Denial Code 119: Benefit Maximum Reached (Simple Explanation + Call Handling Guide)
Denial Code 119 means:
✅ The patient has already used the maximum benefit allowed for that service during the policy period (year / lifetime / occurrence).
So the insurance will not pay for the service anymore.
This denial is also commonly explained as:
“Benefit maximum for this time period or occurrence has been reached.”
What Does “Benefit Maximum Reached” Mean?
Insurance policies usually set limits like:
• Maximum dollar limit per year/lifetime
Example: Insurance pays only up to $1,000 per year
• Maximum visit limit per year/lifetime
Example: Insurance pays only for 5 visits per year
When the patient crosses that limit, the claim gets denied with Denial Code 119.
Example 1: Dollar Limit Exhausted
Let’s say:
• Policy allows $1,000 per year
• Patient already used the same service 5 times
• Total paid amount = $1,000
Now, if the patient visits again:
❌ Insurance will deny the claim
✅ Reason: Maximum dollar benefit already reached
Example 2: Visit Limit Exhausted
Let’s say:
• Policy allows 5 visits per year
• Patient already completed 5 visits (paid by insurance)
Now for the next visit:
❌ Insurance will deny
✅ Reason: Maximum visits already reached
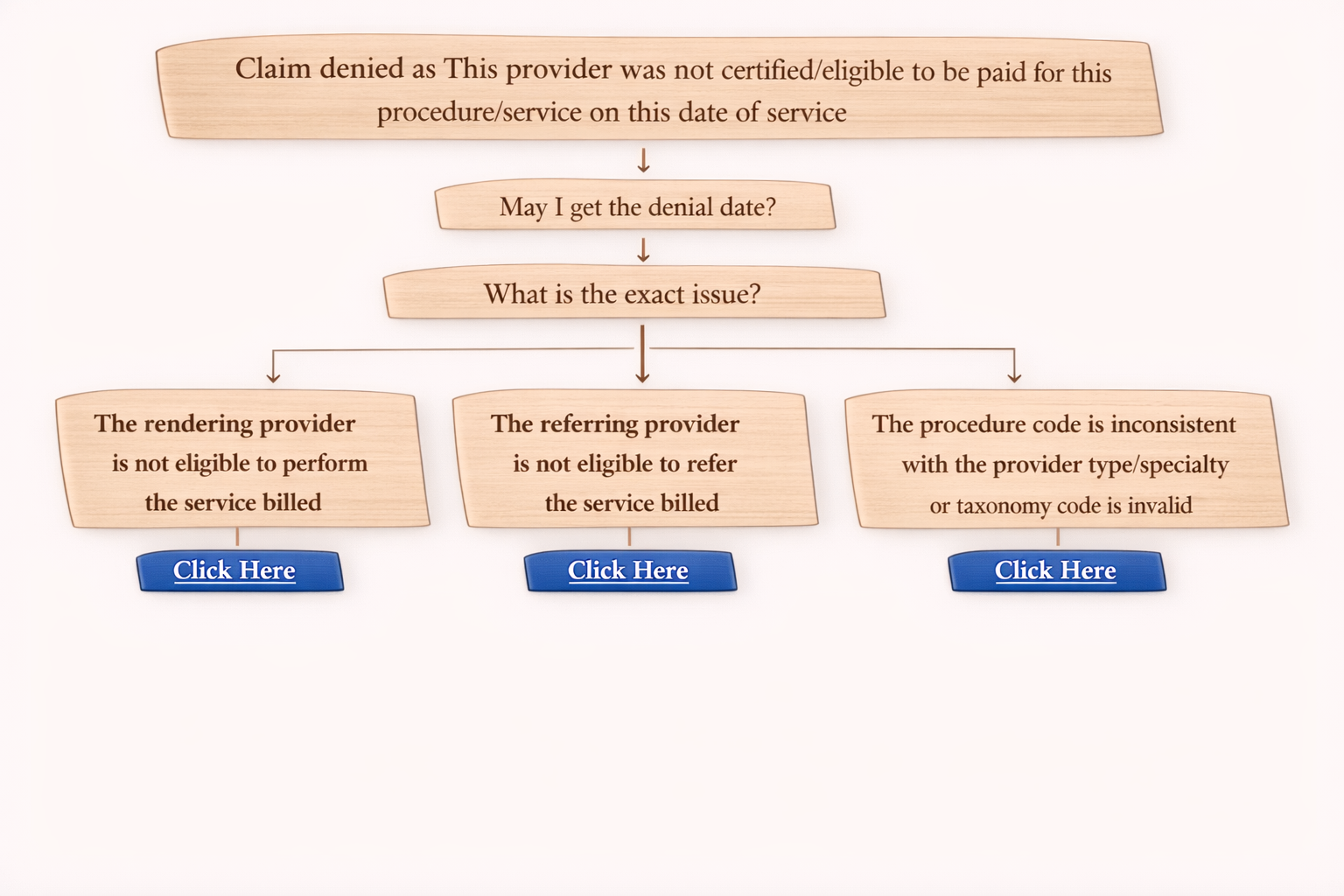
How to Handle Denial Code 119 (On-Call / Insurance Call Script)
When you see Denial 119, follow this simple call flow.
Step 1: Confirm Denial Details
✅ Ask:
- “Claim denied because patient reached maximum benefit allowed. May I get the denial date?”
- “Is the maximum benefit reached in terms of dollar amount or visit limit?”
If Denial is in Terms of Dollar Amount
Ask:
- “How much dollar amount is allowed?”
- “How much dollar amount has the patient met excluding this claim?”
- “Has the patient met the allowed amount excluding this claim?”
If YES (Patient already met limit)
✅ Action
• Request: Claim # and call reference #
• Bill claim to:
o Secondary payer, OR
o Patient (if no other payer)
If NO (Patient has NOT met limit)
✅ Action
• Ask rep to send the claim for reprocessing
• Ask: “What is the TAT for reprocessing?”
• Note down:
o Claim #
o Call reference #
o TAT
• Set follow-up for TAT date
If Denial is in Terms of Visit Limit
Ask:
- “How many visits are allowed?”
- “How many visits has the patient met excluding this claim?”
- “Has patient met the allowed visits excluding this claim?”
If YES (Patient already met visits limit)
✅ Action
• Request: Claim # and call reference #
• Bill to:
o Secondary payer, OR
o Patient
If NO (Patient has NOT met visit limit)
✅ Action
• Ask rep to reprocess the claim
• Ask: “What is the TAT?”
• Save claim/call ref
• Set follow-up for TAT
Important Notes & Actions (Must Follow)
1. If maximum benefit is reached
✅ Claim should be billed to:
• Secondary payer / consecutive payer
OR
• Patient (if no other payer available)
2. Verify secondary insurance eligibility
Before billing:
• Check payer portal (if available)
OR
• Call insurance
3. Do NOT change payer sequence
⚠️ Very important
When billing secondary:
✅ Keep payer sequence same
❌ Do NOT make secondary as primary
Reason:
• If you change sequence, primary denial/EOB will not go to secondary
• Secondary claim may deny as:
“Need Primary EOB”
4. If claim goes for reprocessing
✅ Always:
• Note the TAT provided by rep
• Set follow-up for that date
Conclusion
Denial Code 119 happens when the insurance benefit has been completely used, either by:
✅ Reaching the maximum dollar limit
OR
✅ Reaching the maximum visit count
To resolve:
• Confirm whether it’s dollar-based or visit-based
• Verify what has been used excluding this claim
• If limit is met → bill to secondary or patient
• If not met → request reprocessing and follow up