Denial Code 146: Diagnosis Was Invalid for Date of Service (Simple Guide)
Insurance claim denials are common in medical billing, and one of the frequent denials is:
✅ Denial Code 146 – “Diagnosis was invalid for the date(s) of service reported.”
This denial means the diagnosis code (ICD-10) submitted on the claim is not valid for the date of service (DOS). Usually, the reason is that the diagnosis code was:
• not active during that date
• expired
• updated later
• or incorrect as per payer rules
In this guide, we’ll explain how to handle Denial 146 in a simple and professional way.
What Does Denial Code 146 Mean?
Denial 146 indicates that the diagnosis code billed on the claim is not acceptable for the service date mentioned.
Example:
• Date of service: 12/01/2019
• Diagnosis code used: maybe the code started after 2019 or was deleted before 2019
So, insurance will deny the claim saying:
Diagnosis was invalid for the date(s) of service reported
Denial Code 146 – Call Handling Workflow (On-Call Scenario)
When you call the insurance payer for this denial, follow this simple script flow:
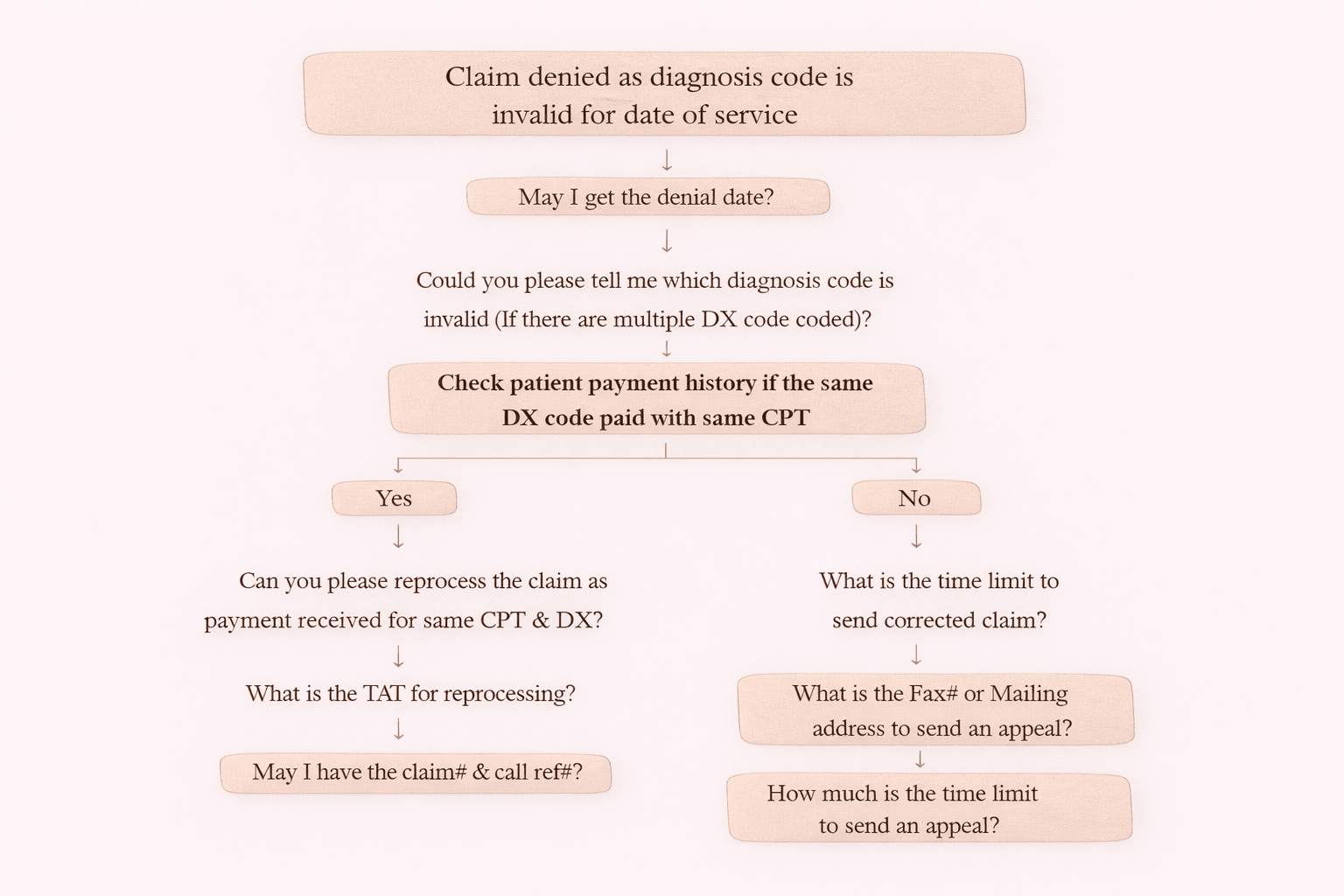
Step 1: Confirm Denial Details
Ask:
- May I get the denial date?
- Could you please tell me which diagnosis code is invalid?
If multiple diagnosis codes are present, ask for all invalid codes.
Step 2: Check Payment History (Important Step)
Next, check:
✅ Has the same Diagnosis code paid earlier with the same CPT code?
This helps you decide whether reprocessing is possible.
If Yes: Same DX & CPT Paid Earlier
If the payer confirms payment history exists, request reprocessing.
Ask the payer:
- Can you please reprocess the claim as payment was received earlier for the same CPT and DX?
- What is the TAT (Turnaround Time) for reprocessing?
- May I have the claim number and call reference number?
This is the best-case scenario because you can resolve the claim without corrected submission.
If No: No Payment History for Same DX & CPT
If the payer says it never paid with that diagnosis code, then the next step is corrected claim or appeal.
Ask:
- What is the time limit to send a corrected claim?
- What is the Fax number or Mailing address to send an appeal?
- How much is the time limit to send an appeal?
- May I have the claim number and call reference number?
Important Notes (Must Follow)
✅ 1. Assign to Coding Team
This denial must be sent to the coding team for review.
Coding team will:
• verify if diagnosis code is incorrect
• provide the correct diagnosis code (if needed)
✅ 2. If Correct DX Provided → Send Corrected Claim
Once correct diagnosis code is received:
📌 Submit corrected claim by updating the DX code only if time limit is not crossed.
⚠️ Sometimes, client may ask to submit corrected claim even if filing time is crossed — follow client instructions.
✅ 3. If Coding Team Says DX Code Is Correct → Send Appeal
If the coding team confirms the diagnosis code is correct:
📌 Proceed with appeal submission.
✅ 4. Appeal Time Limit Calculation
Always calculate appeal time limit from the denial date.
• If appeal time limit is not crossed → send appeal
• If appeal time limit is crossed → write off the claim (if policy allows)
⚠️ Sometimes, client may still want appeal even after time limit — follow client instructions.
Quick Summary: Denial 146 Action Plan
✅ Call Insurance
• Get denial date
• Identify invalid diagnosis code(s)
✅ Check payment history
• If same CPT + DX paid earlier → request reprocessing
✅ If not paid earlier
• Ask timely filing limit for corrected claim
• Ask appeal address/fax + appeal limit
✅ Send to Coding Team
• Correct DX? → Corrected claim
• DX correct? → Appeal