Denial Code 288: Referral Absent – Meaning, Reasons & How to Fix It (Complete Guide)
Referral-related denials are very common in medical billing, especially for HMO and POS plans. One of the most frequent referral denials is:
✅ Denial Code 288 – Referral Absent / Missing
In this guide, we’ll explain what Denial 288 means, why it happens, how to check referral details, and what steps to take to resolve the denial.
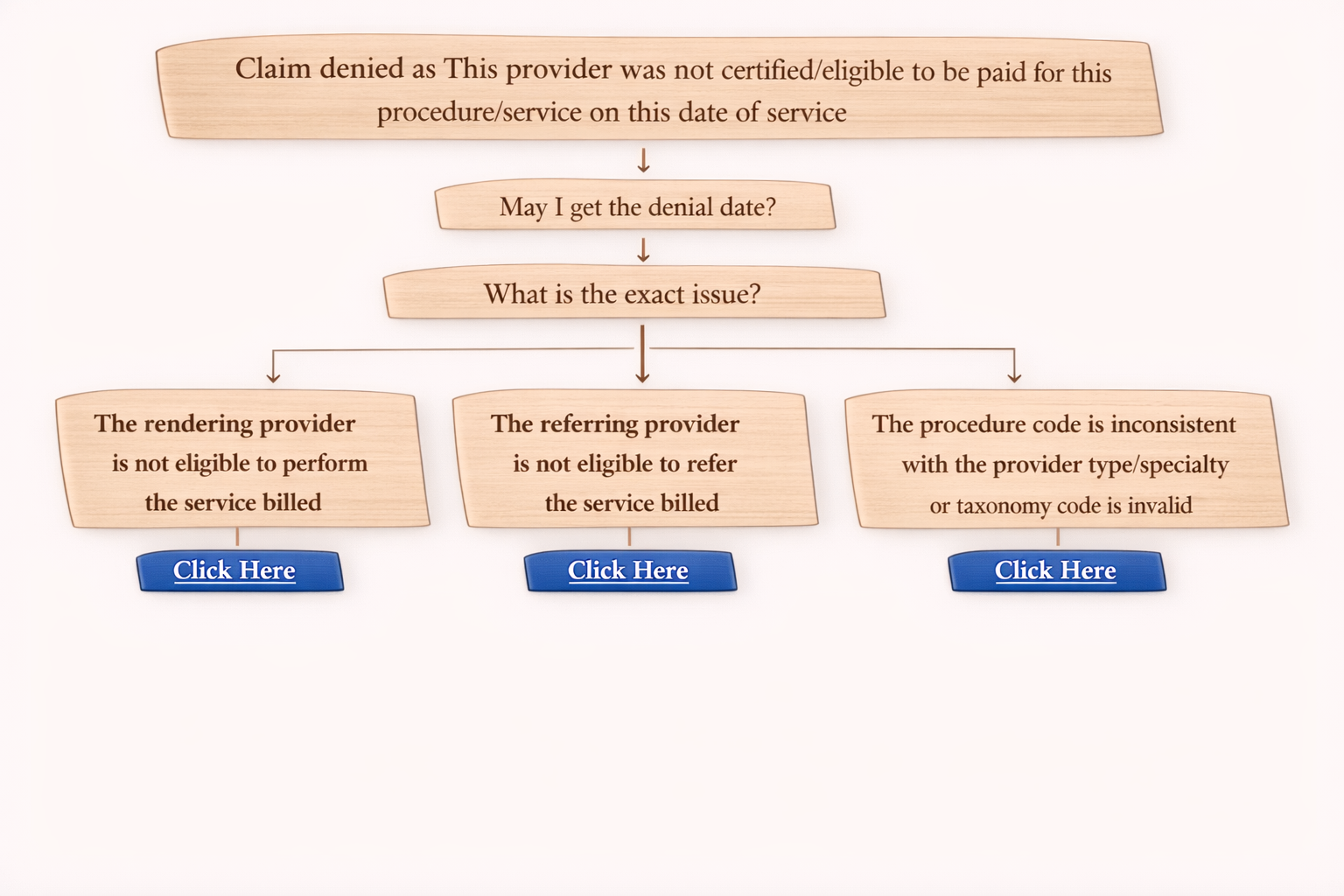
What is Denial Code 288 (Referral Absent)?
Denial Code 288 occurs when the insurance company denies a claim because the referral is missing.
A referral is a document or authorization provided by the Primary Care Physician (PCP) or Referring Provider, allowing the patient to visit a specialist.
When a required referral is not submitted or not found in the claim, the insurer denies the payment.
Where to Find the Referral Number on Claim Forms?
Referral numbers are usually present in the following areas:
✅ CMS1500 Form
📌 Box 23 – Prior Authorization / Referral Number
✅ UB04 Form
📌 Locator 63 – Treatment Authorization Codes
If these fields are blank or incorrect, the claim may deny with Code 288.
Why Does a Referral Become Mandatory?
Referrals depend mainly on the patient’s insurance plan type.
Plans that usually require referral:
✅ HMO (Health Maintenance Organization)
✅ POS (Point of Service)
These plans require the patient to visit PCP first. The PCP sends them to a specialist using a referral.
Plans that usually do NOT require referral:
✅ PPO (Preferred Provider Organization)
✅ EPO (Exclusive Provider Organization)
These plans allow the patient to visit a specialist directly — so referral is not mandatory.
Example of Referral Scenario
A patient visits their PCP for a regular check-up. The PCP identifies a skin problem and advises the patient to see a dermatologist.
In this case:
• PCP = Referring provider
• Dermatologist = Specialist
• Referral is required for HMO/POS plans
How to Fix Denial Code 288 (Step-by-Step Process)
When you receive a claim denial for referral missing, follow this structured approach.
Step 1: Confirm the Denial Date
Start the call with:
✅ “May I get the denial date?”
Step 2: Confirm the Patient Plan Type
Ask:
✅ “What plan does the patient have — HMO, PPO, EPO, or POS?”
This will decide the next action.
If the Plan is HMO or POS (Referral Required)
Since referrals are mandatory, you must confirm if referral exists.
Step 3: Check Referral in Your System
Ask internally or check system:
✅ Is referral number available?
If Referral is Available
Ask insurance rep:
✅ “I have the referral number, can you please reprocess the claim using it?”
Then ask:
• ✅ “What is the turnaround time?”
• ✅ “May I have the claim number & call reference number?”
Set follow-up based on TAT.
If Referral is NOT Available
Ask insurance rep:
✅ “Do you have the referral number on file?”
Also ask (only for non-hospital claims):
✅ “Is there any hospital claim billed on the same DOS where referral is present?”
If Referral Found in Rep System / Hospital Claim
Ask:
✅ “Could you please use the same referral number and send the claim back for reprocessing?”
Then ask:
• ✅ Turnaround time
• ✅ Claim number
• ✅ Call reference number
If Referral Not Found Anywhere
In this case, you have two options:
✅ Send Appeal OR
✅ Write off the claim
Ask rep:
• ✅ “What is the fax number or mailing address to send an appeal?”
• ✅ “What is the appeal filing time limit?”
• ✅ “May I have the claim number & call reference number?”
Follow your client’s SOP whether to appeal or write-off.
If the Plan is PPO or EPO (Referral Not Required)
In this scenario, the denial is incorrect because PPO/EPO typically do not require referral.
Ask the rep:
✅ “Could you please send the claim back for reprocessing since the patient plan does not require a referral?”
Then ask:
• ✅ “What is the turnaround time?”
• ✅ “May I have the claim number & call reference number?”
Set follow-up based on provided TAT.
Quick Important Notes (Must Follow)
✅ If plan is HMO/POS and referral is available → Request reprocessing + follow-up for TAT
✅ If plan is HMO/POS and referral is found by rep/hospital claim → Request reprocessing + follow-up
✅ If plan is HMO/POS and referral not found → Appeal or write-off based on client instructions
✅ If plan is PPO/EPO and rep agrees → Request reprocessing + follow-up for TAT
Conclusion
Denial Code 288 (Referral Absent) is easy to resolve once you identify:
- Plan type (HMO/POS vs PPO/EPO)
- Referral presence (your system / payer system / hospital claim)
- Correct next action (reprocess / appeal / write off)
Following the above call flow will help you handle referral denials confidently and reduce AR days.