Denial Code 226: Medical Records Not Submitted on Time (Simple Explanation + Call Flow)
In medical billing, claim denials are common — but some denials can be avoided easily if we act quickly. One such denial is:
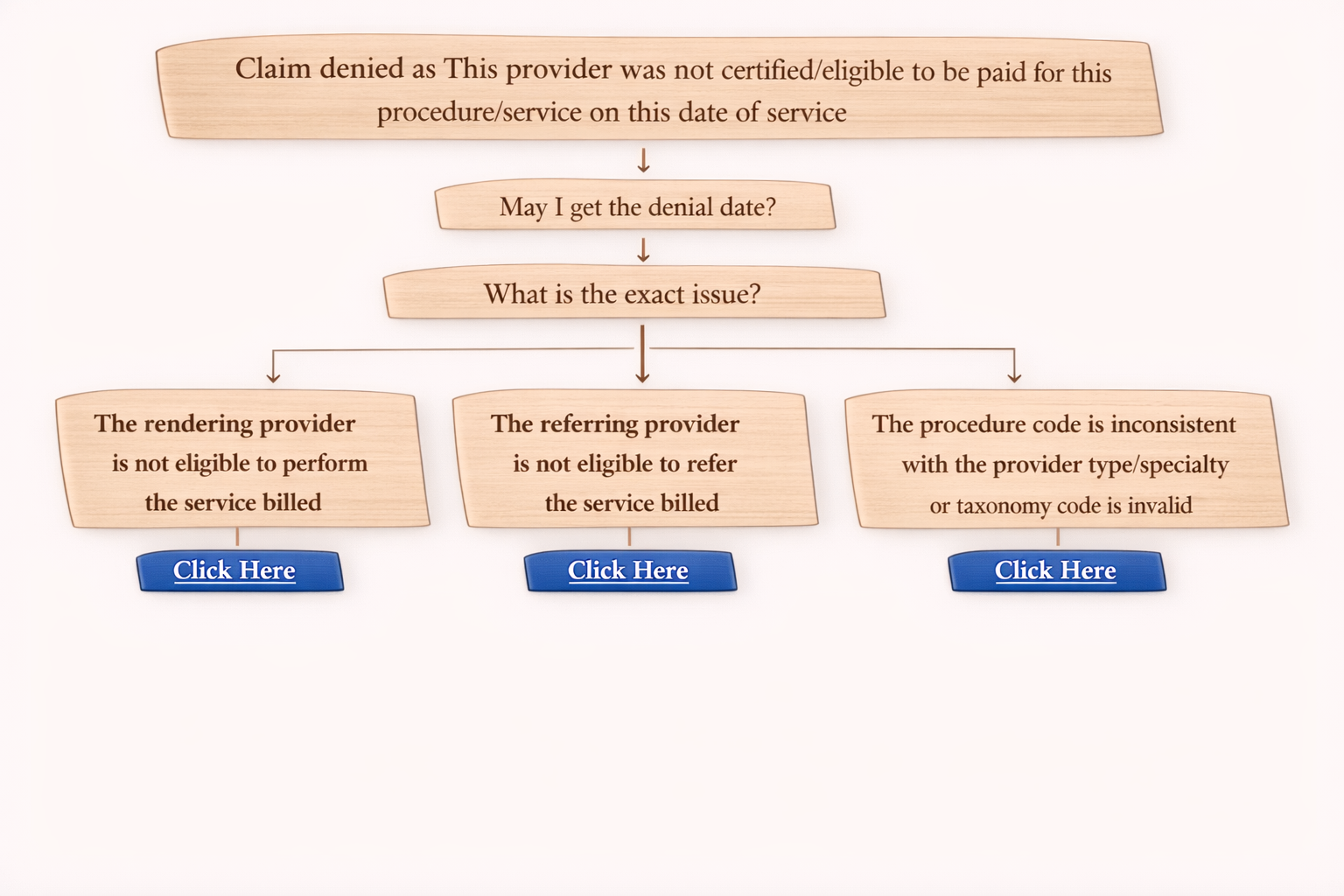
✅ Denial Code 226: Information requested from the Billing/Rendering Provider was not provided or was incomplete / not provided on time
This denial usually happens when the insurance company requested Medical Records (MR), but the provider did not send them within the deadline, or the documents sent were incomplete.
What Does Denial Code 226 Mean?
Denial Code 226 indicates that the payer asked for specific supporting documents such as:
• Medical records
• Chart notes
• Operative reports
• Clinical documentation
• Authorization proof
But those documents were either:
• Not submitted
• Submitted late
• Submitted incomplete or insufficient
So the claim gets denied due to missing documentation.
Most Common Scenario: Medical Records Requested
Typically, this denial appears like:
Claim Denied – Medical Records Requested / Not Received
That means the payer needs proof that the service was medically necessary.
On-Call Scenario / AR Call Script (Step-by-Step)
When calling the payer for Denial Code 226, follow this simple flow.
Step 1: Confirm the Denial Date
Ask:
➡️ “May I get the denial date?”
This is extremely important because the submission deadline depends on this date.
Step 2: Get the Submission Address (Fax or Mailing)
Ask:
➡️ “What is the fax number or mailing address to send the medical records?”
Some payers accept only fax, some accept mail, and some allow portal upload. Always confirm.
Step 3: Ask for the Time Limit
Ask:
➡️ “How much is the time limit to submit the records?”
Most payers allow limited timelines such as:
• 30 days
• 45 days
• 60 days
• 90 days
Step 4: Note Claim & Call Reference Details
Ask:
➡️ “May I have the claim number and call reference number?”
Always capture these details in notes because they help with future follow-ups and audit proof.
Important Note: Time Limit Calculation
This is the most critical part when handling Denial Code 226.
✅ Rule
📌 Calculate the time limit starting from the denial date.
If time limit is NOT crossed
➡️ Send the medical records immediately.
If time limit IS crossed
➡️ Write off the claim (because the payer may not accept records after the deadline).
Special Situation: Client May Still Want MR Sent
Sometimes, even if the deadline is crossed, the client may request sending the medical records anyway.
In those cases:
✅ Follow client instructions
✅ Submit medical records if possible
✅ Document clearly in notes that the time limit was crossed
Very Important: Always Check the Remark Code
Sometimes Denial Code 226 appears, but the remark code explains the exact issue, such as:
• Records were incomplete
• Provider sent incorrect documents
• Missing provider signature
• Notes do not support medical necessity
✅ Always verify the remark code and follow the AR Scenario Tool to proceed correctly.
Final Tips to Avoid Denial Code 226
To reduce these denials in the future:
• Submit requested medical records immediately
• Track document request deadlines
• Confirm the correct fax number or address
• Ensure complete documentation is sent
• Upload proof of submission
Conclusion
Denial Code 226 is mostly a documentation delay issue.
If you quickly confirm the denial date and submission deadline, you can still recover the claim by sending the medical records within the allowed time.