Claim Denial Code 181: Procedure Code Was Invalid on the Date of Service (Simple Guide)
In medical billing, one of the common denials faced by billing teams is:
Denial Code 181 – “Procedure code was invalid on the date of service.”
This denial usually occurs when the CPT/HCPCS code billed was not valid, inactive, or not acceptable for that service date. It may also happen due to incorrect new patient / established patient code selection.
In this blog, we will explain what Code 181 means, why it happens, and the best call scenario workflow to resolve it quickly.
What is Denial Code 181?
Denial 181 means the insurance payer is rejecting the claim because the procedure code used was invalid on the date of service (DOS).
This can happen when:
• The CPT code was not active during the DOS
• A wrong CPT code was used
• The code has been replaced/updated
• Incorrect new patient vs established patient codes were used
• Payer policy does not accept the billed CPT for that DOS
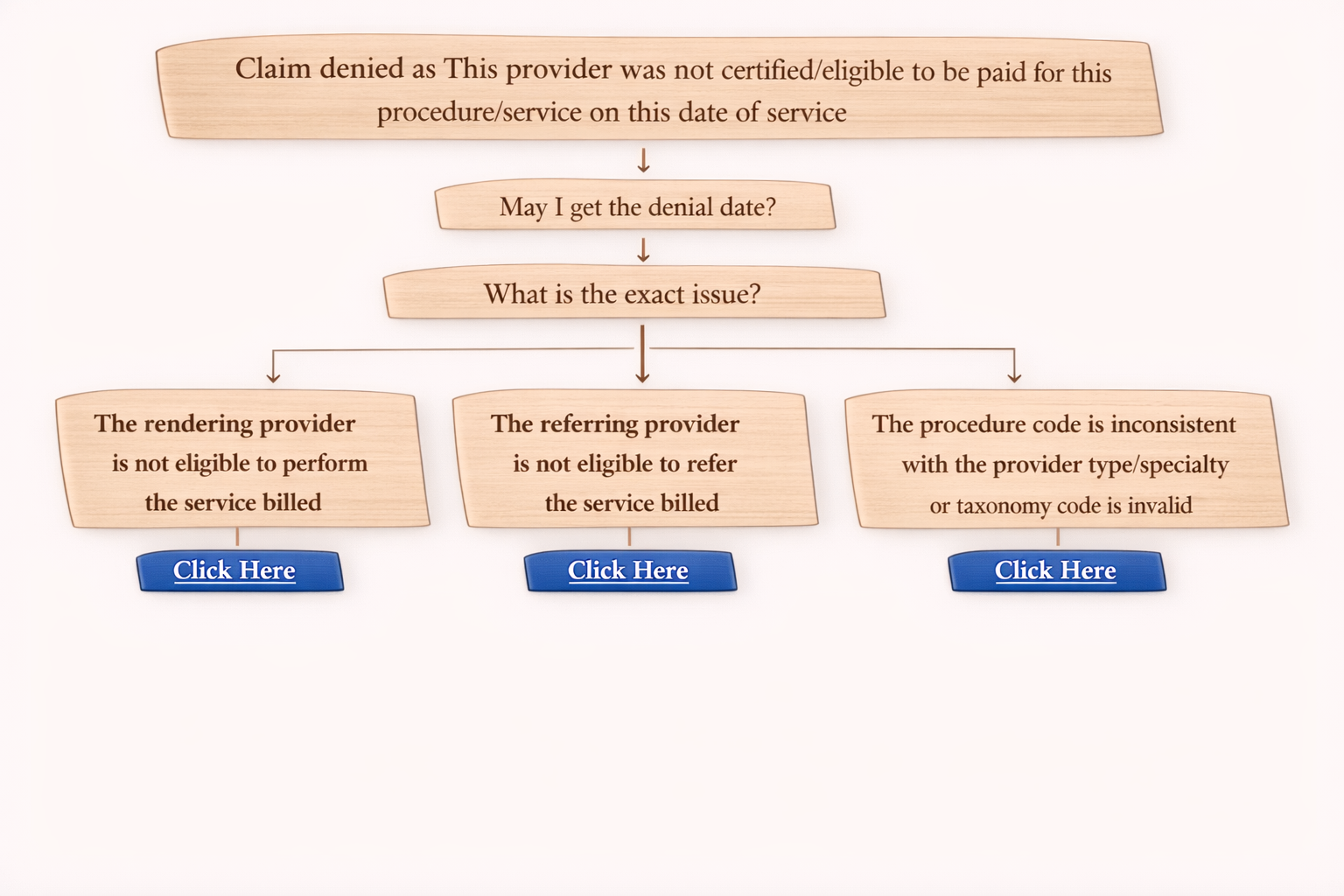
Step-by-Step Workflow to Handle Denial Code 181 (On Call)
When you call the insurance company for this denial, follow this simple flow.
Step 1: Confirm the Denial Date
First ask:
“May I get the denial date?”
This is important because appeal timelines depend on the denial date.
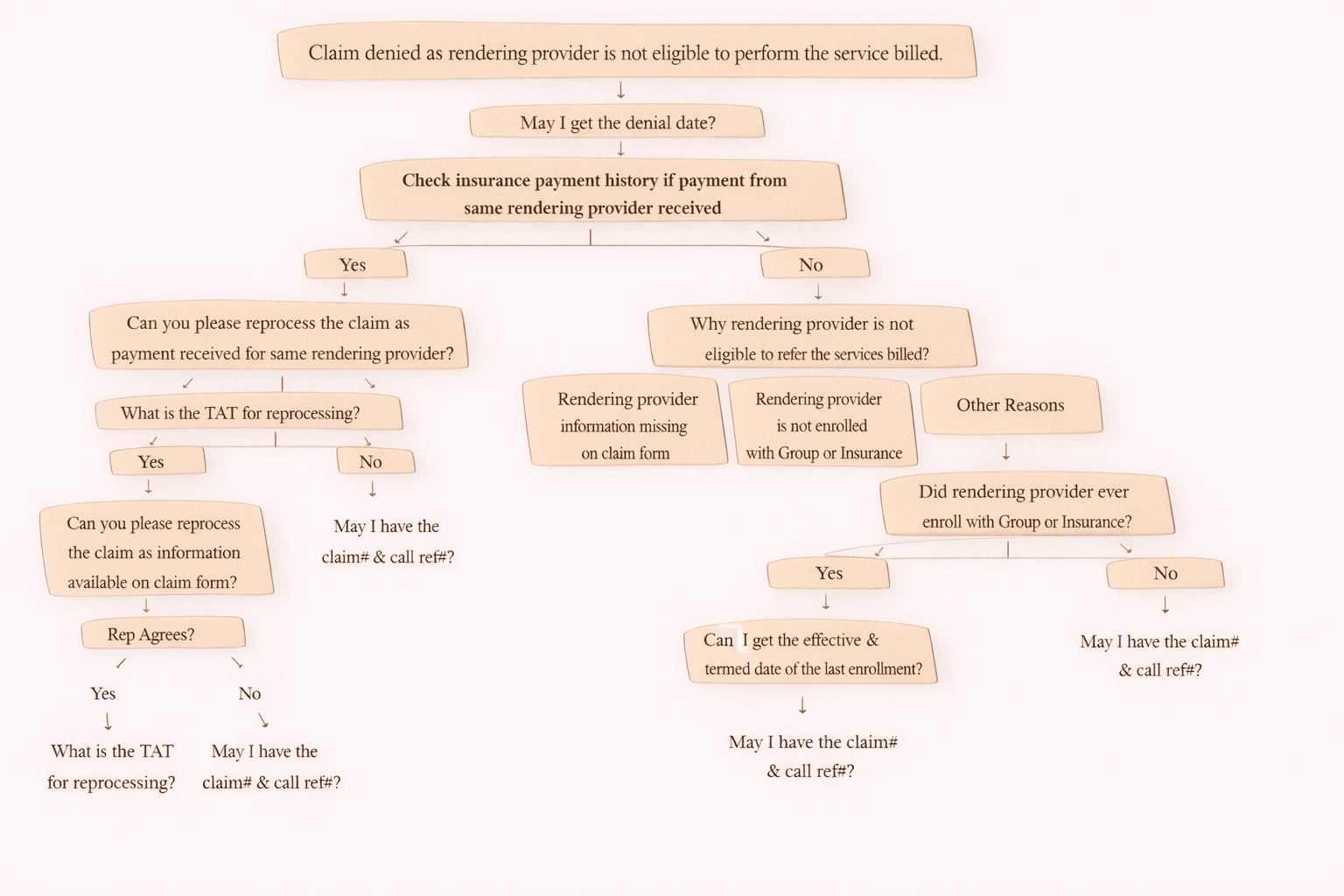
Step 2: Check for Similar Payment History
Next action:
Check insurance payment history
Ask / verify if the same CPT code was paid earlier by the same insurance.
If Same CPT Code Was Paid Earlier (YES)
If you see that the payer has already paid for the same CPT earlier:
Ask the payer:
“Can you please reprocess the claim as payment was received for same CPT?”
Then ask:
• “What is the TAT (Turnaround Time) for reprocessing?”
• “May I have the claim number & call reference number?”
This helps for tracking and follow-up.
If Same CPT Code Was NOT Paid Earlier (NO)
If there is no payment history for the same CPT, then it may be a true coding issue.
Ask:
“What is the time limit to send a corrected claim?”
Then ask:
• “What is the fax number or mailing address to send an appeal?”
• “What is the time limit to send an appeal?”
• “May I have the claim number & call reference number?”
Important Billing Notes for Denial Code 181
1. Assign to Coding Team
This denial should first be assigned to the coding team to confirm:
• Is the CPT code correct?
• If not, what is the correct CPT code?
2. If Coding Team Provides Correct CPT
Once correct CPT is received:
Update the claim with correct CPT
Submit as Corrected Claim, ONLY if the time limit is not crossed
Note:
Sometimes client may request to submit corrected claim even if the time limit is crossed — follow client instruction.
3. If Coding Team Confirms CPT is Correct
If coding confirms that CPT code is valid:
Send an appeal to insurance
Appeal must be sent within the appeal timely filing limit.
4. Appeal Time Limit Calculation
Always calculate appeal time limit from:
Denial date
• If not crossed → send appeal
• If crossed → write off (unless client asks to appeal anyway)
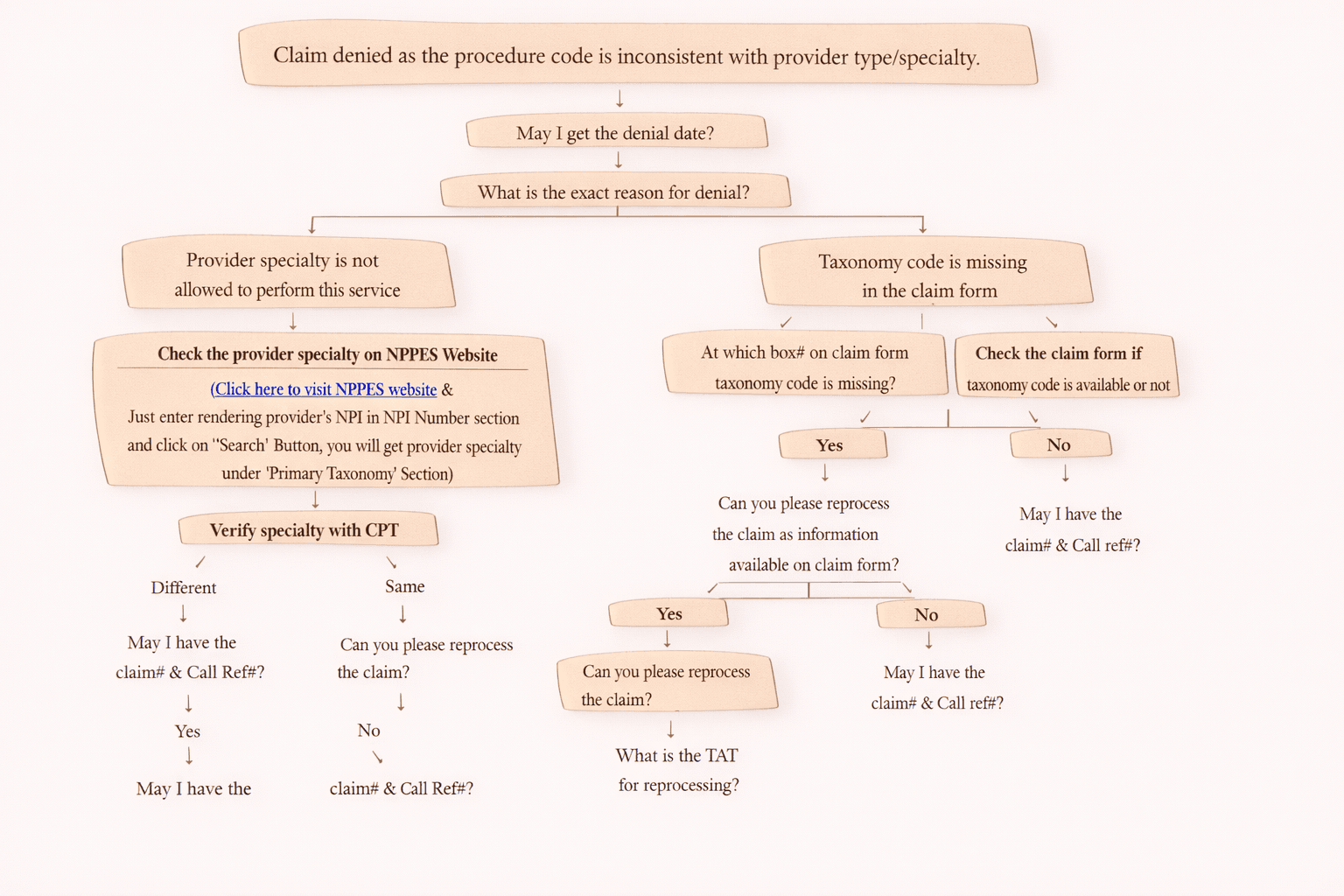
Common Issue: Invalid New Patient / Established Patient Codes
One of the common reasons for this denial is incorrect E/M selection.
Example:
• Billing 99204 (new patient) when the patient is actually established
• Billing 99214 (established) when patient qualifies as new patient
These mismatches can trigger payer edits and lead to Code 181 denial.
Conclusion:
Denial Code 181 is mainly a coding validity issue, but it can also be a payer processing issue. The best way to handle it is:
Confirm denial date
Check payment history for same CPT
If same CPT paid → request reprocess
If not paid → check corrected claim & appeal timely filing limit
Involve coding team always before resubmitting