Claim Denied as “Not Medically Necessary”? Here’s the Simple Process to Fix It (Step-by-Step)
In medical billing, one of the most common denial types is:
Denied as “Medical Necessity” (Not Medically Necessary)
This means the insurance payer believes the service was not required medically, or the documentation/diagnosis code did not justify the procedure.
In this blog, we’ll explain the simple process to handle a Medical Necessity denial and recover payment if possible.
What Does “Not Medically Necessary” Denial Mean?
A claim may be denied as non-covered because:
• The service is not considered medically required
• The diagnosis (DX/ICD-10) does not support the CPT procedure
• The payer guidelines do not approve the service for that diagnosis
In short:
The payer is saying, “This treatment was not required based on the diagnosis submitted.”
On-Call Scenario: Medical Necessity Denial Workflow (Simple Steps)
When the provider calls the insurance payer for a denied claim, follow this simple flow:
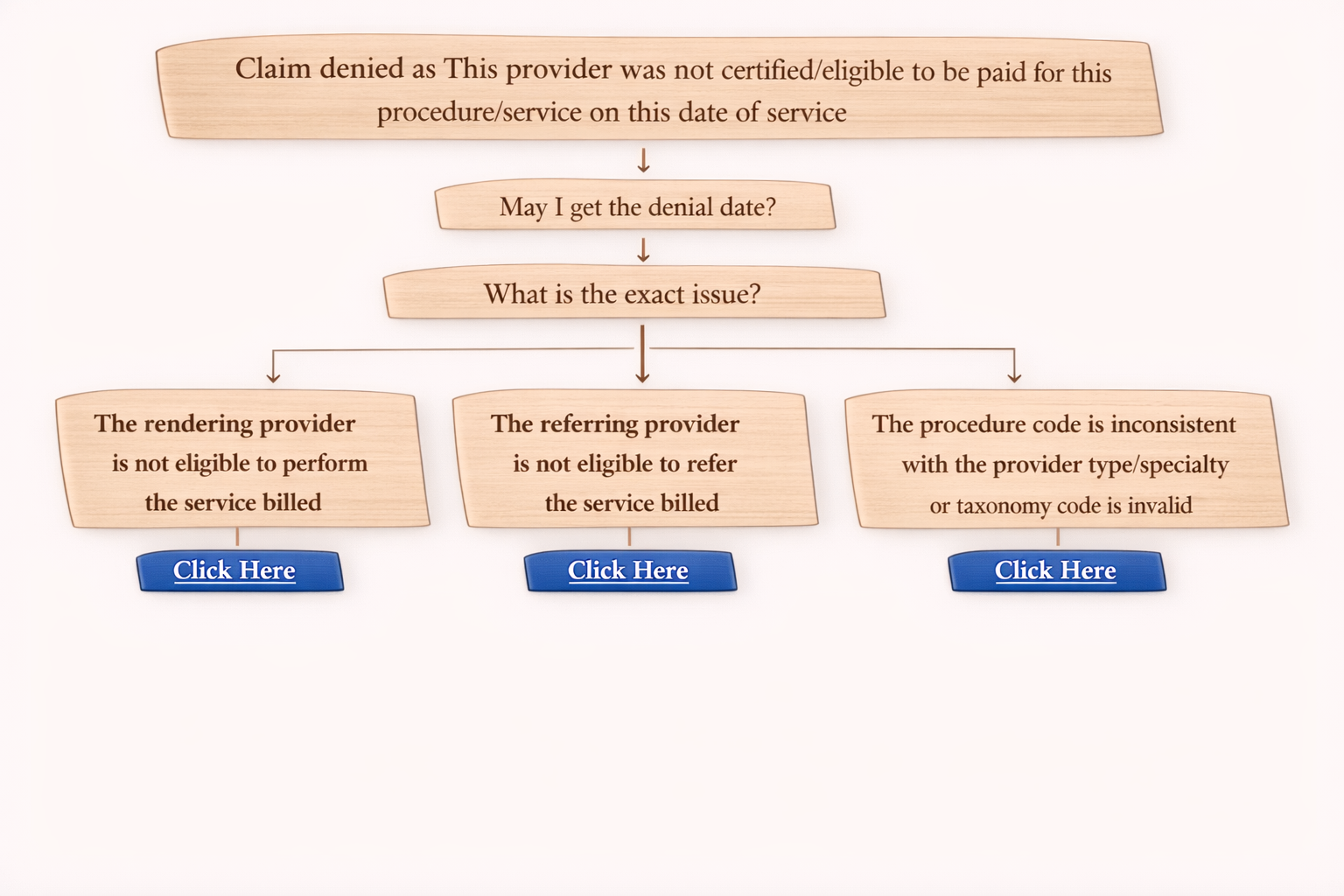
Step 1: Confirm the Denial
Start by stating:
“The claim is denied as not medically necessary.”
Step 2: Ask for Denial Date
Ask:
“May I get the denial date?”
This is important because denial date decides the time limit for:
• corrected claim submission
• appeal submission
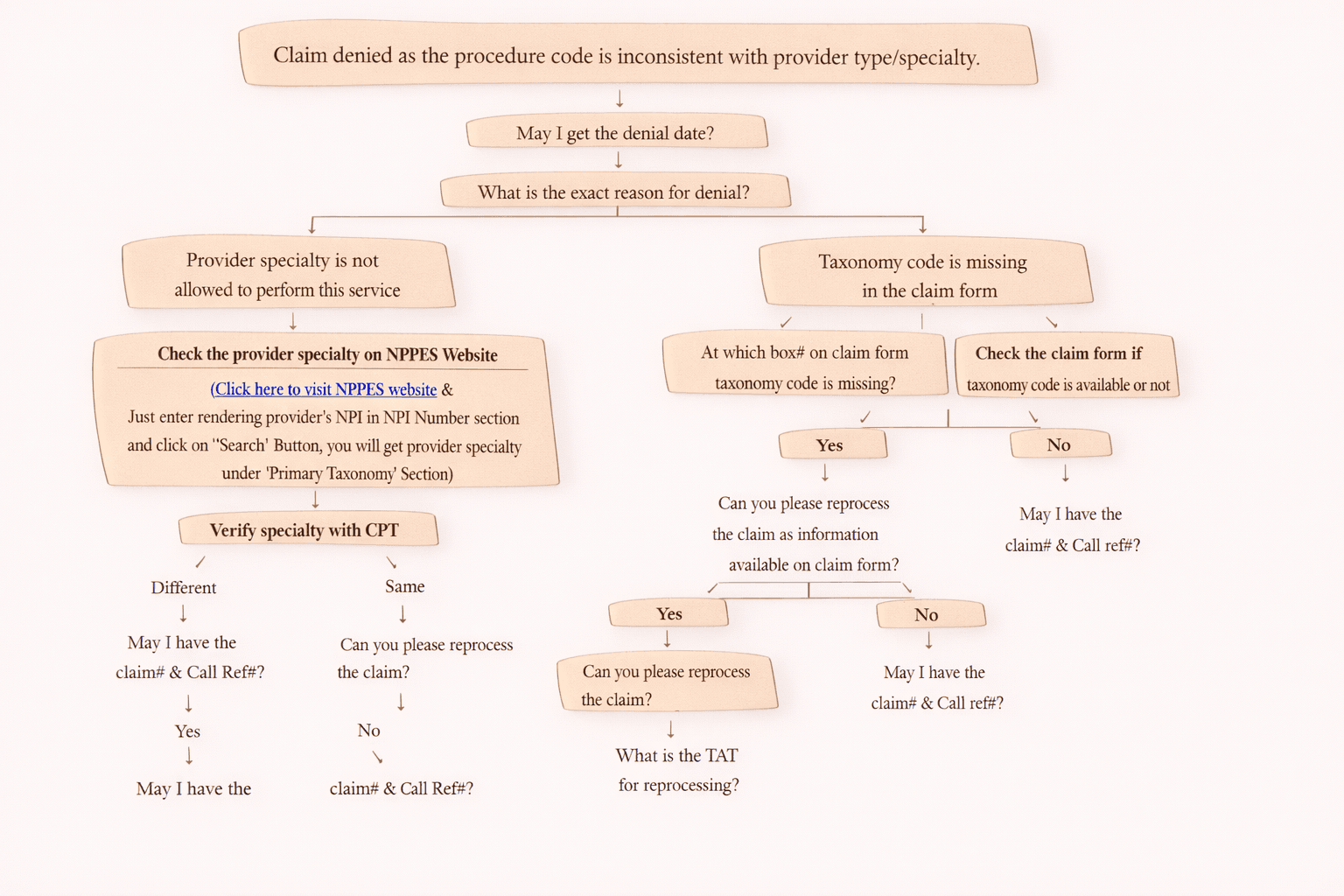
Step 3: Ask Reason for Denial
Then ask:
“What is the reason for medical necessity denial?”
The payer will mention something like:
• DX not matching CPT
• payer policy limitations
• no prior authorization
• missing supporting notes
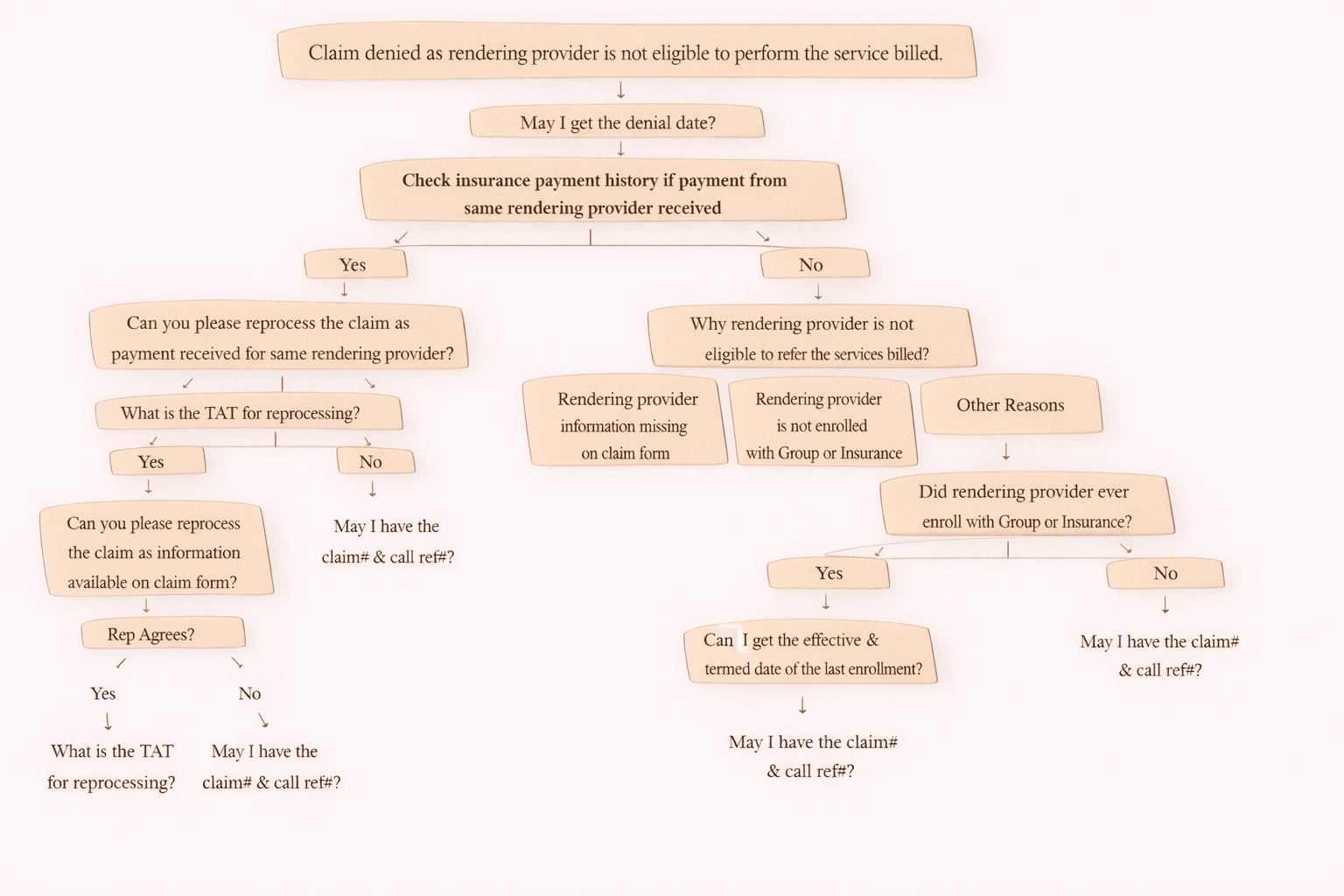
Step 4: Check Payment History (DX + CPT Match)
Now you need to check:
Has the same CPT + DX been paid earlier for this patient?
This is a key trick in denial handling.
If YES (Same CPT + DX Paid Earlier)
Then say:
“Can you please reprocess the claim as payment was received earlier for the same CPT and diagnosis code?”
Next, ask:
- “What is the TAT for reprocessing?”
(TAT = Turn Around Time) - “May I have the claim number and call reference number?”
This helps track the conversation and reprocessing request.
If NO (Same CPT + DX Not Paid Earlier)
Then the claim needs action like corrected claim / appeal.
Step 1: Ask time limit for corrected claim
Ask:
“What is the time limit to send a corrected claim?”
Step 2: Ask address/fax for appeal
Ask:
“What is the fax number or mailing address to send an appeal?”
Step 3: Ask appeal filing limit
Ask:
“How much is the time limit to send an appeal?”
Step 4: Take claim details
Finally, ask:
“May I have the claim number and call reference number?”
Important Note (Must-Do in Back-End Process)
Assign denial to Coding Team
This denial must be sent to the Coding Team to verify:
• Whether the diagnosis code is correct
• If a more appropriate diagnosis should be used to support CPT
Scenario 1: Coding Team Provides Correct DX Code
If coding team says the DX needs correction:
Submit a Corrected Claim by updating the correct DX code
(but only if time limit is not crossed)
Note:
Sometimes client may ask to submit corrected claim even after time limit — follow client instructions.
Scenario 2: Coding Team Confirms DX Code is Correct
If coding team confirms diagnosis is correct:
File an Appeal with documentation support.
Appeal Time Limit Rule:
• Calculate appeal filing limit from the denial date
• If time limit crossed → claim may need write-off (unless client says continue)
Important:
Some clients may still want appeal submission even after the time limit — work accordingly.
Conclusion:
A Medical Necessity denial is not always final. If handled properly, many claims can be recovered by:
reprocessing request (if history supports)
corrected claim submission (DX change)
appeal submission (if DX is correct)
The key is to:
• collect denial date
• check payment history
• confirm corrected claim / appeal time limits
• take claim number & call ref number