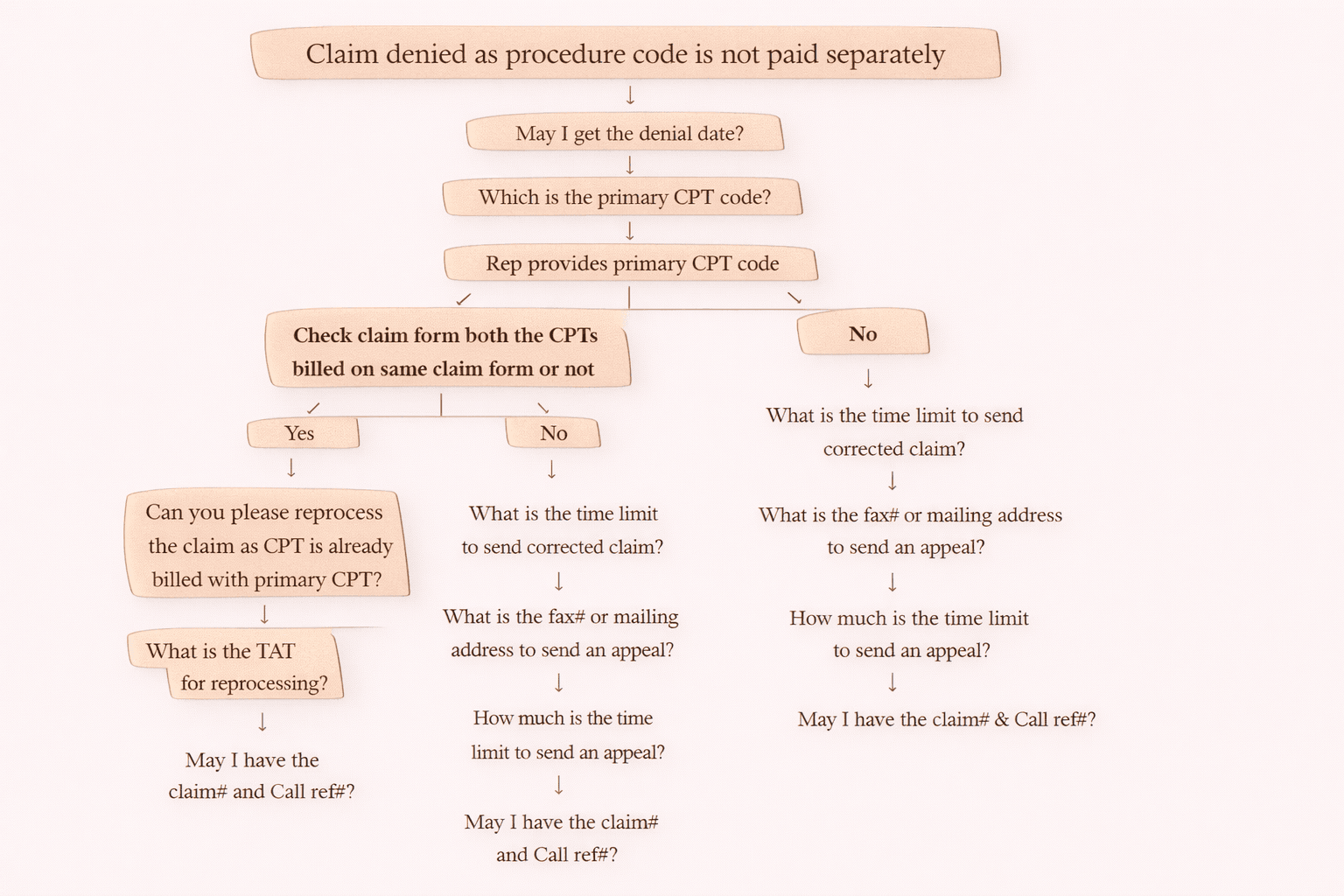
On-Call Scenario: How to Handle Denial Code 234
Step 1: Confirm the Denial
Start the call with:
“Claim denied as procedure code is not paid separately.”
Then ask:
Step 2: Ask for Denial Date
“May I get the denial date?”
Step 3: Identify the Primary CPT Code
Ask the representative:
“Which is the primary CPT code?”
The rep will either provide the primary CPT code correctly or not.
Scenario 1: Rep Provides Primary CPT Code
Now verify if both CPT codes were billed correctly.
Step 4: Check Claim Form
Check whether both CPTs were billed:
• On the same claim form (same claim number)
• On separate claim forms
If Both CPT Codes Were Billed on the Same Claim
Then politely request reprocessing:
“Can you please reprocess the claim as CPT is already billed with primary CPT?”
Next ask:
“What is the TAT for reprocessing?”
(TAT = Turnaround Time)
Finally take documentation:
“May I have the claim number and call reference number?”
If Both CPT Codes Were NOT Billed on Same Claim
Then ask:
“What is the time limit to send a corrected claim?”
Next ask:
“What is the fax number or mailing address to send an appeal?”
Then confirm:
“How much is the time limit to send an appeal?”
Finally take details:
“May I have the claim number and call reference number?”
Scenario 2: Rep Does NOT Provide Primary CPT Code
In this case, do not waste time guessing.
Step 1: Assign to Coding Team
Assign the claim to the coding team to identify the correct primary CPT.
After Coding Team Response
Case A: Primary CPT is correct but not in system
If the primary CPT code is not available in system:
- Create the CPT code
- Resubmit both CPT codes together
Extra Tips to Resolve Denial Code 234 Faster
If you have access to tools like:
• Encoder
• Find-A-Code
• CPT bundling tool
Then check whether the denied CPT can be billed alone.
If CPT Can Be Billed Alone
Call insurance and request reprocessing.
If Rep Refuses
Send an appeal with supporting documentation.
Tools to Identify Bundled CPT Codes
Use these tools to check bundling:
• Encoder tools
• CPT Assistant
• Find-A-Code
• NCCI edits / bundling rules reference
• Internal billing system bundling edits
Conclusion
Denial Code 234 is common and easy to resolve if you follow the right steps:
Confirm denial date
Identify the primary CPT
Check whether both CPTs were billed together
Request reprocessing OR send corrected claim / appeal
Always note claim number + call reference number