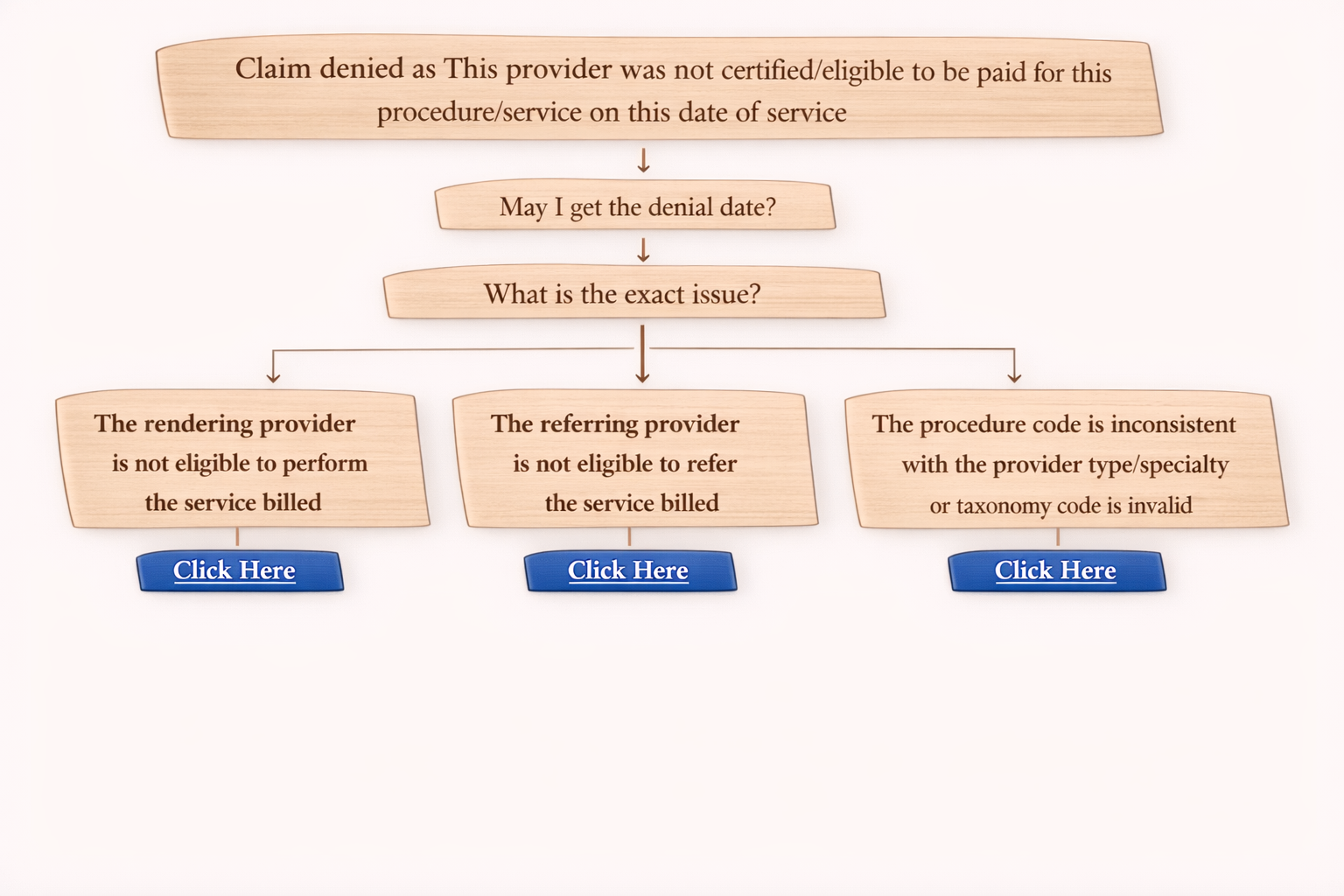
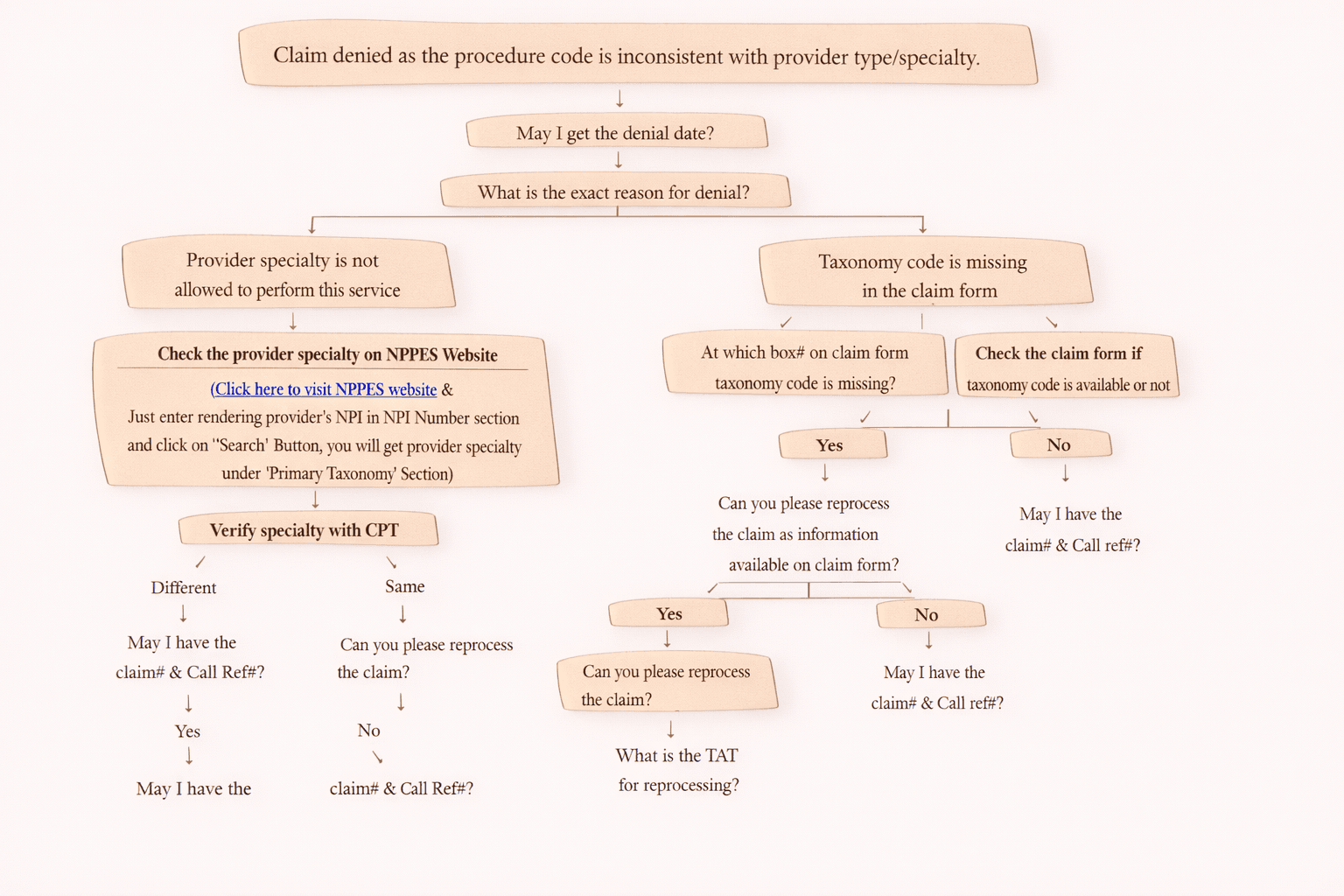
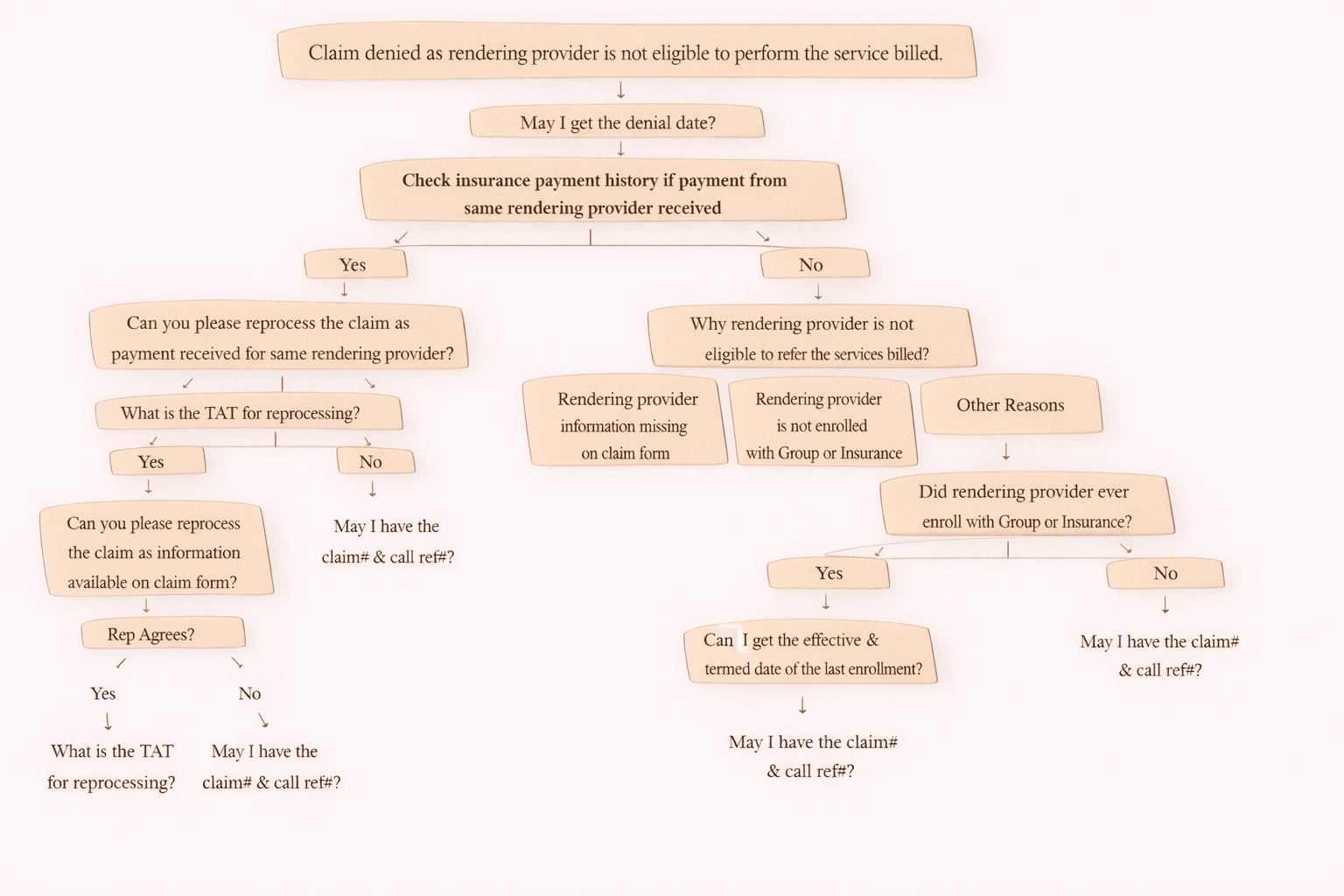
Denial Reason: Procedure Code Inconsistent With Modifier Used (Or Missing Modifier) – Simple Guide
In medical billing, one of the common claim denial reasons is:
“Procedure code inconsistent with the modifier used or a required modifier is missing.”
This means the insurance company believes the CPT/procedure code and modifier billed do not match, or the claim is missing a required modifier.
In this guide, we will explain:
• What this denial means
• How to handle the denial step-by-step
• When to reprocess, correct, or appeal the claim
• Special scenarios like LT/RT and Bilateral modifier 50
• Medicare rules for corrected claims
What Does This Denial Mean?
This denial usually happens when:
- A wrong modifier is used (example: LT instead of RT)
- A required modifier is missing (example: no modifier for a side-specific procedure)
- A procedure should have been billed differently (example: modifier 50 for bilateral)
Insurance companies check modifier rules strictly, so even a small mistake can cause denial.
Step-by-Step Process to Handle This Denial (Call Scenario)
Step 1: Confirm the Denial
When you call the insurance, first confirm:
✅ “Claim denied as procedure code inconsistent with modifier used.”
Step 2: Ask for the Denial Date
Before doing anything else, ask:
✅ “May I get the denial date?”
This is important because appeal and corrected claim timelines are calculated from this date.
Step 3: Check Patient Payment History
Now check internally:
➡️ Has the same CPT code already been paid with the same modifier earlier?
If YES (Same CPT + Same Modifier Already Paid)
That means the insurance has previously accepted that CPT/modifier combination.
Then request:
✅ “Can you please reprocess the claim as payment was received for the same CPT & modifier?”
Next questions:
• “What is the TAT (Turnaround Time) for reprocessing?”
• “May I have the claim number and call reference number?”
If NO (Not Paid Earlier With Same Modifier)
Then proceed to correction or appeal.
Step 1: Check Corrected Claim Time Limit
Ask:
✅ “What is the time limit to send a corrected claim?”
If still within time limit → corrected claim can be submitted.
Step 2: Ask Where to Send It
Ask:
✅ “What is the fax number or mailing address to send a corrected claim or appeal?”
Step 3: Check Appeal Time Limit
Ask:
✅ “How much is the time limit to send an appeal?”
Finally ask:
• “May I have the claim number and call reference number?”
Important Billing Notes (Must Follow)
1) Assign to Coding Team First
This denial should always go to the coding team to confirm:
• Correct modifier needed, OR
• Modifier already correct
Coding Team Outcome
✅ If coding team provides correct modifier
➡️ Submit Corrected Claim (if within time limit)
✅ If coding team confirms modifier is correct
➡️ Send Appeal
2) Corrected Claim Submission Rule
Before sending a corrected claim, always verify:
📌 Corrected claim timely filing limit is not crossed
If time limit crossed
• Normally → claim is written off
• Sometimes client may request submission anyway → follow client instruction
3) Appeal Submission Rule
When sending an appeal
✅ Calculate timeline from the denial date
If appeal limit crossed
• Normally → claim write-off
• Sometimes client may request appeal anyway → follow client instruction
Special Scenario: LT/RT Modifier and Bilateral Modifier 50
Sometimes the same CPT is billed separately like:
• CPT + LT (Left side)
• CPT + RT (Right side)
One side may get paid, while the other side gets denied as invalid modifier.
Correct Fix
Insurance may require billing as:
✅ Modifier 50 (Bilateral Procedure) in a single line
Corrected Claim Steps
- Void both lines (LT and RT)
- Create a new single line
- Add modifier 50
- Double the charge amount
Then submit the corrected claim to insurance.
Medicare Important Rule
📌 Medicare usually does NOT accept corrected claims directly in this scenario.
So the process should be:
- First send a Void claim for the paid CPT
- Then submit a new claim with modifier 50
Quick Summary (Easy Workflow)
If Same CPT + Modifier already paid
✅ Ask insurance to reprocess
✅ Collect claim #, call reference #, and TAT
If Not paid earlier
➡️ Send to coding team
• If modifier change needed → corrected claim
• If modifier correct → appeal
Always confirm:
✅ Denial date
✅ Corrected claim time limit
✅ Appeal time limit
✅ Fax or mailing address
Conclusion
The denial “procedure code inconsistent with modifier used or missing modifier” is a coding/modifier-related denial.
The best practice is to:
• Verify denial date
• Check payment history
• Send to coding team
• Submit corrected claim or appeal based on coding response
• Follow timely filing limits strictly