Denial Code 49: Routine/Preventive Services Not Covered – Causes & How to Fix It
Medical billing denials are common, but some denials are easier to resolve when you understand the reason behind them. One such denial is Denial Code 49, which usually happens when the claim is billed as a routine or preventive service.
This guide explains Denial Code 49, why it occurs, and the step-by-step process to resolve it.
What is Denial Code 49?
Denial Code 49 means:
The service is not covered because it is considered a routine/preventive exam or a diagnostic/screening procedure done along with a routine exam.
In simple words, the insurance is saying:
• This service is routine or preventive
• Routine services are not covered under this plan
• So payment is denied
Why Does Denial Code 49 Occur?
This denial mainly occurs due to the diagnosis code used in the claim.
Main Reason:
The claim is billed with a routine diagnosis code.
Most routine diagnosis codes start with “Z” (ICD-10 codes).
Examples:
• Z00.00 – General adult medical exam without abnormal findings
• Z00.01 – General adult medical exam with abnormal findings
Insurance may treat these as preventive or routine services and deny payment if the plan does not cover them.
How to Resolve Denial Code 49
The denial can sometimes be resolved if the diagnosis is updated correctly.
Fix:
• Review the diagnosis code
• If supported by documentation, replace the routine “Z” diagnosis with a proper medical or clinical diagnosis code
• Submit a corrected claim within the allowed time limit
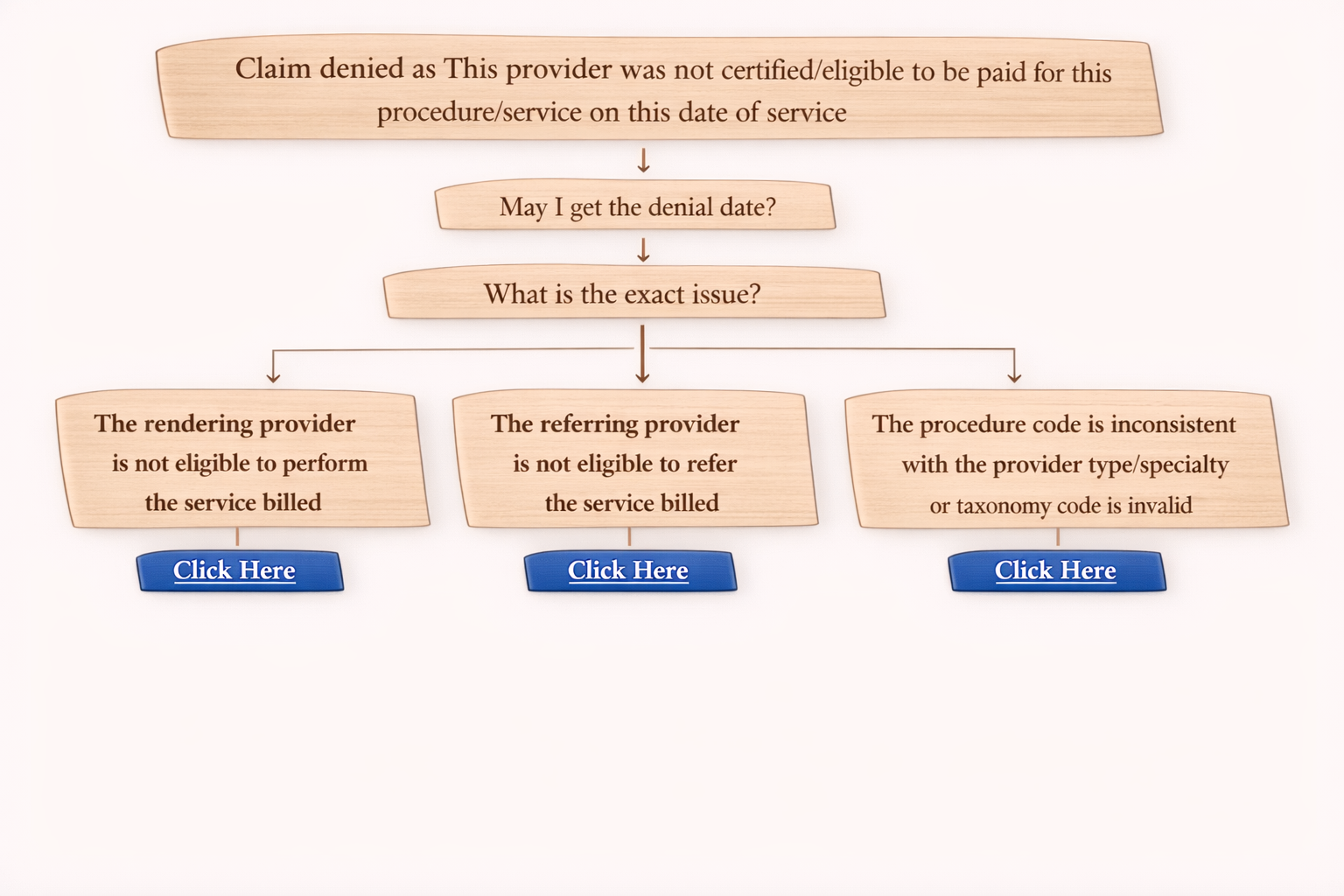
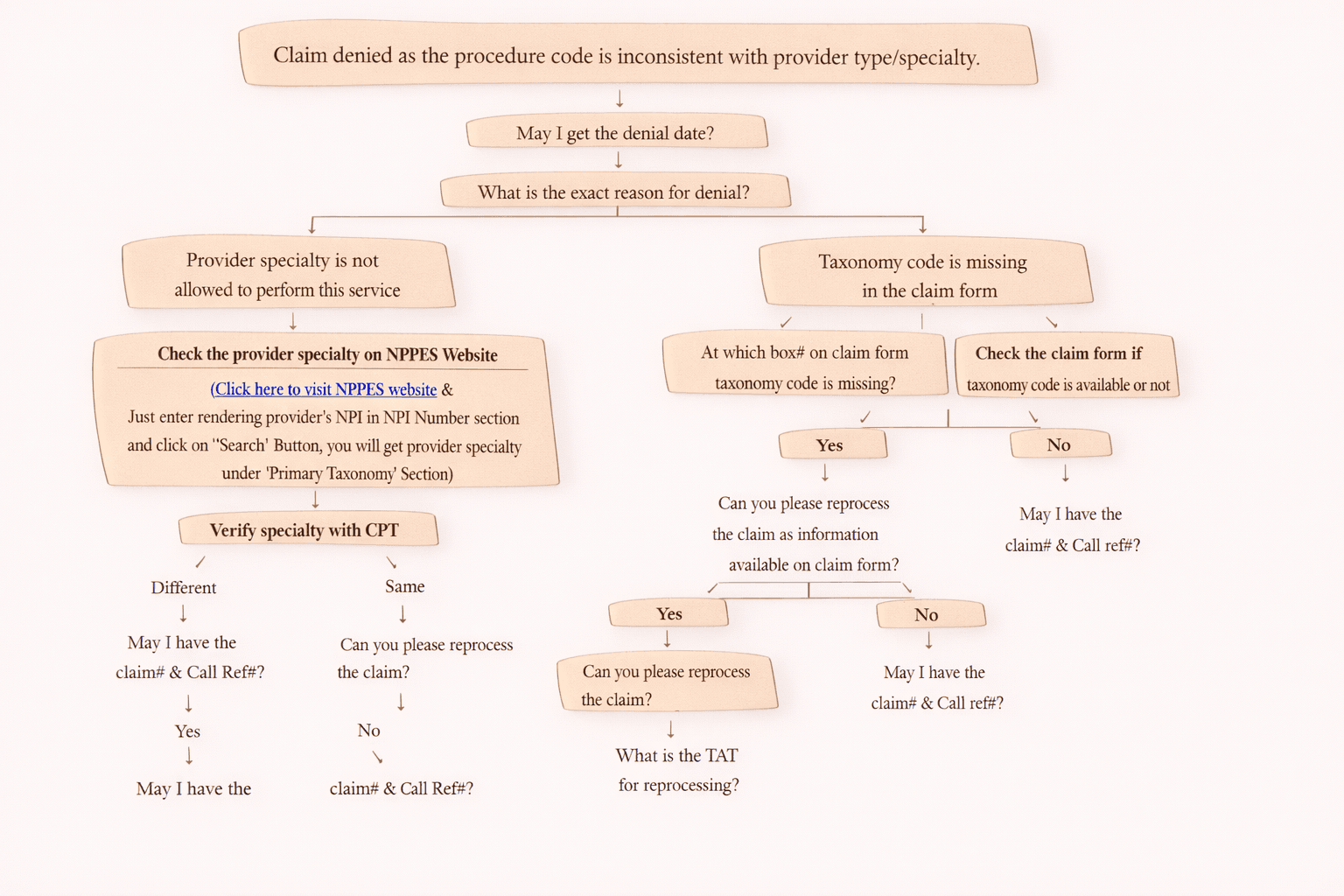
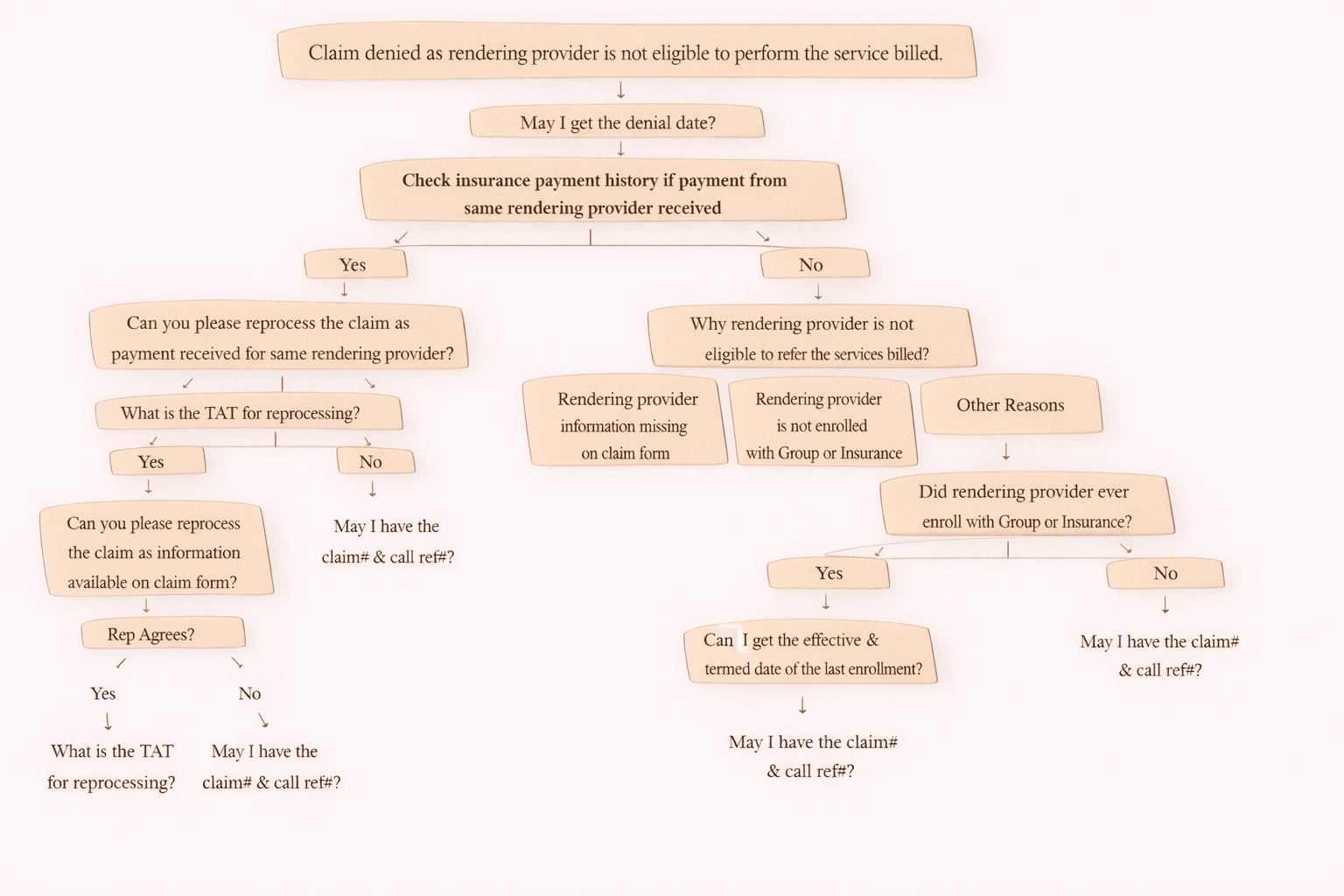
Call Flow / On-Call Scenario for Denial Code 49
When you are on a call with insurance, follow this standard set of questions.
On Call Workflow
- Claim denied as routine services not covered
- Ask: “May I get the denial date?”
- Ask: “What is the time limit to send a corrected claim?”
- Ask: “What is the fax number or mailing address for appeal submission?”
- Ask: “What is the time limit to send an appeal?”
- Ask: “May I have the claim number and call reference number?”
This helps you document everything properly and avoid missing deadlines.
Important Note for Billing Team (Internal Process)
This denial should first be routed correctly.
Step 1: Assign to Coding Team
• Always send the claim to coding team for diagnosis review
• Coding team will confirm if diagnosis should be corrected
Step 2: Submit Corrected Claim
If the coding team provides a new diagnosis:
• Update the claim with the correct diagnosis code
• Submit corrected claim to insurance
• Ensure the filing time limit is not crossed
Even if the time limit is crossed, some clients still request corrected claim submission. Follow client instructions.
If Coding Team Confirms Diagnosis is Correct
Sometimes the coding team confirms the Z diagnosis is accurate.
In such cases:
• Routine service is truly not covered
• It becomes patient responsibility or bill secondary payer
Secondary / Consecutive Payer Verification
Before billing secondary payer, you must verify eligibility.
How to verify:
• Check payer portal (if access available)
• Or call insurance to verify
If secondary or consecutive payer is active on DOS (Date of Service):
Bill the secondary payer
If no other payer exists or policy inactive:
Release claim to patient
Appeal Handling for Denial Code 49
Sometimes clients prefer appeal instead of patient billing.
Appeal Rules:
• Calculate appeal time limit from denial date
• If appeal is within time → submit appeal
If appeal time limit is crossed:
Write off the claim (unless client requests appeal after the limit)
Key Takeaways (Quick Summary)
Denial Code 49 is mostly due to routine diagnosis (Z codes)
First action: send to coding team for diagnosis correction
Submit corrected claim if valid diagnosis exists
If routine diagnosis is correct: bill patient or secondary payer
Verify secondary payer eligibility before billing
If appeal needed, ensure it is within appeal time limit