Denial Code B7: Provider Not Certified/Eligible on Date of Service (Simple Explanation)
In medical billing, Denial Code B7 is one of the most common provider-related denials.
What does Denial Code B7 mean?
B7 Denial Message:
“This provider was not certified/eligible to be paid for this procedure/service on this date of service.”
This means the insurance payer is saying:
The provider (doctor or facility) was not eligible, credentialed, enrolled, or certified to get paid for that service on the date the patient was treated (DOS).
Why is B7 Denial Issued?
B7 mostly occurs due to credentialing or enrollment issues such as:
• Provider not active in payer system
• Provider contract terminated or expired
• License or certification expired
• Provider specialty mismatch
• Taxonomy code mismatch or invalid taxonomy
• Billing provider or rendering provider issues
On Call Scenario (Simple Version)
When the provider office calls insurance, use this flow:
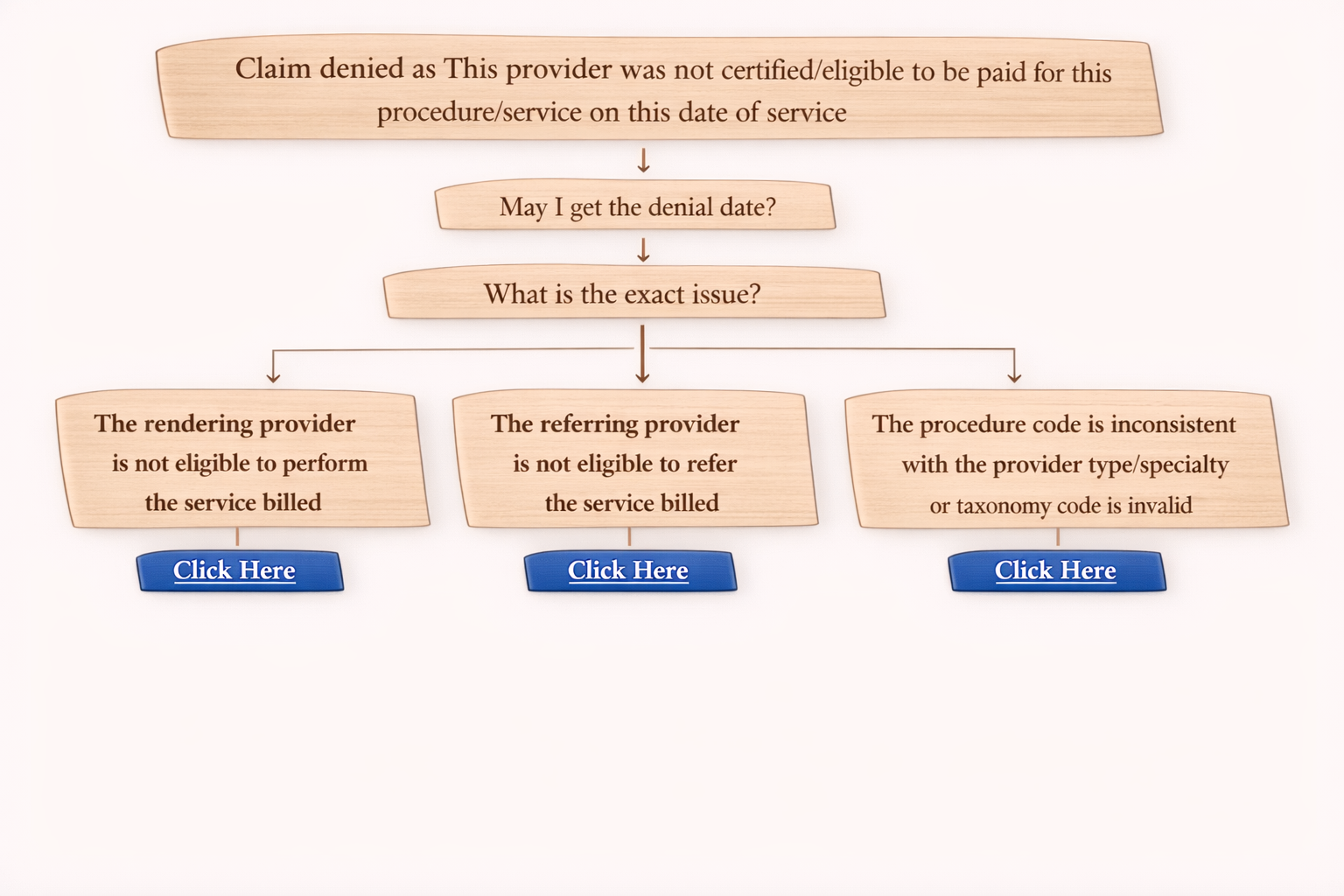
Step 1: Confirm the Denial
Agent:
“Claim denied as provider not certified/eligible to be paid for this procedure on this date of service (B7).”
Step 2: Ask for Denial Date
You:
“May I get the denial date?”
Step 3: Identify the Exact Issue
You:
“What is the exact issue in provider eligibility?”
Then the payer will usually mention one of the following three reasons.
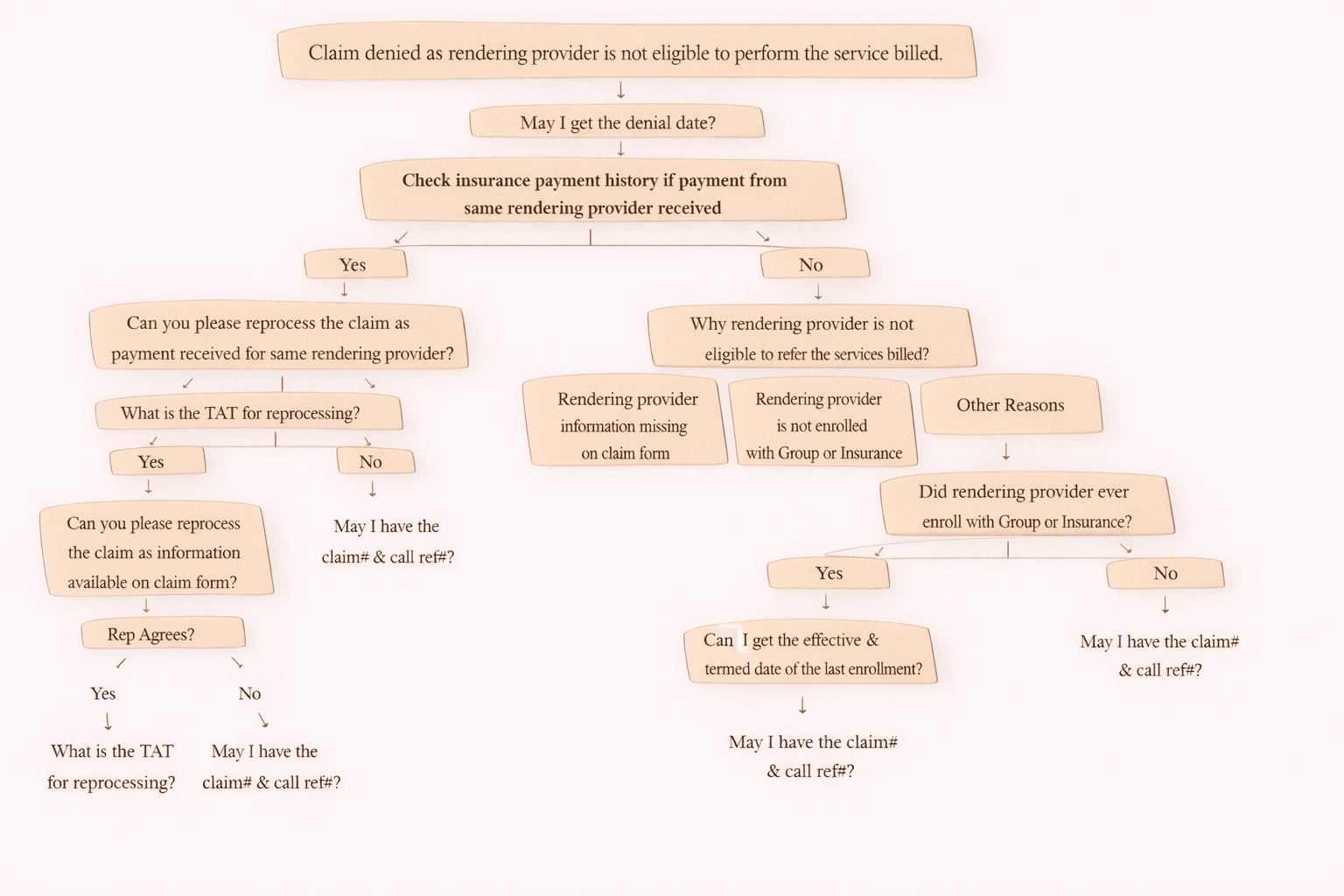
1) Rendering Provider Not Eligible (Denial 185)
Meaning
The rendering provider (who performed the service) is not eligible to perform or bill that service.
This happens when:
• Provider not credentialed with payer
• Provider specialty does not allow the procedure
• Provider enrollment inactive on DOS
• Provider contract terminated
How to Fix
Verify provider credentialing with payer
Check provider enrollment effective date
Confirm NPI and taxonomy are correct
Resubmit claim after correction
2) Referring Provider Not Eligible (Denial 183)
Meaning
The referring provider is not eligible or authorized to refer the service billed.
Common reasons:
• Referring provider NPI inactive
• Referring provider not enrolled with payer
• Referral not allowed for that specialty/provider type
• Invalid referring provider details
How to Fix
Confirm referring provider NPI and name
Check if referral is required and valid
Update claim with correct referring provider information
Resubmit claim
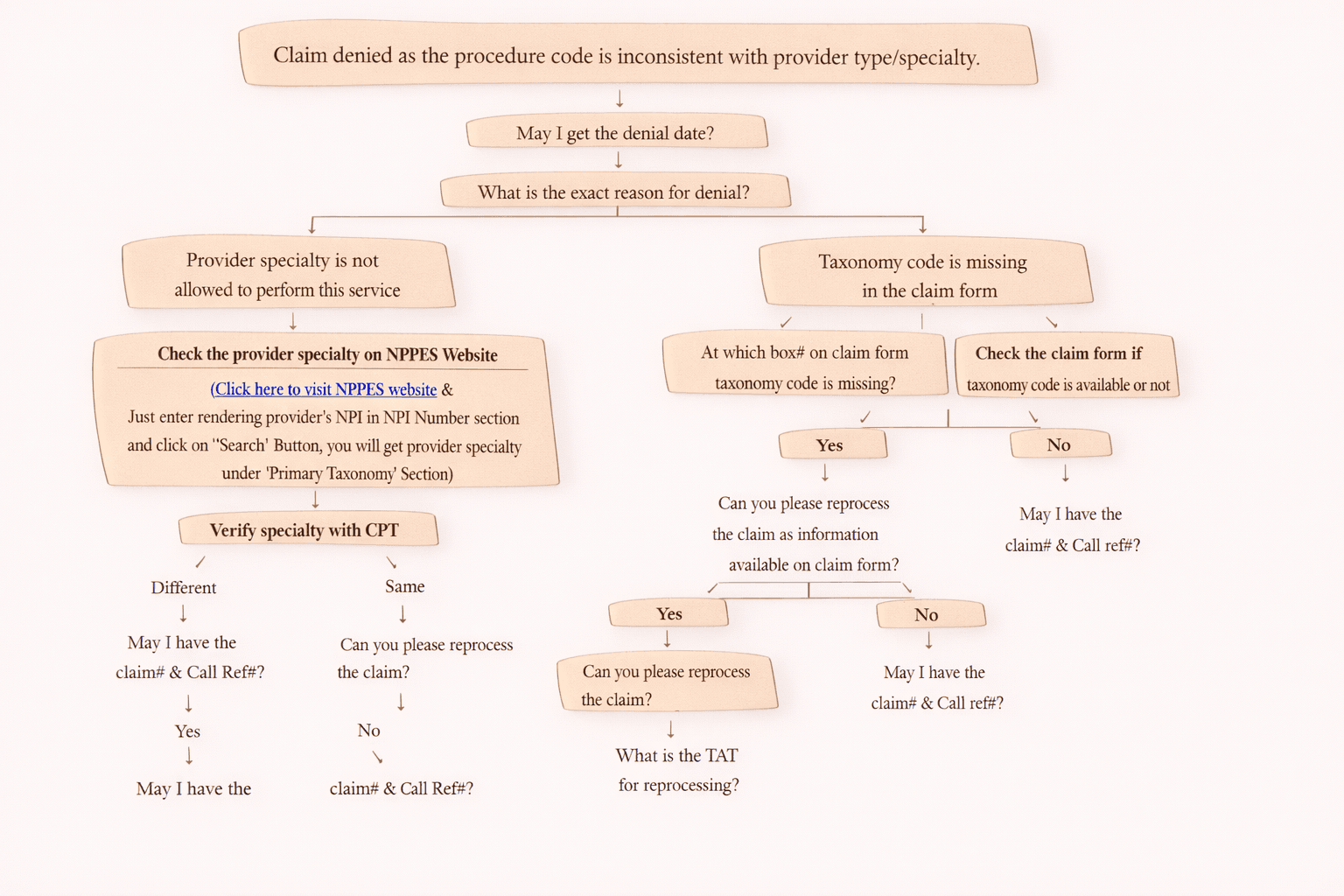
3) Procedure Code Inconsistent With Provider Type (Denial 8)
Meaning
The procedure billed does not match the provider specialty or the taxonomy is incorrect or invalid.
Example cases:
• Provider bills a procedure not allowed for their specialty
• Taxonomy code incorrect or expired
• Provider type not eligible for that CPT code
How to Fix
Verify correct taxonomy code on claim
Confirm provider specialty with payer
Validate CPT allowed for provider type
Correct the claim and resubmit
Quick Checklist to Avoid B7 Denial (Best Practice)
To prevent B7 denials in the future:
Verify provider credentialing before billing
Ensure billing and rendering NPI are active
Keep provider contract and license updated
Confirm taxonomy code is correct
Check procedure allowed for provider specialty
Final Notes (Important)
Denial Code B7 is not always a coding issue.
Most of the time it is a:
Credentialing, enrollment, or contract issue.
So always verify:
• Provider enrollment status
• Effective date vs Date of Service
• Taxonomy and specialty alignment